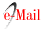Introduction
Haploidentical transplantation with the use of post-transplant cyclophosphamide is an effective therapeutic option for patients with hematologic diseases that do not have an identical histocompatible donor. This procedure is mainly associated with greater immunosuppression that increases the appearance of infectious complications of bacterial and viral etiology.
Reactivation of viruses of the polyomavirus family (PV) such as BK and JC viruses cause serious complications in TPH receptors, with hemorrhagic cystitis (HC) being one of the most frequent and lethal, with an incidence rate that varies between 13 and 70% according to the different series.1,2 BK virus infection is acquired asymptomatically by airborne transmission at early ages and it has the ability to persist in the uroepithelium. HC is caused by viral reactivation and replication in urinary tissue. The condition usually begins between three and six weeks post-transplant - unlike HC, where the metabolites of cyclophosphamide used in conditioning are of earlier onset - and it is characterized by dysuria, hematuria and kidney damage.3
Human papilloma virus (HPV) is the etiologic agent of dermatological and other sexually transmitted diseases, as well as cervical cancer and other tumors.4) The possibility of acquiring the infection at least once is 50% for both sexes, although it is controlled by the immune system.5 The proliferation of HPV due to post-transplant immunosuppression favors the appearance of condyloma acuminata of the anus, a tumor mass of variable size that causes anal pain and the treatment of choice is surgical resection.6
Here, we present a unique case, where both entities are associated in a haploidentical TPH receptor. The clinical symptoms, management and evolution of the patient are further described.
The case
A 20-year-old male patient diagnosed with acute myeloid leukemia (M1 according to FAB classification). He was treated with a 3-8-3 induction scheme (rubidomycin, cytosar and etoposide) and three consolidation cycles with high doses of cytosar prior to the haploidentical transplantation of peripheral blood from his brother. Conditioning regime consisted of fludarabine, cyclophosphamide, and busulfan with post transplantation cyclophosphamide at 50 mg/kg on days + 3 and + 4. Cyclosporine and mycophenolate mofetil (MMF) were used from day + 5. The engraftment occurred on day + 14.
On day + 21, the patient began with suprapubic pain, dysuria, and gross hematuria with the presence of clots that forced the use of permanent cystoclysis. Creatinine rose to 209 mmol/L. The renal ultrasound showed no alterations. The result for BK virus in urine using the polymerase chain reaction technique was positive.
Treatment consisted of hydration, furosemide, antibiotics, blood and platelet transfusion. Four doses of intravesical Heberprot P, a medication based on recombinant epidermal growth factor (rhEGF) developed at the Center for Genetic Engineering and Biotechnology (CIGB, the Spanish acronym) in Havana, was also given with no improvement in symptoms. The patient received seven sessions of hyperbaric oxygen with which the hematuria disappeared.
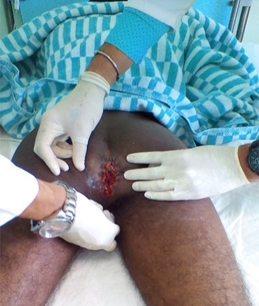
On day + 59 post-transplant, pain and itching appeared in the perianal region. Examination revealed a cauliflower-like vegetative mass of 5 cm in diameter, protruding from the anal region (Fig.1). A biopsy of the lesion reported condyloma acuminatum.
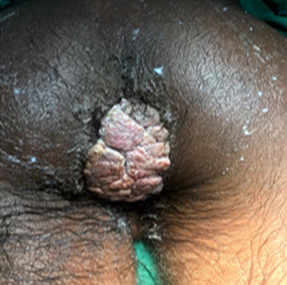
Fig. 1 Photography of the patient at the moment of diagnosis. Perianal exophytic mass consistent with anal condyloma.
The case was consulted with the coloproctology service and tumor excision was performed.
The patient evolved satisfactorily and was discharged (Fig.2).
Discussion
In Cuba, the true incidence of HC by viruses after TPH is unknown. The incidence varies between 13-70% worldwide which is due to the great heterogeneity of the samples and the different conditioning schemes used.1,2 A recent study carried out in children showed up an incidence of 20.7% of HC in 29 patients,7 whereas another investigation in 500 adult patients showed up only 10.4%.8
Condyloma acuminatum of the anus due to HPV infection after TPH has a very low incidence condition (0.3-1.3%).6 Between 1997 and 2005, 312 allogeneic transplants were performed at the University of Kansas Medical Center and only one patient presented giant condyloma of the anus.4 As far as we know, the association of giant condyloma of the anus due to HPV infection and HC with BK virus in a haploidentical TPH receptor has not been reported yet.
There are many studies on the risk factors for contracting these infections in the recipient of a TPH, such as male sex, age over 10, HLA histocompatibility, among others. In the Pérez-Huertas study, after a multivariate analysis, it was found that factors such as age over 10 years, and positive IgG for Epstein Barr; maintained statistical significance.7 The myeloablative conditioning regimen and the use of tacrolimus instead of cyclosporine as part of the prevention regimen to avoid transplant rejection were other risk factors in a group of 161 patients.9 Haploidentical TPH with the administration of post-transplant cyclophosphamide to prevent graft-versus-host disease is another risk factor.10Solomon et al. found a 75% incidence of HC for BK associated with the use of post-transplant cyclophosphamide in haploidentical transplants, while Raiola et al. reported 40%.11.12
In this patient, several of the mentioned risk factors concur, such as age, male sex, haploidentical transplant with the use of post-transplant cyclophosphamide and the myeloablative-conditioning regimen.
The case presented grade IV hematuria based on the classification proposed by Droller et al.13 (gross hematuria, with clots and renal failure secondary to obstruction), and the initial treatment consisted of supportive measures (hyperhydration, forced diuresis, erythrocyte and platelets transfusions, ciprofloxacin, and pain management). These measures are necessary and could be sufficient in mild cases, but none has shown to be effective in grade II-IV hematuria.7,14
Based on the rationale that rhEGF is a cytoprotective agent that can enhance healing of acute and chronic wounds, bladder irrigation by cystoclysis and intravesical instillation of heberprot P (supplied by Heber-Biotec SA) were also used, but hematuria did not improve. Dorticos et al. reported a case of successful application of rhEGF in a patient with grade IV hemorrhagic cystitis after hematopoietic transplant.15
Cidofovir is a proven antiviral with responses between 60 and 80% as reported by various authors.16,17 In this patient, the medicine was not used due to unavailability.
The use of hyperbaric oxygen was decided and the resolution of the condition was achieved after 7 treatment sessions. This result is in line with recent studies reporting excellent responses to this therapy. Urbaniak et al. obtained a complete response in 5 patients with an average of 13 sessions18, other authors have published similar results in small series and case reports.19.20
Condyloma acuminatum of the anus is associated with HPV types 6 and 11 viruses and immunosuppressed states such as that caused by HIV infection; and in post-transplantation of solid organs and hematopoietic progenitors. The possible routes of infection are through sexual transmission, mainly in homosexual men or through contact with infected material, chronic irritation from perianal fistula, ulcerative colitis or poor personal hygiene. The incubation period is two to three months, although it can be up to 20 months.21
Although the histology is benign, the giant condyloma of the anus has oncogenic potential and a tendency to invade more deeply and displace the surrounding tissue, which is why it is considered an intermediate lesion between simple condyloma and squamous cell carcinoma.
In this case, the first symptoms appeared two months after the transplant, with lesions that started as a keratotic plaque and expanded to form a cauliflower-shaped mass that obliterated the entrance to the anal canal, causing local pain, suppuration, itching, bleeding and difficulty walking and defecating, as described in the literature.21
In our opinion, HPV acquisition and condyloma were associated with post-transplant immunosuppression. The patient emphatically denied sexual transmission as a route of HPV infection.
Treatment depends on the extension and size of the lesion; and several modalities are described; however, surgery is the selected choice with high favorable response rates and little risk of recurrence. Other therapies include the use of podophyllin, cryotherapy alone or in combination with 5-fluoracil, radiation therapy, combined chemotherapy, laser therapy, and the use of interferon, among others. 22
The patient underwent a conservative surgery and was allowed to close by second intention, thus guaranteeing better quality of life. Latorre et al.23) reported similar proceeding with successful result. Fanget et al. reported 10 cases of men treated for anus condyloma with a first local excision and the procedure was successful in six cases after a median follow-up of 94.5 months, concluding that an extensive resection was associated with long term survival without recurrence.24
After a follow-up of six months the presented patient was totally asymptomatic and with no signs of recurrence.
This work presents a case that has never been reported before in the literature where HC and giant condyloma acuminatum of the anus concur by reactivation of BK virus and human papilloma virus, respectively, in a haploidentical allogeneic TPH receptor. The use of hyperbaric oxygen in HC and surgical excision of the condylomatous tumor allowed the complete resolution of both pathologies and the preservation of the patient's renal and anal functions.