INTRODUCTION
In recent years, periodontal disease (PD) has been widely studied due to its significant relationship with health. It emerges as a manifestation of systemic disorders, influences the etiology of diverse general diseases, and shares risk factors with current major chronic illnesses, such as cardiovascular,1 rheumatic, renal, and neurological diseases - including Alzheimer's and Parkinson's,2,3 cancer, chronic respiratory diseases,4,5 obesity6 and diabetes,7,8 among others.9,10,11,12,13 As a result of this relationship, and the aging population, an increase in the prevalence of periodontopathies, which in turn are the main cause of dental loss, is expected. Several studies associate edentulism with negative effects at the systemic level.14,15,16
The self-reported periodontal disease (SPD) has acceptable validity when compared to clinical excellence standards. Regarding painful gums, dental mobility, and people's opinions about whether they have gum disease, it can be classified as moderately to highly valid, according to Nelson's validity classification.17
On March 11th, 2020, the World Health Organization declared the COVID-19 pandemic,18 caused by a novel coronavirus SARS-COV-2. It produces pulmonary damage and other organ failures, and like PD, features an exacerbated immune-inflammatory response, resulting in an excessive host immune reaction with cytokine storming, which is closely related to severity in the presence of chronic non-communicable diseases.6,10,18,19,20
The severity spectrum of COVID-19 ranges from asymptomatic to severe. While a significant proportion of SARS-CoV-2 positive individuals do not manifest symptoms or have only mild ones, some become seriously ill and develop a hyperinflammatory response leading to dysregulation of the involved organ metabolism, with potentially life-threatening consequences. Overall, the severity of COVID-19 increases with pre-existing comorbidities.21 In this context, several hypothetical mechanisms may explain the strong associations observed between PD and COVID-19 severity.20,22,23,24,25
Up to the completion date of this research, there was no scientific evidence of SDP studies in Cuba, nor any antecedents of studies related to COVID-19 in adults over 60. For this reason, this research aims to determine the relationship between SDP, dental loss, and COVID-19 activity.
This research aims to determine the relationship between self-reported periodontal disease, dental loss, and COVID-19 activity.
METHODS
Type of study: A cross-sectional descriptive research was conducted from April to September 2021. It was approved by the Ethics Committee of the Faculty of Stomatology at University of Medical Sciences of Havana as the main subject of the master's studies of one of the authors.
Inclusion and sample criteria: The sample consisted of 238 individuals aged over 60, who were infected with COVID-19 and survived it, from March 11th, 2020 to March 11th, 2021, and lived in Playa municipality in Havana, Cuba. They were all confirmed positive cases for COVID-19 according to the PCR test (Polymerase Chain Reaction).
Variables: The study variables were defined by gender (male/female), age groups (60-75 and 76-100), evolutionary severity of COVID-19 (asymptomatic, symptomatic, and severe), comorbidities (hypertension, diabetes mellitus, heart disease, chronic respiratory disease, and morbid obesity), dental loss (teeth and edentulous), and SPD (absence and presence of PD and presence of advanced periodontal disease (APD)).
Techniques and procedures: Credentials were submitted to governmental institutions to access the data required to develop the research. Then, personal data were collected from patients confirmed as COVID-19 positive. Individuals were presented with a 4-question survey to identify the presence of periodontal disease. This survey was validated in New Zealand,26 and translated into Spanish for its usage. First, the absence of PD was determined when all four answers were negative; then, the presence of PD was determined in cases with two positive answers and if only the fourth one was also positive. Finally, the presence of SPD was determined when answers 2,3, and 4 were positive.
All data were collected through a Google form and stored in a database. General information, personal pathological background, and edentulous or dentate status were also recorded. All participants were visited and surveyed at their homes. All health protocol measures required by the relevant health organizations were followed, and the required protective equipment was used.
Data processing and analyses: Data regarding the evolutionary severity of COVID-19, the PD, and the SPD were dichotomized to process all variables and perform Pearson's odds ratio and the chi-square test. It aimed to determine the connection between their relationship (as possible risk factors) and the evolutionary severity of COVID-19. There was a 95 % confidence interval defined to establish this relation; besides, the p-value had to be less than 0.05 or equal to it to show any significance. All data were processed using Excel databases and imported into IBM SPSS® Statistics 25 for Windows. All statistical tests applied to the primary endpoints were assessed with a 95 % confidence interval. Similarly, this database is available in the Zenodo repository based on the principles of open sciences.27
Ethical aspects: The mediating institutions authorized using patient data through the official research document. All individuals received the informed consent document as per the Helsinki principles, which they signed voluntarily, and their identity and privacy were protected. They were informed of receiving information about the research results after its publication.
RESULTS
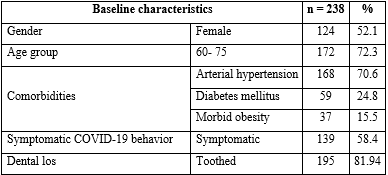
The population studied showed a slight predominance of female participants, and 72.3 % belonged to the early old age group. Among the comorbidities, there was a high prevalence of arterial hypertension (70.6 %), followed by diabetes mellitus and obesity. More than half of the total (58.4 %) had COVID-19 clinical symptoms, and a significant percentage of patients (81.9 % of the total) preserved their teeth despite their age (table 1).
The self-reported results of periodontal disease, even advanced periodontal disease, were high (between 48.7 % and 45.6 %) and did not have a statistically significant relationship regarding the evolutionary severity of COVID-19. This was evidenced by the ODDS ratio values and their confidence intervals 1.598 (0.261; 9.78) and 1.814 (0.296; 11.105) respectively, as well as the p-value of 0.609 and 0.514 for each of them. Besides, more than half of all of people affected by SPD presented clinical symptoms derived from COVID-19.
Dental loss p-values results were less than 0.05, and edentulous patients were statistically significant, suggesting the teeth loss as a risk factor for the evolutionary severity of COVID-19 with an ODDS ratio of 3.897 and confidence intervals between 1.001 and 15.173; supported by the p-value equal to 0.036 (table 2).
Likewise, there was a significant relationship between respiratory diseases and the severity of COVID-19, with an odds ratio of 6,833 and confidence intervals between 1,717 and 27,192 (table 2).
Table 2 Self-reported Periodontal Disease, dental loss, comorbidities and evolutionary severity of COVID-19
| Variables | Total n= 238 | Severe n= 9 | Not severe n= 229 | OR (IC 95%) | |
|---|---|---|---|---|---|
| SPD | 95 (48.7) | 5 (5.26) | 90 (94.38) | 1.598 (0.261; 9.78) | 0.609 |
| SPD (advanced) | 89 (45.6) | 3 (3.37) | 86 (96.6) | 1.814 (0.296; 11.105) | 0.514 |
| Toothed patients | 195 (81.9) | 5 (2.5) | 190 (97.5) | 0.257 (0.066; 0.999) | 0.036 |
| Edentulous patients | 43 (18.1) | 4 (9.3) | 39 (90.7) | 3.897 (1.001; 15.173) | 0.036 |
| Arterial hypertension | 168 (70.5 %) | 8 (88.9 %) | 160 (69.9) | 3.45 (0.423; 28.115) | 0.219 |
| Diabetes mellitus | 59 (24.8) | 4 (44.4) | 55 (24.0) | 2.531 (0.657; 9.756) | 0.164 |
| Heart diseases | 31 (13.0 %) | 1 (11.1) | 30 (13.1) | 0.826 (0.100; 6.867) | 0.862 |
| Respiratory diseases | 28 (11.8) | 4 (44.4) | 24 (10.5) | 6.833 (1.717; 27.192) | 0.002 |
| Morbid obesity | 37 (15.5) | 3 (33.3) | 34 (14.8) | 2.868 (0.684; 12.019) | 0.133 |
DISCUSSION
Dental loss might represent a risk factor contributing to the severity of COVID-19; however, there is no documented evidence in other articles connecting both situations. Recent studies suggest an association between edentulous diagnosed patients and lower respiratory capacity, a high incidence of chronic obstructive pulmonary diseases, greater susceptibility to hospitalizations due to pulmonary conditions, and even a higher risk of mortality derived from pneumonia, than toothed patients.16,28,29,30,31 The biological mechanism relating the periodontal disease, dental loss, and edentulism to chronic diseases involves a local and systemic inflammation due to endothelial dysfunction, together with micro and macro-vascular impairment. In general, people with systemic diseases, elderly or not, have a weakened immune response.14,28,32,33
The relationship between the presence of respiratory diseases and the severity of COVID-19 was reaffirmed. It has been seen that, while suffering from COVID-19, patients with pre-existing respiratory illnesses have had an increased risk of serious complications and some have even died.34,35,36,37 The underdiagnosis of all chronic respiratory diseases has been a universal characteristic, and despite reporting low prevalence among all chronic non-communicable diseases, according to Signes-Costa et al.38 is the one with the greatest statistical relevance.34
Although the expected association between SPD and COVID-19 was not detected, recent studies from Qatar and England suggest an increased risk of severity, hospitalization, and death from COVID-19 when patients have periodontal disease.39,40 This can be attributed to the lack of traditional procedures used for diagnosis, a limitation that all self-reported measures share when compared to the results of periodontal probing and radiographic examinations. Self-reported methods had a desirable use considering the epidemiological situation. Besides, the relationship among high blood pressure, diabetes mellitus, obesity, cardiovascular diseases, and the severity of COVID-19 were significant in this study, which differs from other results of several studies carried on in Cuba and the world.41,42,43,44,45 This can be attributable to the low percentage of critically ill patients who made up the sample.
Self-reported diagnostic methods stated the presence of PD and can be used for epidemiological purposes. There is no relationship between SPD and the evolutionary severity of COVID-19 in the population studied. However, a relationship is observed targeting dental loss and respiratory diseases as determinant risk factors in the severity of COVID-19.