Introduction
Closed isolated subtalar dislocations are very rare and forms a meager 1% of all lower limb injuries.1) Subtalar dislocation without any associated fracture is less described and fewer publications are available. Since its first description by Judcy et al in 1811,2 the major cause of subtalar dislocation remains to be road traffic accidents (43.7%) followed by falls from height and sports injury with 32.9% and 13.9% respectively.3) In this case report we present the rare presentation and diagnostic dilemma between medial subtalar dislocation and medial swivel dislocation and hence the management dilemma in isolated closed subtalar dislocation.
Case report
22-year-old male medical student came to the department of Emergency in mid-June 2021 with a complaint of severe pain and swelling in his left foot and heel. He gave history of accidentally putting his left foot down in a ditch in an attempt to balance his falling two-wheeler in a road traffic accident. He was brought within half an hour of his injury. He was unable to bear weight and had difficulty in moving his left ankle.
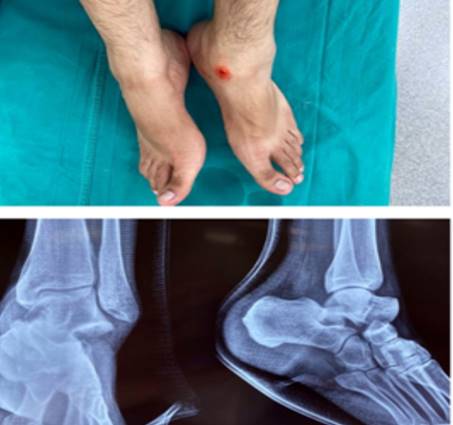
He was noted to have a deformed inverted left foot with minimal swelling and an abrasion on the medial aspect distal to the medial malleolus. Talus was palpable on the dorso-lateral side of the ankle, and rest of the foot inverted. No neurovascular deficits were noted. Radiographs revealed medial talocalcaneal and talonavicular dislocations with no obvious fracture (fig. 1).
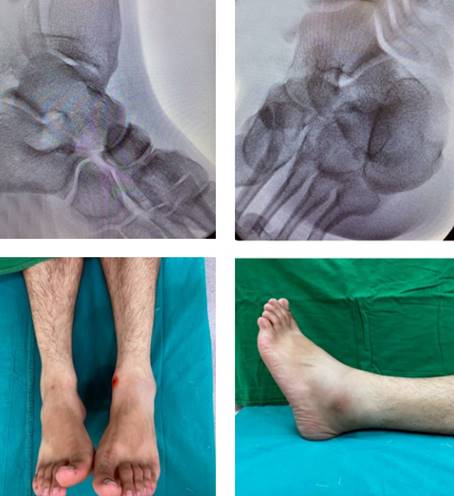
After taking informed consent he was taken up for closed reduction under sedation in operation theatre. Consent was also taken for open reduction if required. Manual traction was given along the direction of dislocation and the head of talus was pushed medially while bringing the foot to neutral with gentle eversion. The reduction was clinically felt with a clunk and visual reduction of the talar head which was confirmed with congruency of reduction of the subtalar and talonavicular joints under image intensifier (fig. 2).
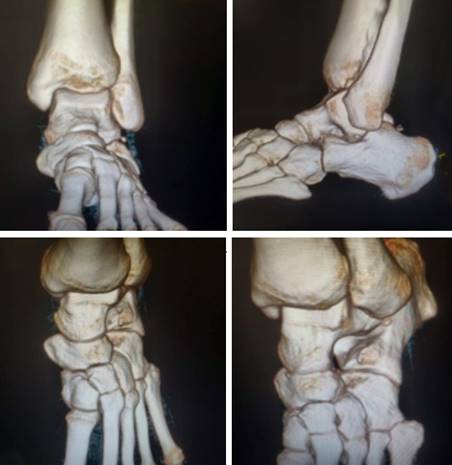
Reduction was stable with no distal vascular deficits. He was put on the posterior below knee POP slab for immobilization. Post reduction CT showed subtalar and talonavicular joints to be congruent with no associated fractures (fig. 3).
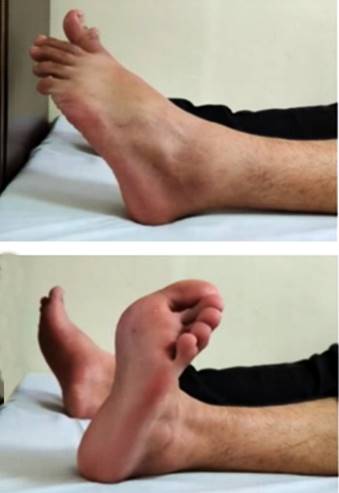
Post reduction the limb was kept elevated to avoid dependent oedema. Once the swelling subsided below knee synthetic cast was applied. Follow up radiographs taken at 2 weeks in July first week of 2021 showed no subluxation. He was allowed to mobilize without putting weight on the left lower limb with crutches till 4 weeks. After that, the cast was removed and partial weight bearing mobilization with active range of movements of ankle and foot were started in July 2021. Full weight bearing mobilization along with strengthening and proprioception exercises were started at 6 weeks according to new protocols in August 2021. At the end of one year of follow up in June 2022, patient had a very good functional outcome (AOFAS score 100) (fig. 4) and no radiological features of hind foot arthritis or avascular necrosis.
Discussion
In the year 1853, Broca classified subtalar dislocations on the basis of position of the dislocated foot, and its relation between talus and calcaneus into medial, lateral and posterior,4) later Malgaigne et al in 1856 added anterior.5 Medial dislocations are more common where the pivot is sustentaculum talus, there is lower incidence of talus avascular necrosis with good prognosis. After proper reduction the ligamentous dislocation has the best outcome in comparison to dislocations associated with fractures.6,7) Subtalar dislocation of joint differs from swivel injuries in that in swivel injuries deforming force most likely fall more anterior than subtalar injury deforming forces.8,9) In medial swivel injuries calcaneocuboid joint is intact but talonavicular joint subluxate medially due to the direction of deforming force is directed medially.10
Forced inversion, and equinus foot position leads to medial subtalar dislocation.6,7) When the inversion forces act on the foot, the strong calcaneonavicular ligament bears the stress and resists but the weaker talocalcaneal and talonavicular ligaments give away displacing the entire foot leading to subtalar dislocation. Here the sustentaculum tali act as a fulcrum point for medial subluxation or dislocation.
There is a need to differentiate among subtalar medial dislocation and medial swivel type of talo-navicular dislocation because traction and eversion reduces medial subtalar dislocation while traction along with lateral rotation of the foot will reduce swivel dislocation. Tibialis posterior tendon interposition or articular surface fractures of talus or navicular bone with impaction, cause hindrances to closed reduction, these interpositions are not found in dislocation of swivel type hence easier reduction and lesser need of open reduction.9 Hence it is necessary for the treating orthopaedician to be prepared for emergency open reduction if closed manoeuvres fail.
There is no consensus for the immobilization period following reduction of subtalar dislocations. However, in uncomplicated cases a protocol of early bearing of weight is advocated, following immobilization for a period of 3-4 weeks in below-knee cast.2 In other situations of complicated dislocation like with instability and fractures, the external fixator or k wires crossing and stabilizing the joint is advisable; hence immobilising for 6-12 weeks.2
In around 10% of closed dislocations and around 50% in open dislocations osteonecrosis might be seen as a complication. Most common complication of subtalar dislocations are posttraumatic arthritis of sub talar joint with rates around 60%.11 The subtalar joint chronic instability is rare and mostly attributable to inadequate immobilization.4
Conclusions
Excellent outcomes can be expected if closed reductions are done immediately following injury. There is a need to identify the difference between medial dislocation and medial swivel injury which have different mechanisms as well as different reduction manoeuvres. If the closed reduction fails, then with suspicion of tendon incarceration open reduction must be done and additional stabilization is required if the reduction is unstable.