
Medical Care Organization to Face Dengue Epidemics
Organización de la atención médica para enfrentar una epidemia de dengue
]]>
Eric MartinezII MD, ScD. Professor and Researcher. Institute of Tropical Medicine "Pedro Kourí". Ciudad de La Habana, Cuba.
INTRODUCTION: dengue is only a disease with a wide clinical spectrum including undifferentiated fever or fever with malaise and general manifestations, and severe dengue, induced mainly by plasma extravasation leading to prolonged or recurrent shock and death. Medical care organization during epidemics is crucial to prevent fatalities and includes at least five components: 1. Training of medical and nurse personnel. It is an investment that shall be programmed, controlled and evaluated. The time and resources for training must be considered as the equivalent of the expenses in still unavailable vaccines or drugs against dengue. 2. Health education. To involve patients and their families in their own care, so that they can be prepared to ask for medical care at the right time, avoid self medication, identify skin bleedings (petechiae), and look for warning signs. 3. Classification of every suspected dengue case (triage). A good classification of patients should be simple to be used in every place and should be dynamic to allow changes in treatment. Early recognition of warning signs that announce dengue severity and intravenous fluids (crystalloids) given at that very moment can prevent dengue shock and other complications. 4. Rearrangement of medical services and warranty of some resources. It is not correct to think that the preparation to face a dengue epidemic will include big amounts of drugs, blood and blood products. The most important resource continues being the human resource. If doctors and nurses are well trained, the prescription of such drugs and procedures will decrease, including platelet transfusion or blood transfusions. 5. Research. Biomedical and social research are needed, with emphasis on the impact of health education on patients and their families, the natural course of the illness and the best way to do ambulatory treatment.
CONCLUSIONS: The future of the severe dengue cases will be usually decided upon not in the Intensive Care Unit but long before, in the Primary Care unit, Hospital Emergency Department or hospital ward. Good health managers can save more lives than physicians or intensive care specialists during dengue epidemics.
Key words: dengue shock, clinical warning signs, health education, capacity building, dengue case management, medical care organisation.
RESUMEN
INTRODUCCIÓN: el dengue es solo una enfermedad con un amplio espectro clínico que abarca fiebre común o fiebre con malestar y manifestaciones generales, mientras el dengue severo es provocado sobre todo por la extravasión del plasma que ocasiona un shock prolongado o recurrente y finalmente la muerte. La organización de los servicios de atención médica durante una epidemia es crucial para evitar decesos, abarca como mínimo cinco componentes: 1. Preparación del personal médico y de enfermería, constituye una inversión que se programa, se controla y se evalúa. El tiempo y los recursos que se emplean deben considerarse como el equivalente de los gastos en que pudiera incurrirse para adquirir vacunas o medicamentos contra esta enfermedad, que todavía no están disponibles. 2. Educación para la salud. Involucrar a los pacientes y sus familias en el cuidado de su salud, hacer que estén preparados para solicitar atención médica en el momento adecuado, evitar la automedicación, identificar los sangramientos por la piel (petequias), y buscar señales de aviso. 3. Clasificación de cada caso con sospecha de dengue (selección). Una buena clasificación de pacientes debe ser sencilla en todos los lugares y dinámica para permitir modificaciones en el tratamiento. El reconocimiento precoz de las señales de aviso que anuncian la gravedad del dengue y los fluidos intravenosos (cristaloides) administrados en ese preciso momento pueden evitar el shock y otras complicaciones. 4. Reordenamiento de los servicios médicos y aseguramiento de algunos recursos. No es correcto pensar que la preparación para enfrentar la epidemia de dengue incluirá grandes cantidades de medicamentos, volúmenes de sangre y de productos sanguíneos. El recurso más importante continúa siendo el recurso humano. Si los médicos y las enfermeras están bien adiestrados, las prescripciones para el uso de esos medicamentos y la aplicación de métodos disminuirán, incluida la transfusión de plaquetas o las transfusiones de sangre. 5. Realizar estudios investigativos. Son necesarios los estudios investigativos biomédicos y sociales, con énfasis en el efecto de la educación para la salud sobre los pacientes y sus familiares, el desarrollo natural de la enfermedad y la mejor forma de aplicar el tratamiento ambulatorio.
CONCLUSIONES: el futuro de los casos graves de dengue se deciden por lo general no en la Unidad de Cuidados Intensivos sino mucho antes, en la Unidad de Atención Primaria, el Departamento de Urgencias Médicas o la sala del hospital. Los buenos directivos del sistema de salud pueden salvar más vidas que los médicos o los especialistas de cuidados intensivos durante la epidemia de dengue.
]]>
Palabras clave: shock del dengue, señales clínicas de aviso, educación para la salud, fomento de capacidades, atención de los casos de dengue, organización de la atención médica.
]]>
INTRODUCTION
Dengue is only a disease with a wide clinical spectrum including undifferentiated fever, fever with malaise and general manifestations, with associated minor bleedings or not, which can increase in severity induced by plasma extravasation, thrombocytopenia, shock, massive digestive haemorrhages, and death, sometimes also having particular organ affectation as hepatitis, myocarditis, encephalitis or other.1
Although an antiviral drug is not available, it is not correct to say that dengue and severe dengue do not have any treatment. Dengue can be successfully managed with the application of the existing clinical knowledge to classify (triage) patients according to symptoms and the phase of the disease and the early recognition of warning signs that announce dengue severity.2 Dengue shock can be prevented with intravenous fluids (crystalloids) given at that very moment or successfully treated to prevent other complications as massive haemorrhages, disseminated intravascular coagulation and multi organ failure.3
The aim of this article is to contribute to prepare medical services in order to prevent fatalities during dengue epidemics by means of organizational and teaching activities demonstrating how important Medical Care managers in saving lives and preventing dengue complications are.
HOW TO IMPROVE MEDICAL CARE DURING DENGUE EPIDEMICS?
]]>
A particular dengue case can be well managed only if a group of organizational and teaching activities are carried out at every hospital, primary health centre and the community, as follows:
1. Training all medical and nurse personnel.
2. Health education to population.
3. Triage of dengue patients according to their signs and symptoms.
4. Reordering medical services and resources.
5. Doing research.
1. TRAINING OF MEDICAL AND NURSE PERSONNEL ]]>
Training personnel is an investment that shall be programmed, controlled and evaluated.4 The time and resources dedicated to training must be considered as the equivalent of the expenses in still unavailable vaccines or drugs against dengue.
To train all medical and nurse personnel working in hospitals or health centres to get knowledge and to develop capacities5 for:
1.1 Improve dengue diagnosis
During the training emphasis should be made on the following issues:
- Dengue diagnosis is supported by epidemiological, clinical and laboratory criteria. However, physicians usually must take decisions according to symptoms and signs of the disease because they cannot wait for dengue serology or other dengue laboratory confirmation to start treatment of a particular case. ]]>
- According to the clinical sequence, the disease has three stages or phases: febrile, critical and recovery.
- At the beginning and during the first days of the disease (Febrile stage) it is impossible to determine if the patient is going to have uncomplicated dengue all the time or if it is just the febrile stage of severe dengue. That is why every patient should be prospectively evaluated at least once a day during the febrile period and 48 hours after defervescence.
- Leucopoenia is more evident and intense in dengue fever than in severe dengue, particularly when haemorrhages are present. In this case, leukocytes counts can be normal or raised.
- Only the sequence of clinical manifestations and laboratory data can make the physician identify the patient WHO will develop severe dengue or the one that has already begun to develop it.
- The clinical warning signs are: intense and continuous abdominal pain, frequent vomiting, sudden fall of temperature from high fever to hypothermia, with weakness and, sometimes, lypothimia, irritability sometimes alternating with somnolence (table 1).

- The hematocrit and the platelet count are the most important laboratory tests to manage dengue cases.6 Usually, it is necessary to repeat both several times. .
- The hematocrit is normal at the beginning of the disease and increases progressively until it rose by 20% or more manifesting hemoconcentration due to clinically relevant plasma extravasation. At the same time, thorax radiography or abdominal ultrasonography shows ascitis and/or right or bilateral pleural effusion. Dengue shock is essentially hypovolemic.
- Other laboratory tests can be done, depending on the particular clinical picture of the patient and the facilities of the hospital or health centre: coagulation studies, speed of sedimentation rate, proteinogram, ionogram, liver enzymes, creatinine, urea and so on. ]]>
- Laboratory warning signs are the progressive increase of hematocrits and the progressive decrease in platelet counts.
1.2- Apply good classification of patients, which should be simple to be used in every place and also dynamic to allow changes in treatment
During the training, emphasis should be made on the following issues:
- Ambulatory management of patients during the first two or three febrile days, and also during the next days if bleedings or loss of fluids are not evident, and/or abdominal pain or another warning sign is not present.
- The patient and his/her family should be warned that he/she must come back immediately to the health facility if one of those signs appear.
- Dengue shock is 4 to 5 times more frequent during defervescence or during the 24 next hours than during the febrile stage.
- Intense and continuous abdominal pain or another warning sign indicates the beginning of clinical deterioration of dengue patient. This is the right time to start intravenous fluid (crystalloids) replacement to save his or her life.7 ]]>
- Bleedings are not necessarily related to the severity of thrombocytopenia.7
1.3- Improve treatment: to prevent and to early treat the complications avoiding unnecessary drugs.
During the training, emphasis should be made on the following issues:
- Intravenous (IV) fluid therapy should be started at the place where the warning sign has been identified. Even when the patient is going to be sent to another hospital, fluid replacement should not be delayed. The main objective : to prevent shock.
- Every admitted dengue patient must be clinicaly monitored (blood pressure, respiratory rate, cardiac rate, temperature particularly looking for coldness of distal segments, cyanosis or other sign of impaired hemodynamic situation- to detect the imminence of shock. IV rehydration is mandatory. Main objective: early treatment of shock.
- The first sign of shock is the narrowness of the blood differential pressure (less than 20 mm Hg). Later, hypotension and other clinical signs of shock such as tachycardia and tachypnea will be present.
- During dengue shock, haematemesis and other major hemorrhages are frequent, including respiratory hemorrhages, and others that can be massive ones. to prevent shock also means to prevent major hemorrhages ]]>
- At the very beginning of dengue shock, physicians will not be afraid of prescribing the necessary volume of IV fluid usually a relative big volume of fluid is needed- to rapidly restore the hemodynamic balance. The main objective: to prevent multi organ failure and disseminated intravascular coagulation.
- Crystalloids are the choice for the treatment of dengue shock. When to initiate fluid replacement to prevent dengue shock or to treat it early is the most important question a physician must raise, even more important than what kind of crystalloid solution should be used.
- 20 mL of IV fluids per Kg will be prescribed for the first hour, although sometimes the patient will not require all this because he or she will be hemodynamically recovered before that time. On the contrary, other patients will need the administration of this amount of IV fluids at least twice.
- The use of Colloids in dengue shock should be restricted to special situations when a rapid restoration of blood pressure is needed or crystalloids alone are unable to get it. Anyway, the volume of colloids won't be big and the treatment with IV crystalloids solutions should be resumed later.
- An important haemorrhage may be the causes of prolonged dengue shock after an adequate volume of IV fluids has been given, particularly if hematocrits are decreasing. It is the time to consider a blood transfusion (packed red cells).
- It has not been demonstrated the usefulness of platelet transfusions.
- Neither corticoids nor heparins are used in dengue shock.
- Inotropic drugs (dopamine, dobutamine) are indicated when the ventricular function is impaired or when the replaced IV fluid has failed to improve perfusion.
]]>
2. HEALTH EDUCATION
The population living in a city or region where dengue is being transmitted must be well informed, not only on the actions for vector control, but on the symptoms and signs of the illness.
Health education, what for?
To involve patients and their families in their own care, being prepared to ask for medical care at the right time, avoid self medication, identify skin bleedings (petechiae), consider the day of defervescence (and during 48 hours) as the time when complications more frequently occur and look for warning signs as intense and continuous abdominal pain, and frequent vomiting.
The best way that information can be understood and accepted by each group of population will depend on their own cultural level, the knowledge on dengue and other diseases they have previously achieved, the accessibility to health services, among others. That is why the design of educational activities should be done by health technicians working together with experts in social communication. ]]>
Mass media can have an excellent participation if they are duly guided. Workshops and other meetings with journalists, editors, artists and executives will contribute to draw the best strategy to educate people without making them feel panic. It is about to give information but also to assist in changing attitudes.Teachers and professors from different teaching levels become indispensables, even more if are able to multiply their efforts using their own students. Doing this, health education can be taken to homes and families by members of their own. The same can be done by formal and informal community leaders.
During dengue epidemics, the medicine and nurse students working together with community activists can visit homes with a double purpose: to do health education and to search for dengue cases. This activity has demonstrated to be feasible, unexpensive and effective, and must be coordinated with the Primary Health Care units, having printed some messages on dengue illness and warning signs to be delivered in the community.
Medical care providers as physicians and nurses must include health education actions into their daily activities considering that promotion and prevention are also an important part of the work they have to do.
3. CLASSIFY EVERY SUSPECTED DENGUE CASE (TRIAGE)
To classify dengue cases, how? ]]>
Up to now, symptomatic dengue virus infections have been classified into three categories: undifferentiated fever, dengue fever (DF) and Dengue Hemorrhagic Fever (DHF); DHF was further classified into four severity grades, grades III and IV being defined as Dengue Shock Syndrome (DSS). Over recent years there have been many reports from South and Latin America about the difficulties in the use of this classification8-10 which were summarized in a systematic literature review.11 Difficulties in applying the complex criteria for DHF in the clinical setting and the appreciation that many cases of clinically severe dengue cases did not fulfil the criteria of DHF lead to the request from practising clinicians around the world to re-visit the classification scheme originally developed over 30 years ago.
A Word Health Organization/Program for Training and Research in Tropical Diseases (WHO/TDR) supported prospective clinical multi-centre study (DENCO, DENgue CONtrol)), across dengue endemic regions was set up to collect evidence about criteria for classifying dengue that could be used to aid triage, clinical management, surveillance and future research. The DENCO study reports that by using clinical and simple laboratory tests it is possible to classify patients into two groups based on the severity of illness (Fig.) while taking into consideration the evolving nature of the disease, the two groups are: Severe dengue and dengue with or with warning signs.
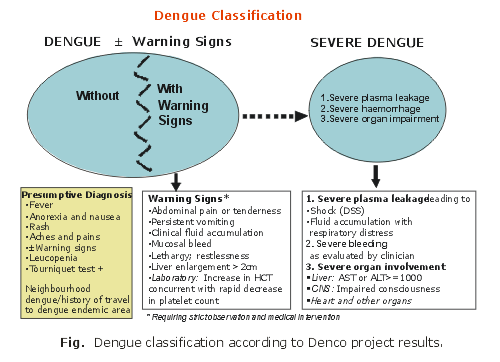
An expert consensus group had been convened in Geneva from 29 September to 01 October 2008 with the aim of advising on the use of the DENCO data. 50 dengue experts from 25 countries in the world convened for the meeting. The participants of the group have endorsed the results of the study. The need to change the existing WHO classification for dengue has been recognised and the DENCO model has been recommended by the expert group for worldwide application. The model should be tested in implementation research for further refinement and adaptation, if necessary, before implementation and recommendation by WHO for regional and national use. (TDR/WHO). Modification to the Dengue Case Classification: An expert consensus based on reviewing available literature and evidence from the DENCO study. Meeting held in Geneva: 29 September to 01 October 2008. Date of draft: 02 October 2008)
To classify dengue cases, what for? ]]>
Physicians and other medical care providers need a simple method to classify patients during an epidemic.12 Classify to act, that means identify specific signs in patients to decide the best way to be managed: where and how treat him or her, what laboratory tests are necessary, which prescriptions can be done and when to initiate early IV fluid therapy.
This triage or classification of patients for treatment is to be applied at every level of the Health System, including Primary Care units, emergency departments, wards in hospitals, and also during the home visits by medical service providers and trained students. Dengue cases should be actively searched and identified.
Every febrile patient should be interrogated according to clinical and epidemiological thinking to find out the day when the fever began, considered in practice as the first day of the disease. Those questions and a careful clinical examination are also important to make the diagnosis of other causes of fever (differential diagnosis) which frequently also occur during dengue epidemics.
Just a few questions are necessary to classify the febrile patient: does he or she have dengue? Is any bleeding present? Is any Comorbidity or any special condition age, pregnancy- present? Any warning sign? ¿shock? According to these questions, the suspected dengue case will be included in one of three groups (A, B or C) to take management decisions. Every case often needs a very dynamic evaluation because the ill person can change his/her clinical picture in a short time and new decisions for treatment are required.
Management decisions13
Depending on the clinical manifestations and other circumstances, patients may be:
]]>
· sent home (group A),
Group A patients who may be sent home
These are patients who are able to tolerate adequate volumes of oral fluids and pass urine about 3-4 times per day; they do not have any of the warning signs, particularly when fever subsides. Ambulatory patients should be checked daily for warning signs until they are out of the critical period. If full blood counts are done, those with stable hematocrits can be sent home with the advice to return immediately to the hospital if they develop any of the warning signs. Every patient considered as dengue (GROUP A) having neither bleeding nor warning signs- may have ambulatory treatment: acetaminophen for fever and body pain and plenty of fluid orally during the febrile period but particularly during defervescence, when the same oral rehydration salts used for diarrhoea can be taken.
Group B patients who should be referred for in-hospital management
]]>
These include patients with any of the following feature:
Patients with warning signs:
Warning signs suggest on-going, significant and sudden decrease in intravascular volume. Warning signs help doctors at the frontline and primary care levels to identify patients at higher risk of developing severe disease for referral to a higher level of care.
A patient with clinical warning signs will need IV fluid therapy. . This is the right time to start IV fluid resuscitation and save the patient's life. The physician must consider that the critical stage of dengue has begun and therefore, the patient can undergo shock and other complications. The progressive increase of hematocrits and/or progressive decrease of platelets are laboratory warning signs, not being necessary to wait for frank hemoconcentration (hematocrits > 20 %) to give IV fluids.
Give only isotonic solutions such as 0.9% saline, Ringer's lactate, Hartmann's solution. Start with 5-7 ml/kg/hour for 1-2 hours, and then reduce to 2-3 ml/kg/hr or less according to clinical response. Obtain if possible- a reference haematocrit before fluid therapy. Give the minimum volume required to maintain good perfusion and urine output of about 0.5 mL/kg/h. Intravenous fluids are usually needed for only 24 to 48 hours. Patients with warning signs should be re-classified as severe dengue if they meet the criteria of severe dengue.
Patients without warning signs, but having:
]]>
Co-existing conditions that may make dengue or its management more complicated, such as pregnancy, infancy and old age, obesity, diabetes mellitus, renal failure, chronic haemolytic diseases, peptic ulcer and others. Social circumstances such as living alone or living far from health facility or without a reliable means of transport.Patients with spontaneous mucosal bleedings are also considered in GROUP B and they will need to have platelet count and hematocrits (probably will be repeated some hours later).
The main reason to decide hospital admission of these dengue patients is to keep them under medical surveillance to observe and note his / her serial vital signs (blood pressure, respiratory rate, cardiac rate, temperature, volume of fluid intake and losses, urine output volume and frequency) and abdominal pain or other warning sign. During defervescence, this clinical surveillance is crucial and the mentioned signs should be watched hourly, if possible.
Encourage oral fluids. If not tolerated, start intravenous fluid therapy of 0.9% saline or Ringer Lactate with or without dextrose at maintenance rate. Patients may be able to take oral fluids after a few hours of intravenous fluid therapy.
Group C: Patients with Severe Dengue who require emergency treatment and urgent referral
If shock is evident, with narrowness of blood differential pressure < 20 mm Hg or frank hypotension, patient is considered in GROUP C and receive urgent treatment for hypovolemic shock also very similar to the treatment of hypovolemic shock during severe diarrhoea mainly IV fluid replacement (crystalloids).
]]>
4. REARRANGEMENT OF MEDICAL SERVICES AND GUARANTEE SOME RESOURCES
- Rearrange the Emergency Department, giving priority to patients with dengue (14), having trained personnel to classify febrile cases, at hospitals and Primary Care level, where dengue units must be created with physicians and nurses working 24 hours a day.
- Apply triage for the classification of patients. Posters with the fluxogram can be located where patients are being classified.
- Perform just the essential laboratory tests.
- Apply well defined admission criteria (table 1) having hospital beds enough for every dengue case that could need it.
- Create new facilities in Primary Care level units to give immediate and transitory medical care to patients with dengue WHO need intravenous fluid therapy (until they can be transferred to the hospital). ]]>
- Organise a good clinical observation for admitted patients. Trained medical and nursery students can cooperate in looking for warning signs and watching vital signs every one or two hours in order to early identify complications.
- Transform an ordinary hospital ward (or more than one, if necessary) in dengue ward(s) for clinical observation and treatment of patients with a minimum of trained nurses and doctors.
- Give qualified medical attention to severe dengue cases in wards for special care where the best human and other resources have been located and controlled, keeping Intensive Care Units for every severe case that need supported ventilation or other particular procedure.
- Discharge patients according to unified criteria (table 2).
- A high scientific level Committee will evaluate and control the process, analyse the cases that die and provide the media with relevant information on a regular basis.
- Some drugs should be guaranteed, such as acetaminophen, crystalloids solutions for intravenous infusions, a minimum of colloids (human plasma or human albumin, gelatine or starch), some inotropic drugs, the reagents to be used in the laboratories and radiographic films. Recently, sonographic studies have demonstrated their usefulness and have replaced more expensive studies. Neither corticoids nor heparin will be used.
- Equipments for microhematocrits are very useful and should be located in the facilities.

It is not correct to think that the preparation to face a dengue epidemic will include big amounts of drugs, blood and blood products. If doctors and nurses are well trained, the prescriptions of such drugs and procedures will decrease, including platelet transfusion or blood transfusions, although some platelets and blood should be available. The most important resource continues being the human resource.
A relative small number of resources well used and on time are able to save lives with a low cost, and on the contrary- all the expensive treatments used late in the process of clinical impairment won't be able to save dengue cases already with severe complications. ]]>
5. TO DO RESEARCH
- Introduce and evaluate the results from former investigations (implementation research) and do new biomedical and social research, with emphasis on the impact of health education on patients and their families, the natural course of the illness and the best way to do ambulatory treatment.
CONCLUSIONS ]]>
The future of the severe dengue cases will be usually decided not in the Intensive Care Unit but long before, in the Primary Care unit, Hospital Emergency Department or hospital ward. By improving organization and training of the personnel, good health managers can save more lives than physicians or intensive care specialists during dengue epidemics.
ACKNOWLEDGEMENT
To Olaf Horstick who kindly revised the paper and made valuable comments and linguistic corrections.
]]>
REFERENCES
1. Martínez-Torres E, Polanco-Anaya AC, Pleites-Sandoval EB ¿Cómo y por qué mueren los niños con dengue? Rev Cubana Med Trop. 2008;60(1):40-7.
2. Rigau-Perez JG, Laufer MK. Dengue-related deaths in Puerto Rico, 1992-1996: diagnosis and clinical warning signals. CID. 2006;42:1241-6.
3. Martinez E. La prevención de la mortalidad por dengue: un espacio y un reto para la atención primaria de salud. Rev Panam Salud Pública. 2006;20(1):60-74.
4. Ettelt S, Nolte E, Thomson S, Mays N, and the International Healthcare Comparisons Network. Capacity planning in health care: a review of the international experience. New policy brief on capacity planning. World Health Organization on behalf of the European Observatory on Health Systems and Policies. Policy Brief No. 13, February 2008. Available at: http://www.euro.WHO.int/Document/E91193.pdf
5. Kalayanarooj S, Chansiriwongs V, Vatcharasaevee V, Waleerattanapa R, Nimmannitya S. Capacity building for case management of dengue hemorrhagic fever. Thai Pediatr J. 2000;7:178-9.
6. De Azevedo MB, Kneipp MB, Baran M, Nicolai MC de A, Caldas DR, Fernandes SR et al. O previsível e o prevenível: mortes por dengue na epidemia carioca (em foco/informe epidemiológico em saúde coletiva). Rev Saúde (Rio de Janeiro) 2002;24:65-79.
7. Villar-Centeno LA, Díaz-Quijano FA, Martínez-Veja RA. Biochemical alterations as markers of dengue hemorrhagic fever. Am J Trop Med Hyg. 2008;78(3):370-4.
8. Deen JI, Harris E, Wills B, Balmaseda A, Hammond SN, Rocha C, et al. The WHO dengue classification and case definitions: time for reassessment.Lancet. 2006;368:170-3. Available at: www Thelancet.com
9. Thangaratham PS, Tyagi BK. Indian perspective on the need for new case definitions of severe dengue. Lancet. 2007;7:81-3. Available at: http://infection.thelancet.com
10. Rigau-Pérez JG. Severe dengue: the need for new definitions. Lancet. 2006;6:297-302. Available at: http://infection.thelancet.com
11. Bandyopadhyay S, Lum L, Kroeger A. Classifying dengue: a review of the difficulties in using the WHO case classification for dengue haemorrhagic fever. Trop Med International Health. 2006;11(8):1238-55.
]]>
12. Zamora-Ubieta F, Castro-Peraza O, González-Rubio D, Martínez-Torres E, Sosa-Acosta A. Guías prácticas para la asistencia integral al dengue. Ciudad de La Habana; 2006 [citado 2 Nov 2006]. Disponible en: http://www.sld.cu/galerias/pdf/sitios/ desastres/guia_dengue.pdf
13. Martínez-Torres E. Datos-clave para el tratamiento de enfermos con dengue. Em: Dengue. Estudos Avançados (São Paulo). 2008;22(64):33-52. Disponible en: http://www.scielo.br/scielo.php?script=sci_issuetoc&pid=0103-401420080003&ln
14. Wakimoto MD, de Azevedo MB, de Oliveira JSA, Vlommaro, Dornas JE. A experiencia de um hospital público na vigilancia e assistencia aos casos de dengue durante a epidemia de 2002 (em foco/informe epidemiológico em saúde coletiva). Rev Saúde (Rio de Janeiro). 2002;24:55-63.
Recibido: 2 de agosto de 2008.
Aprobado 30 de diciembre de 2008.
]]>
Dr. Eric Martinez. Institute of Tropical Medicine «Pedro Kourí» (IPK). Autopista Novia del Mediodía Km 6 1/2, Lisa, Ciudad de La Habana, Cuba. E-mail: ericm@ipk.sld.cu ]]>