Sensibilidade dolorosa à palpação em pacientes com disfunção temporomandibular crônica
Painful sensitivity to palpation in patients presenting with chronic temporomandibular dysfunction
Sensibilidad dolorosa a la palpación en pacientes con disfunción temporomandibular crónica
]]>
Ana Lúcia Franco,I Caroline Borges de Oliveira,II Giovana Fernandes,I Sabrina Maria Castanharo,I Daniela A. de Godói Gonçalves,III Cinara Maria CamparisIV
I Licenciada em Odontologia. Faculdade de Odontologia. Universidade Estadual Paulista, Araraquara, Brasil.
II Doutor em Odontologia. Faculdade de Odontologia. Universidade Estadual Paulista, Araraquara, Brasil.
III Licenciada em Odontologia. Assistente. Faculdade de Odontologia. Universidade Estadual Paulista, Araraquara, Brasil.
IV Licenciada em Odontologia. Professora Adjunta. Faculdade de Odontologia. Universidade Estadual Paulista, Araraquara, Brasil.
]]>
RESUMO
Cefaléias primárias estão freqüentemente relacionadas à disfunção temporomandibular, sendo o aumento da sensibilidade dolorosa um achado comum nesses pacientes. Este estudo propôs investigar a sensibilidade dolorosa à palpação em pacientes com disfunção temporomandibular crônica, comparando grupos com presença ou ausência de cefaléias primárias. A disfunção temporomandibular e o tipo de cefaléia primária foram diagnosticados, respectivamente por meio dos critérios de diagnóstico para pesquisa das desordens temporomandibulares e por um questionário baseado na Classificação Internacional de Cefaléias (2004). A localização, avaliação e o agrupamento dos sítios musculares e articulares para palpação foram realizados segundo os critérios de diagnóstico para pesquisa das desordens temporomandibulares, considerando-se o temporal, masseter, articulação temporomandibular e sítios cervicais bilateralmente. A amostra foi composta por 213 (88,0 %) mulheres e 29 (12,0 %) homens, com faixa etária média de 37,41 anos. As médias do número de sítios positivos à palpação nos grupos sem cefaléia, cefaléia do tipo tensional, migrânea e cefaléia crônica diária e foram respectivamente: 12,43; 14,38; 15,21 e 15,62 (p= 0,107) (mínima 2 e máxima 22). Apenas para os sítios do músculo temporal foi detectada diferença estatisticamente significante entre os grupos de cefaléia quanto à sensibilidade dolorosa à palpação (p= 0,007). O número de sítios dolorosos não foi estatisticamente diferente entre os grupos estudados e apenas o músculo temporal demonstrou diferença estatisticamente significante quanto ao grau de dor à palpação.
Palavras chave: dor facial, articulação temporomandibular, cefaleia.
ABSTRACT
The cephalalgias are frequently associated with the temporomandibular disorders being common to find an increase of pain sensitivity in these patients. Thus, the objective of present study was to assess the sensitivity to palpation in patients presenting with chronic temporomandibular disorders comparing two groups one with headache and other without it, respectively. The temporomandibular disorders and the primary cephalalgias were diagnosed according the Diagnostic Criteria for the Research of Temporomandibular Disorders and by a questionnaire based on the International Classification of the Cephalalgias (2004). Location, assessment and grouping of muscular and articular areas for palpation were carried out according to the Diagnostic Criteria for above mentioned disorders, considering bilaterally the masseter muscle, the temporalis muscle, the cervical region and the temporomandibular joint. Sample included 213 (88.0 %) of women and 29 (12.0 %) men with a mean age of 37.41 years. The mean of number of zones positive to palpation in the groups without headaches, tension headache, migraine and daily chronic headache were: 12.43, 14.38, 15.21 and 15.62 (p= 0.107) (min 2 max 22). The areas of temporalis muscle showed significant differences among groups (p= 0.007). The number of painful points was not statistically different among groups and only in the temporalis muscle there were differences with statistical significant to palpation.
]]>
Key words: facial pain, temporomandibular joint, headaches.
RESUMEN
Las cefaleas están frecuentemente relacionadas con los trastornos temporomandibulares, por esta razón es común encontrar un aumento de sensibilidad al dolor en los pacientes que padecen dicha enfermedad. El objetivo de este estudio fue evaluar la sensibilidad a la palpación en pacientes con trastornos temporomandibulares crónicos. Se realizó una comparación entre 2 grupos con cefalea y sin cefalea respectivamente. Los trastornos temporomandibulares y las cefaleas primarias, fueron diagnosticados mediante los criterios diagnósticos para la investigación de los trastornos temporomandibulares y por un cuestionario basado en la clasificación internacional de cefaleas en el año 2004. La localización, evaluación y agrupación de las áreas musculares y articulares para la palpación, se realizaron de acuerdo a los criterios diagnósticos para la investigación de los trastornos temporomandibulares, se tuvo en cuenta el músculo masetero, el temporal, la región cervical y la articulación temporomandibular bilateralmente. La muestra fue de 213 mujeres (88,0 %) y 29 hombres (12,0 %), con una media de edad de 37,41 años. La media del número de zonas positivas a la palpación en los grupos sin cefalea, dolor de cabeza de tipo tensional, migraña y cefalea crónica diaria fueron: 12,43; 14,38; 15,21; 15,62 y (p= 0,107) (mínimas 2 y máximas 22). Las áreas del músculo temporal demostraron diferencias significativas entre los grupos (p= 0,007). El número de puntos dolorosos no fue estadísticamente diferente entre los grupos y solo en el músculo temporal se observó diferencias estadísticamente significativas a la palpación.
Palabras clave: dolor facial, articulación temporomandibular, cefalea.
INTRODUÇÃO ]]>
Disfunção temporomandibular (DTM) é um termo coletivo que abrange os problemas clínicos que envolvem a musculatura da mastigação, a articulação temporomandibular (ATM) e as estruturas associadas. Os sinais e sintomas incluem: dor nas estruturas envolvidas, limitação ou desvio no movimento mandibular e sons articulares durante a função.1 As DTM podem estar associadas a outras patologias somáticas ou neurológicas, como por exemplo às cefaléias primárias.2-5Estudos epidemiológicos em adultos sugerem uma associação entre cefaléia e DTM e que ambas apresentam sinais e sintomas similares.6-12 A gravidade da DTM parece estar correlacionada com a intensidade e a frequência com que a dor de cabeça ocorre, e o tratamento da DTM pode proporcionar um resultado positivo na redução da cefaleia.13,14 Além disso, cefaleias recorrentes são encontradas em 70 % a 85 % dos pacientes com DTM.15,16 Um estudo populacional de DTM e cefaléia, verificou-se que os indivíduos com sintomas de DTM têm 1,8 a 2 vezes mais chances de apresentar cefaléia.6
Segundo a literatura o dolorimento da musculatura pericraniana é um achado clínico comum nos pacientes portadores de DTM, cefaléia do tipo tensional (CTT) e migrânea.4,17,18 Sugere-se que os prolongados impulsos nociceptivos provenientes dos músculos da região da cabeça seriam responsáveis pela elevação da sensibilidade dolorosa e pela diminuição do limiar de dor local. Ainda estes impulsos levariam à sensibilização central nos pacientes afetados, posteriorente contribuindo para cronificação da dor e da cefaleia.19
Os dados levantados na literatura atual suportam a ideia de uma estreita inter-relação entre cefaleias primárias, DTM e sensibilidade pericraniana. Autores sugerem a existência de um mecanismo fisiopatológico comum, envolvido com o núcleo caudado do trigêmeo. Esse nervo, responsável pela sensibilidade orofacial, entrelaçaria os sinais e sintomas dessas condições. Sugere-se ainda, que um problema afetaria o outro, atuando como fator predisponente, desencadeante ou agravante.17-24 Assim o objetivo desse estudo foi investigar a sensibilidade dolorosa à palpação em pacientes com DTM crônica, comparando grupos com presença ou ausência de cefaleias primárias.
MÉTODO
Seleção da Amostra
A amostra foi composta por 242 pacientes que procuraram tratamento na clínica de Dor Orofacial e Disfunção Temporomandibular da Faculdade de Odontologia de Araraquara-Universidade Estadual Paulista (UNESP), Brasil, examinados durante os anos 2007 e 2008. Ao serem selecionados para a amostra todos os indivíduos assinaram o termo de consentimento livre esclarecido. Esse estudo foi aprovado pelo Comitê de Ética em Pesquisa em Seres Humanos da Faculdade de Odontologia de Araraquara (processo 33/06).
]]>
Avaliações
Todos os pacientes foram avaliados por um pesquisador calibrado de acordo com os seguintes instrumentos:
Ficha para anamnese e exame físico da Clínica de DTM e Dor Orofacial da FOAr-UNESP, no intuito de obter: a queixa principal, o diagnóstico de DTM e as características da dor (local, intensidade, qualidade, duração e fatores agravantes), presença de cefaleia e dores extra-cefálicas e a história médica. O critério diagnóstico da AAOP1 foi aplicado para o diagnóstico diferencial de outras condições capazes de mimetizar a DTM. Naqueles cuja presença de DTM foi confirmada, aplicamos o critérios de diagnóstico para pesquisas das desordens temporomandibulares (RDCDTM).
Critérios de diagnóstico para pesquisas das desordens temporomandibulares: traduzido, adaptado e validado na língua portuguesa,25,26 para confirmação do diagnóstico de DTM dolorosa e avaliação dos sítios dolorosos musculares e articulares.
Questionário para identificação da cefaleia primária baseado na Classificação Internacional das Cefaleias:27 que consiste em 26 questões que avaliam as principais características requeridas para o diagnóstico das cefaleias primárias mais comuns. As questões englobam as características da dor (ex. Latejante, em pressão), severidade (leve, moderada ou severa), localização (unilateral, bilateral), frequencia e duração das crises, sintomas associados e fatores desencadeantes. Com base nesse questionário todos os diagnósticos de cefaléias primárias puderam ser verificados: migrânea, cefaleia do tipo tensional, cefaleias em salvas e outras cefaleias trigêmino-autonômicas e outras cefaleias primárias. Adicionalmente segundo o critério proposto por Silberstein e Lipton,28 a cefaleia foi classificada como cefaléia crônica diária (CCD), caso houvesse relato de presença de dor por mais de 15 dias ao mês.
]]> Critérios de inclusão e de exclusão
Foram incluídos pacientes diagnosticados com DTM crônica dolorosa (dor por periodo maior que seis meses),29 de acordo com os critérios do Eixo I do RDCDTM. Os critérios de exclusão consistiram em: dor aguda, diagnósticos isolados do grupo II do Eixo I (deslocamentos do disco), osteoartrose com outra manifestação de DTM, odontalgia, neuropatia, lesões intra-orais, presença de outra condição dolorosa crônica, por ex. fibromialgia ou artrite, pacientes com alterações das funções cognitivas eu comprometimento da capacidade de comunicação e indivíduos menores de 18 anos.
Análise dos dados
A partir do questionário de cefaléia, considerando a presença e o tipo de cefaleia primária diagnosticada, os pacientes puderam ser alocados em quatro grupos: pacientes com DTM e sem cefaleia primária, pacientes com DTM e migrânea, pacientes com DTM e CTT e pacientes com DTM e CCD (presença de dor em mais de 15 dias ao mês). Segundo o formulário de exame muscular fornecido pelo Eixo I do RDCDTM:
O número de sítios dolorosos à palpação foi obtido pelo exame físico do RDCTMD, considerando-se bilateralmente 6 sítios para os músculos temporais, 6 para os masséteres e 4 para as ATM. Foram também considerados os músculos cervicais posteriores, esternocleidomastoideos e trapézios (6 sítios). Ao todo, foram examinados 22 sítios. O número de sítios com palpação diferente de zero foi contado e a média de sítios positivos à palpação obtida para cada grupo considerado. Para a análise quantitativa utilizou-se o teste de Mann-Whitney (distribuição não normal).
Para a análise da intensidade da dor à palpação, considerou-se a moda da graduação obtida durante a palpação de cada músculo e ATM, de acordo com a escala proposta pelo RDCDTM: 0 "ausência de dor", 1 "dor leve", 2 "dor moderada" e 3 "dor grave"; quando houve modas coincidentes, foi considerada aquela de maior valor. Os indivíduos foram agrupados de acordo com a moda da intensidade de dor demonstrada em cada sítio palpado além do diagnóstico de cefaléia primária atribuído. Foram utilizados testes do qui-quadrado para avaliar associações entre as intensidades dolorosas demonstradas pelos grupos, sendo considerados estatisticamente significantes aqueles que apresentaram nível de significância igual ou menor que 0,05.
]]>
RESULTADOS
A amostra foi composta por 213 (88,0 %) mulheres e 29 (12,0 %) homens, com faixa etária média de 37,41 anos, não havendo diferença estatisticamente significante entre os grupos para a idade (p= 0,652). Quanto ao gênero, as mulheres foram mais prevalentes em todos os grupos (p= 0,000), entretanto a diferença entre a proporção de mulheres e homens foi menor no grupo com DTM e sem cefaleia primária (respectivamente 60,9 % contra 39,1 %) e no grupo com DTM e CTT (respectivamente 75,9 % contra 24,1 %). Segundo a frequência, a cefaleia primária mais encontrada na amostra foi a migrânea (n= 99; 40,9 %), seguida pelas CCD (n= 91; 37,6 %), CTT (n= 29; 12,0 %) e ausência de cefaleias primárias (n= 23; 9,5 %).
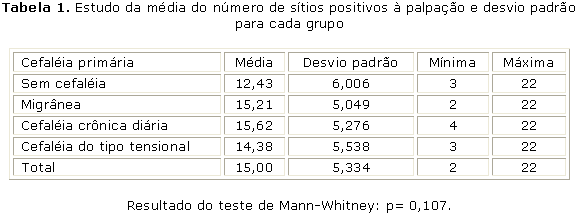
Conforme se pode observar na tabela 1, de um total de 22 sítios avaliados, a média do número de sítios positivos à palpação nos pacientes com DTM foi de 15,0 sítios (mín. 2 máx. 22), não havendo diferença estatisticamente significante entre os grupos de cefaleia primária (p= 0,107). A média do número de sítios positivos à palpação foi crescente na seguinte ordem: sem cefaleia (12,43 sítios), CTT (14,38 sítios), migrânea (15,21 sítios) e CCD (15,62 sítios).
Com relação à análise da intensidade da dor à palpação (tabelas 2, 3, 4 e 5) segundo os grupos de cefaleia primária, apenas no músculo temporal verificou-se diferença estatisticamente significante entre os indivíduos (p= 0,007). De acordo com a tabela 2, a maioria dos pacientes sem cefaleia primária apresentou como moda a intensidade 0, que representa ausência de dor nesse sítio muscular (n= 16; 69,6 %). De maneira similar e ao contrário do que se imagina os indivíduos diagnosticados com CTT também apresentaram em sua maioria, ausência de dor nesse sítio (n= 19; 65,5 %).
DISCUSSÃO
Trabalhos recentes5,16,30 mostram que determinadas cefaleias primárias são bastante comuns às populações com DTM, sendo portanto comorbidades esperadas, por dividirem uma fisiopatologia comum, envolvida com o aumento da atividade do sistema trigeminal.31 Esses pacientes apresentam sensibilidade muscular aumentada a qual parece mediada por alterações no processamento da dor.20 Os estímulos nociceptivos prolongados provenientes do tecido miofascial sensibilizam o sistema nervoso central e assim, induzem ao aumento da sensibilidade dolorosa.6,32
Também há possibilidade de que a mialgia apresentada por esses pacientes resulte da sensibilização dos nociceptores periféricos que inervam o tecido cutâneo e muscular.20 A hiperexcitabilidade neuronal resultaria de alterações capazes de afetar desde o nível dos receptores periféricos até os centros sensitivos mais altos do cérebro (córtex).21 Nesse estudo, apenas no músculo temporal foi detectada diferença estatisticamente significante entre os grupos quanto à sensibilidade, especialmente nos pacientes com migrânea e CCD. ]]>
Em pacientes com CTT e migrânea a sensibilidade dolorosa da musculatura pericraniana também é um achado clínico comum.4,17,18,33 Estudos demonstraram que a sensibilidade dolorosa aumentada dos pacientes com CTT é conseqüência e não fator de risco para a mesma, o que também suporta a hipótese da sensibilização central. Assim os impulsos nociceptivos provenientes da região da cabeça seriam responsáveis pela elevação da sensibilidade dolorosa e pela diminuição do limiar de dor local. Estes impulsos levariam à sensibilização central nos pacientes afetados, contribuindo para cronificação da cefaleia.19Migranosos apresentam sensibilidade dolorosa pericraniana aumentada durante os ataques de dor, o que sugere ser também conseqüência da cefaléia.18 Isso pode justificar a diferença encontrada na amostra apenas para a região do músculo temporal, cuja maior sensibilidade observada seria decorrente da sensibilização periférica das regiões onde a cefaleia é sentida. Diferentemente dos nossos achados em relação à cronicidade da cefaleia, estudos verificaram que a ocorrência de cefaleias freqüentes esteve correlacionada com o aumento da sensibilidade muscular e articular nos pacientes. Assim pode haver alteração qualitativa e quantitativa da nocicepção como conseqüência à sensibilização central, devido ao fluxo contínuo de impulsos proveniente dos tecidos pericranianos.7,18,19
Outro aspecto que influencia a manifestação e a intensidade dos sintomas dolorosos é o gênero. Esta amostra foi composta em sua maioria por mulheres e com faixa etária adulta média. Segundo a literatura as DTM são de 2 a 5 vezes mais prevalentes em mulheres do que em homens, acometendo os pacientes preferencialmente por volta da terceira a quinta décadas de vida.3,15 Além disso as cefaleias especialmente a migrânea, são também mais comuns nas mulheres entre os 20 e 50 anos.34 As evidências disponíveis suportam a existência de diferenças entre os gêneros no que diz respeito à resposta a dor. Verifica-se que a maioria das condições dolorosas crônicas (ex. fibromialgia, migrânea, artrite) é mais comum entre o gênero feminino.15,35 Dessa forma a elevada frequência de mulheres na amostra é, provavelmente, decorrente da maior procura por tratamento pelo gênero feminino, mais acometido por essas condições.
Devido à escassez de informações referentes às características comuns entre os pacientes com DTM e cefaleias primárias, este estudo apresenta relevância clínica. Nossos mais importantes achados consistem em: o número de sítios dolorosos não foi estatisticamente diferente entre os tipos de cefaleias primárias e dentre os sítios considerados, apenas o músculo temporal demonstrou diferença estatisticamente significante quanto ao grau de dor apresentado pelos pacientes.
Dessa forma, se conclui que a sensibilidade muscular pericraniana apresentada pelos pacientes com DTM pode ou não ser agravada pela presença de uma cefaleia primária. Pelo fato de as cefaleias primárias e as DTM serem condições inter-relacionadas, muitas vezes expressas concomitantemente por um mesmo indivíduo, saber dos achados comuns apresentados pelos pacientes é fundamental para um diagnóstico preciso e tratamento adequado.
REFERÊNCIAS BIBLIOGRÁFICAS
1. Okeson JP. Dor Orofacial guia de avaliação, diagnóstico e tratamento. São Paulo: Quintessence Editora Ltda; 1998. p. 287. ]]>
2. Auvenshine RC. Temporomandibular disorders: associated features. Dent Clin N Am. 2007;51:105-27.
3. Dworkin SF, Huggins KH, LeResche L, Korff MV, Howard J, Truelove E, et al. Epidemiology of signs and symptoms in temporomandibular disorders: clinical signs in cases and controls. J Am Dent Assoc. 1990;120:273-81.
4. Haley D, Schiffman E, Baker C, Belgrade M. The comparison of patients suffering from temporomandibular disorders and a general headache population. Headache. 1993;33:210-3.
5. Gonçalves DAG, Bigal ME, Jales LCF, Camparis CM, Speciali JG. Headache and symptoms of temporomandibular disorder: an epidemiological study. Headache. 2009;50(2):231-41.
6. Ciancaglini R, Radaelli G. The relationship between headache and symptoms of temporomandibular disorder in the general population. J Dent. 2001;29:93-8. ]]>
7. Bernhardt O, Gesch D, Schwahn C, Mack F, Meyer G, John U, et al. Risk factors headache, including TMD signs and symptoms, and their impact on quality of life. Results of the Study of Health in Pomernia (SHIP). Quintessence Int. 2005;36:55-64.
8. Mitriattanakul S, Merrill RL. Headache impact in patients with orofacial pain. J Am Dent Assoc. 2006;137:1267-74.
9. Glaros AG, Urban D, Locke J. Headache and temporomandibular disorders: evidence for diagnostic and behavioral overlap. Cephalalgia. 2007;27(6):542-9.
10. Ballegaard V, Thede-Schimidt-Hansen P, Svensson P, Jensen R. Are headaches and temporomandibular disorders related? A blinded study. Cephalalgia. 2008;28:832-41.
11. Liljeström MR, Le Bell Y, Laimi K, Antilla P, Aromaa M, Jämsa T, et al. Are signs and symptoms of temporomandibular disorders stable and predictable in adolescents with headache? Cephalalgia. 2008;28:619-25. ]]>
12. Lupoli TA, Lockey RF. Temporomandibular dysfunction: an often overlooked cause of chronic headaches. Ann Allergy Asthma Immunol. 2007;99:314-8.
13. Schiffman E, Haley D, Baker C, Lindgren B. Diagnostic criteria for screening headache patients for temporomandibular disorders. Headache. 1995;35:121-4.
14. Liljeström MR, Jämsa T, Le Bell Y, Alanen P, Antilla P, Metsähonkala L, et al. Signs and symptoms of temporomandibular disorders in children with different types of headache. Acta Odontol Scand. 2001;59:413-7.
15. Drangsholt M, LeResche L. Temporomandibular Disorder Pain. In: Crombie IK, Croft PR, Linton SJ, LeResche L, Von Korff M. Epidemiology of Pain. Seattle: IASP Press; 1999. p. 203-33.
16. Franco AL, Gonçalves DAG, Castanharo SM, Specialli JG, Bigal ME, Camparis CM. Migraine is the most prevalente headache in individuals with temporomandibular disorders. J Orofac Pain. 2010;24:287-92. ]]>
17. Graff-Radford SB. Temporomandibular disorders and headache. Dent Clin N Am. 2007;51:129-44.
18. Bendtsen L. Central sensitization in tension-type headachepossible pathophysiologycal mechanisms. Cephalalgia. 2000;20:486-508.
19. Buchgreitz L, Lyngberg AC, Bendtsen L, Jensen R. Frequency of headache is related to sensitization: a population study. Pain. 2006;123(1-2):19-27.
20. Maixner W, Fillingim R, Sigurdsson A, Kincaid S, Silva S. Sensitivity of patients with painful temporomandibular disorders to experimentally evoked pain: evidence for altered temporal summation of pain. Pain. 1998;76:71-81.
21. Jensen TS. Recent advances in pain research: implications for chronic headache. Cephalalgia. 2001;21:765-9. ]]>
22. Merrill RL. Central mechanisms of orofacial pain. Dent Clin N Am. 2007;51:45-59.
23. Woolf CJ. Central sensitization. Uncovering the relation between pain and plasticity. Anestesiology. 2007;106:184-7.
24. Buchgreitz L, Lyngberg AC, Bendtsen L, Jensen R. Increased pain sensitivity is not a risk factor but a consequence of frequent headache: a population-based follow-up study. Pain. 2008;137(3):623-30.
25. Dworkin SF, LeResche L. Research diagnostic criteria for temporomandibular disorders: review, criteria, examinations and specifications, critique. J Craniomand Disord. 1992;6:301-55.
26. Pereira FJ, Favilla EE, Dworkin SF, Huggins KH. Research diagnostic criteria for temporomandibular disorders (RDC/TMD). [On line]. 2009. Disponible en: http://www.rdc-tmdinternational.org/LinkClick.aspx?fileticket=ieimc6uFywQ%3d&tabid=86&mid=395. ]]>
27. Subcomitê de Classificação Internacional das Cefaléias da Sociedade Internacional de Cefaléia. Classificação Internacional das Cefaléias. São Paulo: Alaúde Editorial Ltda; 2006.
28. Silberstein SD, Lipton RB. Chronic daily headache, including transformed migraine, chronic tension-type headache and medication overuse. In: Silberstein SD, Lipton RB, Dalessio DJ. Wolff's headacheand other head pain. New York: Oxford University Press; 2001. p. 247-82.
29. Merskey H, Bogduk N. Classification of chronic pain: descriptions of chronic pain syndromes and definitions of pain terms. Seattle: IASP; 1994.
30. Gonçalves DAG, Speciali JG, Jales LCF, Camparis CM, Bigal ME. Temporomandibular symptoms, migraine and chronic daily headaches in the population. Neurology. 2009;73:645-6.
31. Dando WE, Branch MA, Maye JP. Headache disability in orofacial pain patients. Headache. 2006;46:322-6. ]]>
32. Jensen R, Bendtsen L, Olesen J. Muscular factors are of importance in tension-type headache. Headache. 1998;38:10-7.
33. Stuginsky-Barbosa J, Macedo HR, Bigal ME, Speciali JG. Signs of temporomandibular disorders in migraine patients: a prospective, controlled study. Clin J Pain. 2010;26:418-21.
34. Stovner JL, Scher AI. Epidemiology of Headache. In: Olesen J, Goadsby PJ, Ramadan NM, Tfelt-Hansen P, Welch KMA. The Headaches. Philadelphia: Lippincott Williams & Wilkins; 2006. p. 393-8.
35. Cairns BE. The influence of gender and sex steroids on craniofacial nociception. Headache. 2007;47:319-24.
]]>
Recibido: 26 de agosto de 2011.
Dra. Ana Lúcia Franco. Faculdade de Odontologia. Universidade Estadual Paulista, Araraquara, Brasil. Correo electrónico: analu.franco@hotmail.com
]]>