Hospital Militar Central "Dr. Luis Díaz Soto"
My. Ángel Arpa Gámez,1 Cap. Corb. Odalys González Sotolongo,2 Dr. Juan A. Henry Favier,1 Dr. Mario Cervantes Marichal,1 Dr. Vladimir Feliciano Álvarez1 y Dra. Dulce María González1
Se presenta una paciente de 30 años de edad, mestiza, con historia de nefrectomía por "quistes renales" que acude a consulta por disnea y tos. Se detecta derrame pleural quiloso bilateral y durante su evolución sufre un neumotórax espontáneo. Se realizó tomografía computadorizada del alta resolución, y se observó la imagen característica de una linfangioleiomiomatosis pulmonar. Se hace una breve revisión de la entidad. Se concluye que el caso es típico de esta rara entidad y los quistes renales por los que se le realizó nefrectomía pueden haber correspondido a angiolipomas renales, característicos de la enfermedad.
DeCS: NEFRECTOMIA; ANGIOLIPOMA; DERRAME PLEURAL; NEUMOTORAX; TOMOGRAFIA; LINFANGIOMIOMA, LEIOMIOMATOSIS; NEOPLASMAS PULMONARES. ]]>
La linfangioleiomiomatosis es una enfermedad rara que afecta a mujeres jóvenes en edad fértil.1-4 Se caracteriza patológicamente por la proliferación de músculo liso intersticial pulmonar y formación de quistes.1,5-11 No se conoce su incidencia y prevalencia, pero probablemente represente menos del 1 % de los casos de enfermedades pulmonares difusas. Se presenta casi exclusivamente en mujeres premenopáusicas; se encuentra más del 70 % entre los 20 y 40 años de edad.1,5-7
Casi todas las pacientes se quejan de disnea al momento del diagnóstico.6,7,9-16 Otras quejas comunes incluyen tos y dolor torácico. El examen físico puede ser irrelevante o demostrar estertores al final de la espiración, hiperinflación, murmullo disminuido o ausente. Algunas complicaciones matizan su evolución, como neumotórax espontáneo,14-17 quilotórax,18 quiloperitoneo, quiluria, quilopericardio y angiomiolipomas renales que crecen como grandes masas quísticas.19 Se presenta una paciente con este diagnóstico que aparentemente debuta con un quilotórax bilateral.
Paciente MGP, del sexo femenino, mestiza, de 30 años de edad, con historia de salud hasta 1997 en que es estudiada por dolor abdominal y se le diagnostica quiste mesentérico y grandes quistes en riñón izquierdo, por esto último se le realiza nefrectomía al año siguiente. Varios meses previos a este ingreso comienza con tos frecuente, seca y disnea progresiva. Al examinarla se detecta disminución de las vibraciones vocales y del murmullo vesicular en ambas bases pulmonares, sin otro hallazgo de interés. Desde el punto de vista radiológico (rayos X de tórax posteroanterior) se detecta un derrame pleural bilateral que es confirmado mediante ultrasonido. Se realiza toracentesis, obteniéndose un líquido de carácter lechoso. A los 7 días de evolución en sala se queja de dolor inframamario izquierdo, punzante que se exacerbaba con la respiración y empeoró la disnea. Se detecta radiológicamente un hidroneumotórax izquierdo del 5 % que es tratado con pleurotomía mínima y evoluciona favorablemente con reexpansión total. Se realiza los exámenes complementarios siguientes:
| Hb: 121 g/L | Glicemia: 4,05 mmol/L |
| Hto: 0,40 | Colesterol: 4,87 mmol/L |
| Leucocitos: 9,2 x 10 9/L | Triglicéridos: 0,86 mmol/L |
| Eritrosedimentación: 20 mm | Proteínas totales: 80,7 % |
| Serología: negativa | Albúmina: 44,2 |
| VIH: negativo | Amilasa: 75 U/L |
| Serología TB: negativa | LDH: 467 U/L |
| Tuberculina: 0 mm | Creatinina: 80 µmol/L |
| Células LE: negativo | |
| Estudio del líquido pleural: | |
| Leucocitos: 0 x 109/L | Amilasa: 360 U/L |
| Hematíes: 0 x 109/L | Factor reumatoideo: negativo |
| LDH: 280 U/L | Glucosa: 1,40 U/L |
| Colesterol: 3,20 mmol/L | Proteínas: 120 g/L |
| Triglicéridos: 39,0 mmol/lL |
US: Ausencia de riñón izquierdo. Resto normal. Derrame pleural bilateral.
Rayos X de tórax: derrame pleural bilateral.
Prueba funcional respiratoria: trastorno ventilatorio mixto con componente restrictivo moderado. Signos que traducen disminución importante en el comportamiento elástico pulmonar.
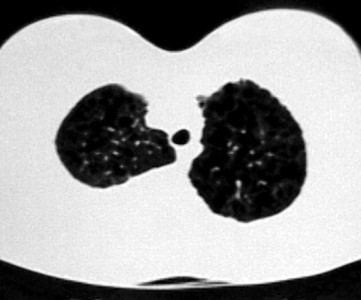
]]> Tomografía axial computadorizada de alta resolución (helicoidal): múltiples imágenes aéreas redondeadas, de paredes muy finas, que fluctúan de 0,5 a 3 cm y ocupan ambos pulmones de los vértices a las bases (fig.).FIG. TAC pulmonar. Imágenes en panal de abejas.
En esta paciente, la forma aparente de presentación pudiera considerarse el quilotórax bilateral descrito. Sin embargo, si se tienen en cuenta los antecedentes, en los que se recoge una nefrectomía izquierda por "grandes quistes renales" y una tumoración intraabdominal que fue definida como un "quiste mesentérico", claramente se puede reconocer estas alteraciones como manifestaciones típicas de la linfangioleiomiomatosis, según se describirán a continuación.
Esta rara entidad, según se dijo, casi exclusiva de las mujeres en edad fértil, se caracteriza, además de la sintomatología respiratoria (tos, disnea, signos de atrapamiento aéreo, hemoptisis, etc.), por diversas complicaciones tanto torácicas como extratorácicas. Dentro de las primeras el quilotórax y los neumotórax espontáneos son las más llamativas. El quilotórax se debe al engrosamiento y dilatación del conducto torácico y los linfáticos pulmonares por la proliferación anormal de células musculares lisas atípicas, pleomórficas, que se tiñen positivamente con el anticuerpo monoclonal HMB-45. Los neumotórax son consecuencia de la formación de dilataciones quísticas en los espacios aéreos distales,1,8,12 elemento característico de esta enfermedad y que se formarían por alguno de los mecanismos siguientes:
Aunque no se cuenta con la confirmación anatomopatológica, los grandes y múltiples quistes renales que se recogen en la historia clínica y llevaron a la nefrectomía en esta paciente pudieran corresponder a angiomiolipomas renales, que aparecen en el 50 % de dichos casos; en ocasiones alcanzan gran tamaño antes de ser detectados e imageneológicamente dan una imagen indistinguible de los quistes renales simples.19 Lesiones semejantes pueden verse en la cavidad abdominal o en el retroperitoneo.
Tanto los antecedentes que se recogen en esta paciente como los hallazgos actuales pueden corresponderse perfectamente con el diagnóstico de una linfangioleiomiomatosis, que en nuestro caso se confirmó con el hallazgo tomográfico de múltiples lesiones hipodensas, redondeadas, de paredes muy finas que abarcaban todo el parénquima de ambos pulmones. Como se ha dicho, el diagnóstico de esta entidad requiere biopsia pulmonar, pero las lesiones características descritas en la tomografía axial de alta resolución permiten confirmar el diagnóstico.
The case of a 30-year-old black female patient with hystory of nephrectomy due to kidney cysts that seeked for medical assistance due to dyspnea and cough., is presented. A pleural chylous bilateral effusion was detected and during the evolution she suffered from a spontaneous pneumothorax. High resolution computed tomography was performed and the characteristic image of a pulmonary lymphagioleiomyomatosis was observed. A brief review of the entity was made. It was concluded that the case was typical of this rare entity and that the kidney cysts for which she underwent nephrectomy may have correponded to kidney angiolipomas, which are characteristic of this disease.
Subject headings: NEFRECTOMY; ANGIOLIPOMA; PLEURAL EFFUSION; PNEUMOTHORAX; TOMOGRAPHY; LYMPHANGIOMYOMA; LEIOMYOMATOSIS; LUNG NEOPLASMS.
Recibido: 2 de junio de 2003. Aprobado: 8 de julio de 2003.
My. Ángel Arpa Gámez. Hospital Militar Central "Dr. Luis Díaz Soto". Avenida Monumental, Habana del Este, CP 11700, Ciudad de La Habana, Cuba. ]]>
1 Especialista de I Grado en Medicina Interna.
2 Especialista de I Grado en Endocrinología.
]]>