Mi SciELO
Servicios Personalizados
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Revista de Ciencias Médicas de Pinar del Río
versión On-line ISSN 1561-3194
Rev Ciencias Médicas vol.27 no.1 Pinar del Río ene.-feb. 2023 Epub 01-Ene-2023
Articles
Total cardiovascular risk category in hypertensive patients
1University of Medical Sciences of Pinar del Rio. Municipal Health Directorate. Los Palacios, Pinar del Río, Cuba.
2University of Medical Sciences of Pinar del Rio. University Polyclinic Elena Fernández Castro. Los Palacios, Pinar del Río, Cuba.
Introduction:
The relationship of blood pressure and risk of cardiovascular events is independent of other risk factors and when hypertension coexists with other factors, it can be enhanced, resulting in a higher total cardiovascular risk than the sum of its individual components.
Objective:
to determine the total cardiovascular risk in hypertensive patients in clinic 12 of the Los Palacios municipality during the year 2022.
Methods:
descriptive and cross-sectional study; universe 203 hypertensive patients aged 18 years and older; sample 183 patients with a diagnosis of arterial hypertension who met the inclusion criteria. Summary measures were used for qualitative data.
Results:
female sex (67,2 %) and age 60 years and older (57,4 %) predominated; family history of hypertension, sedentary lifestyle and obesity prevailed as risk factors. Forty-three percent were classified as moderate risk. The relationship between pulse pressure greater than 60 mm Hg and cardiovascular disease was highly significant.
Conclusions:
the moderate and high total cardiovascular risk categories predominated in hypertensive patients, so it is necessary to work with the identified risks for better prevention and control.
Key words: HEART DISEASE RISK FACTORS; HYPERTENSION; PATIENT.
INTRODUCTION
The relationship of blood pressure and risk of cardiovascular and cerebrovascular disease events is continuous, consistent and independent of other risk factors.1 The higher the blood pressure, the greater the chance of myocardial infarction, heart failure, stroke and renal disease. The need to reduce morbidity and mortality from cardiovascular disease is the main reason for approaching the problem of hypertension control from a more comprehensive point of view and not just focusing on blood pressure figures as the main variable for deciding the need for and type of treatment.(1,2
The therapeutic strategy should take into account the total cardiovascular risk, in addition to blood pressure levels, to maximize cost-effectiveness in the treatment of arterial hypertension. The prevention of cardiovascular diseases in hypertensive patients should be adapted to their total cardiovascular risk; the higher the risk, the more intensely the strategy should be applied to control and reduce it.3,4
In Cuba there are no large cohort studies whose final objective is to evaluate the influence of a given cardiovascular risk factor on cardiovascular mortality. Given this limitation, the Cuban Hypertension Guidelines,1 propose using a modification of the Framinhgan, World Health Organization and Systematic Coronary Risk Evaluation models in which total cardiovascular risk is stratified into different categories based on blood pressure, cardiovascular risk factors, asymptomatic organ damage or target organ lesion and the presence or absence of diabetes mellitus, and total cardiovascular risk is classified into low, moderate and high. Therefore, it is recommended that all hypertensive patients should have their total cardiovascular risk stratified in the initial evaluation in order to decide the type and intensity of the therapeutic strategy to be used.1
The municipality of Los Palacios, like the rest of the country, has among its main causes of death cardiovascular diseases in which arterial hypertension plays a fundamental role. For this reason, based on the Cuban Guide for the diagnosis, evaluation and treatment of arterial hypertension,1 it is necessary to determine the total cardiovascular risk of hypertensive patients and thus be able to design prevention and control strategies aimed at modifying and/or eliminating the risk factors detected.
METHODS
A descriptive and cross-sectional study was carried out in clinic 12 of the Elena Fernández Cas-tro polyclinic in the municipality of Los Palacios during the year 2022.
Universe and Sample
The population was represented by all patients aged 18 years and older with a diagnosis of arterial hypertension belonging to clinic 12 of the Elena Fernández Castro polyclinic, Los Palacios municipality in the year 2022 (203 patients), from which a sample of 183 patients was obtained who met the following inclusion criteria:
Informed consent
40 years of age or older
No mental illness that would prevent cooperation with the study.
Exclusion criteria: Not meeting the inclusion criteria.
B. Variables:
Age, sex, risk factors, pulse pressure, cardiovascular risk category.
Pulse pressure: 1 Differential between systolic blood pressure (SBP) and diastolic blood pressure (DBP). Pulse pressure above 60 mm Hg is considered an independent marker of total cardiovascular risk.
Risk category 1
Low risk: hypertensive patient with no additional cardiovascular risk factors and arterial blood pressure grade 1; prehypertensive patient with one or two additional risk factors.
Moderate risk: hypertensive patient without additional cardiovascular risk factors and blood pressure grade 2; patient with one or two cardiovascular risk factors and blood pressure grade 1 or 2; prehypertensive patient with three or more cardiovascular risk factors or with diabetic or diabetic organ damage.
High risk: patient with no other cardiovascular risk factors and blood pressure grade 3; patient with one or two cardiovascular risk factors and blood pressure grade 3, and patient with three or more cardiovascular risk factors or with target organ damage or diabetes mellitus and any blood pressure grade.
The data were taken from the individual medical records, which reflected the interrogation, physical and complementary examinations performed on the patients.
Ethical considerations: All data were handled by health personnel with prior authorization from the responsible managers and their use was intended for scientific purposes only.
RESULTS
The predominant age group was 60 years and older (57,4 %) and female sex (67,2 %). Table 1
Table 1: Hypertensive patients according to age and sex. Clinic 12. Los Palacios 2022
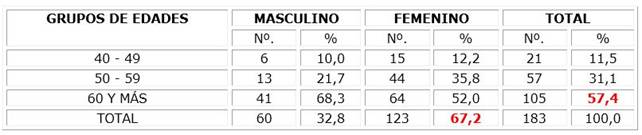
Source: Individual medical history
Among the cardiovascular risk factors, family history of hypertension predominated (66,6 %), followed by sedentary lifestyle and obesity (Table 2).
Table 2: Risk factors present
| RISK FACTORS (N =183) | No. | % |
|---|---|---|
| Family history of hypertension | 122 | 66,6 |
| Sedentary lifestyle | 83 | 45,3 |
| Obesity | 39 | 21,3 |
| Smoking | 32 | 17,5 |
| Dyslipidemia | 30 | 16,4 |
| Diabetes | 23 | 12,6 |
| Alcoholism | 12 | 6,6 |
Source: Individual medical history
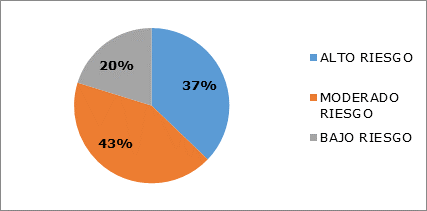
Moderate (43 %) and high risk (37 %) prevailed in the sample studied (Graf. 1).
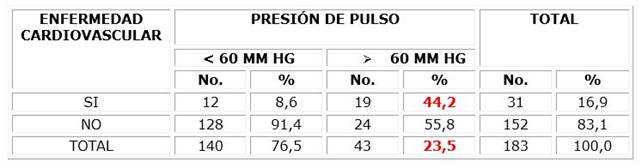
23,5 % of the patients showed elevated pulse pressure and of these, 44,2 % had cardiovascular disease (table 3), which was highly significant.
DISCUSSION
From the sociodemographic point of view, regarding the prevalence of the female sex Paramio Rodrí-guez A et al.5 presented similar results while other studies show data that are not related to what was presented.2,6,7 Among the non-coincidental Rivera Ledesma et al.,6 point out in their research how the percentage of the male sex was significantly higher than that of the female group, showing also how the average probability of developing a cardiovascular epi-sodium was significantly higher in men than in women. Regarding sex, it should be pointed out that most of the studies indicate that the male sex predominates in morbidity until menopausal ages,2,6,7) when the estrogenic protective factor disappears in women, and the possibilities are equal in both sexes after menopause, given that in the sample the postmenopausal ages prevailed, this may have influenced the superiority of the female sex.
In relation to the age factor, it is recognized that age by itself increases the absolute risk of suffering from cardiovascular disease as a result of the progressive accumulation of coronary atherosclerosis.6) Gonzáles de la Fé et al,7 in this regard, showed a predominance in older adults similar to that found in the present study.
The findings regarding risk factors are partly consistent with studies such as that of Hierrezuelo Rojas N et al.,4) where sedentary lifestyle and stress predominated; while a study carried out in Holguín by Cobiellas and Anazco8 showed that the magnitude of the estimated risk is higher in smokers and obese people. Internationally, several studies,9,10,11 have shown the strong influence of all these risk factors on the progression of HT and the occurrence of major cardiovascular events.
The stratification of cardiovascular risk by means of scales is a fundamental pillar for making therapeutic decisions in primary health care.
At the individual level, special attention should be paid to those who showed the highest risks, as they deserve priority preventive and health care actions that will lead to their control and better cardiovascular health.
The calculation or determination of CVR is a useful element for assessing the cardiovascular health of subjects and populations. It is necessary to seek strategies to achieve a better acceptance of the recommendations, to induce favorable changes in the individual's lifestyle and to generate public actions to promote health and reduce the levels of risk factors present in the community.12,13
The evaluation of cardiovascular risk is essential in the Cuban population, because it will contribute to the care and management of the factors that determine it, and will result in the reduction of morbimortality due to cardiovascular diseases, which are the leading cause of death in Cuba.14
Different studies have shown that the elevation of pulse pressure is a marker of cardiovascular events in both normotensive and hypertensive populations.1,15
Table 3 shows that about 25 % of the patients had elevated pulse pressure and of these, 44,2 % had cardiovascular disease, which was highly significant.
Indeed, in recent years, pulse pressure has been shown to be an independent marker of cardiovascular risk in processes such as myocardial hypertrophy, coronary heart disease, acute myocardial infarction, heart failure, carotid artery stenosis, ischemic stroke, end-stage renal disease, cardiovascular mortality, including in the normotensive population, and total mortality. The frequency of these complications increases with the increase in pulse pressure.15
The results obtained have shown that the moderate and high total cardio-vascular risk category predominated in the patients, the sociodemographic characteristics were identified, the risk factors present and the existence of an association between elevated pulse pressure and cardiovascular disease was demonstrated, all of which will make it possible to draw up prevention and control strategies aimed at modifying and/or eliminating the risk factors detected.
BIBLIOGRAPHIC REFERENCES
1. Ministerio de Salud Pública. Guía para el diagnóstico, evaluación y tratamiento. Comisión Nacional Técnica Asesora del Programa de Hipertensión Arterial. Habana; Editorial Ciencias Médicas[Internet]; 2018 [Citado 13/06/2021]. 103 p. Disponible en: Disponible en: http://www.bvscuba.sld.cu/libro/hipertension-arterial-guia-para-el-diagnostico-evaluacion-y-tratamiento/ 1. [ Links ]
2. Díaz-Esquivel, Aymeé María et al. Estimación del riesgo cardiovascular en pacientes hipertensos. Policlínico Docente Universitario Luis Augusto Turcios Lima, 2021. Rev Ciencias Médicas[Internet]. feb. 2022 [Citado 13/06/2021]; 26(1): e5365. Disponible en: Disponible en: http://www.revcmpinar.sld.cu/index.php/publicaciones/article/view/5365 2. . [ Links ]
3. . Díaz Piñera A, Rodríguez Salvá A, García Roche R, Carbonell García I, Achiong Estupiñán F. Resultados de una intervención para la mejora del control de la hipertensión arterial en cuatro áreas de salud. Rev Finlay [Internet]. 2018 [Citado 13/06/2021]; 8(3): 180-9. Disponible en: Disponible en: http://scielo.sld.cu/scielo.php?script=sci_arttext&pid=S2221-24342018000300002 3. [ Links ]
4. Hierrezuelo Rojas N, Álvarez Cortés JT, Monje Labrada A. Estimación del riesgo cardiovascular en adultos mayores con hipertensión arterial. MEDISAN [Internet]. 2021 [Citado 13/06/2021]; 25(3): 566-579. Disponible en: Disponible en: http://scielo.sld.cu/scielo.php?script=sci_arttext&pid=S1029-30192021000300566 4. [ Links ]
5. Paramio-Rodríguez A, Aguilera-García L, Carrazana-Garcés E, Hernández-Navas M. Riesgo cardiovascular global en tres casas de abuelos del municipio Boyeros. Rev Cubana Med Gen Integr [Internet]. 2021 [citado 20/03/2022]; 37(4). Disponible en: Disponible en: http://www.revmgi.sld.cu/index.php/mgi/article/view/1417 5. [ Links ]
6. Rivera Ledesma E, Bauta León L, González Hidalgo JA, Arcia Chávez N, Valerino Meriño I, Placencia Oropeza E. Categoría de riesgo de enfermedad cardiovascular. Rev Cubana Med Gen Integr [Internet]. 2017 [Citado 13/06/2021]; 33(4): [aprox. 7 p.]. Disponible en: Disponible en: http://scielo.sld.cu/scielo.php?pid=S0864-21252017000400004&script=sci_arttext&tlng=en 6. [ Links ]
7. González de la Fé R, Casado Méndez PR, Santos Fonseca RS, Mustelier Sánchez RM, Remón Elías M. Evaluación del riesgo cardiovascular global en población adulta del Consultorio Médico 21. Multimed [Internet]. 2017 [Citado 13/06/2021]; 21(6). Disponible en: Disponible en: http://www.revmultimed.sld.cu/index.php/mtm/article/view/673/1045 7. [ Links ]
8. Cobiellas Carballo LI, Anazco Hernández A. Estimación del riesgo cardiovascular en pacientes hipertensos del reparto Santiesteban del municipio Holguín. 16 de Abril [Internet]. 2020 [Citado 13/06/2021]; 59(275): 865-872. Disponible en: Disponible en: http://www.rev16deabril.sld.cu/index.php/16_04/article/view/865 8. . [ Links ]
9. Anh Hien H, Tam NM, Tam V, Van Minh H, Hoa NP, Heytens S, et al. Estimation of the cardiovascular risk using world health organization/international society of hypertension risk prediction charts in Central Vietnam. PLoS ONE [Internet]. 2020 [Citado 13/06/2021]; 16(12): e0261099. Disponible en: Disponible en: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0242666 9. [ Links ]
10. Leiva AM, Petermann Rocha F, Martínez Sanguinetti MA, Troncoso Pantoja C, Concha Y, Garrido Méndez A, et al. Asociación de un índice de estilos de vida saludable con factores de riesgo cardiovascular en población chilena. Rev. méd. Chile [Internet]. 2018 [Citado 13/06/2021]; 146(12): 1405-1414. Disponible en: Disponible en: https://scielo.conicyt.cl/scielo.php?script=sci_arttext&pid=S0034-98872018001201405 10. [ Links ]
11. Pan J, Wu L, Wang H, Lei T, Hu B, MSa, et al. Determinants of hypertension treatment adherence among a Chinese population using the therapeutic adherence scale for hypertensive patients. Medicine [Internet]. 2019 [Citado 13/06/2021]; 98(27): e16116. Disponible en: Disponible en: http://doi.org/10.1097/MD.0000000000016116 11. [ Links ]
12. Hechavarría Matos S, Montes de Oca Carmenaty M, Chaveco Bello LL, Hernández Lin T. Estimación del riesgo cardiovascular total en pacientes con hipertensión arterial. Inmedsur [Internet]. 2020 [Citado 13/06/2021]; 3(1): 23-31. Disponible en: Disponible en: http://www.inmedsur.cfg.sld.cu/index.php/inmedsur/article/view/58 12. [ Links ]
13. Revueltas-Aguero M, Valdés-González Y, Serra-Larín S, Suárez-Medina R, Ramírez-Sotolongo J, Betancourt-Bethencourt J. Evaluación del riesgo cardiovascular en una muestra poblacional con dos tablas predictivas en La Habana. Rev Cubana Med Gen Integr [Internet]. 2022 [citado 20/03/2022]; 38(1) Disponible en: Disponible en: http://www.revmgi.sld.cu/index.php/mgi/article/view/1650 13. [ Links ]
14. Varona Pérez P, Armas Rojas N, Suárez Medina R, Bonet Gorbea M, Dueñas Herrera A. Estimación del riesgo cardiovascular en la población cubana. Una aproximación al tema. Rev Cubana Cardiol Cir Cardiovasc. 2015 [acceso: 20/07/2020]:21(4). Disponible en: Disponible en: http://www.revcardiologia.sld.cu/index.php/revcardiologia/article/view/606/pdf_26 14. . [ Links ]
15. Hernández Gárciga FF, González Chacón Y. Presión del pulso y su relación con el riesgo cardiovascular incrementado. Rev Cubana Invest Bioméd [Internet]. 2015 Sep [citado 03/12/2019]; 34(3). Disponible en: Disponible en: http://scielo.sld.cu/scielo.php?script=sci_arttext&pid=S0864-03002015000300005&lng=es 15. [ Links ]
Received: November 09, 2022; Accepted: December 17, 2022











 texto en
texto en