ARTÍCULO ORIGINAL
Factores de riesgo y complicaciones cardiovasculares en pacientes con enfermedad renal crónica en hemodiálisis: prevalencia, morbilidad y mortalidad
Risk factors and cardiovascular complications in patients with chronic renal disease on hemodialysis: prevalence, morbidity and mortality
MSc. Mirna Caridad Atiés Sánchez,1 Dra. Silvia Collado Nieto,2 Dr. Julio Pascual Santos,2 Dr. Higinic Cao,2 Dr. Frances Barbosa2
1 Instituto Nacional de Nefrología "Abelardo Buch López".
RESUMEN
Objetivos: describir los factores de riesgo cardiovasculares (FRCV) y la asociación con enfermedad cardiovascular (ECV) de los pacientes con enfermedad renal crónica (ERC) en hemodiálisis (HD).
Métodos: se realizó un estudio descriptivo transversal. Se incluyeron 345 pacientes prevalentes adultos en programa de HD convencional, por cualquier etiología, de ambos sexos, con 18 y más años, que se encontraban en el Hospital del Mar de Barcelona y 3 centros de diálisis de los que dicho hospital es centro de referencia, y que mostraron su consentimiento informado por escrito, se revisaron historias clínicas de las bases de datos de dichos centros y se emplearon estadísticas descriptivas.
Resultados: la edad media fue de 69,19 ± 14,03 años; 71,5 % del sexo masculino; el tiempo promedio en tratamiento 62,26 ± 84,79 meses. La frecuencia de los FRCV clásicos ha sido hipertensión (82,5 %), diabetes mellitus (DM, con 32,2 %), sexo masculino (71,6 %) y dislipemia (55,7 %).
Conclusiones: los pacientes con enfermedad renal crónica en hemodiálisis tienen elevada frecuencia de ECV y de FRCV clásicos. Los factores predictores de ECV clínica en nuestra población fueron la edad, la presencia de ECV subclínica HVI y FRCV clásicos (HTA, DM, dislipidemia y hábito tabáquico, edad, Índice de comorbilidad de Charlson).
Palabras clave: enfermedad renal crónica, enfermedad cardiovascular, hemodiálisis, factor de riesgo cardiovascular.
Abstract
Objectives: describe cardiovascular risk factors (CVRF) and their association with cardiovascular disease (CVD) in patients with chronic renal disease (CRD) on hemodialysis (HD). Methods: a descriptive cross-sectional study was conducted with 345 prevalent adult patients of both sexes, aged 18 and over, following a conventional HD program irrespective of etiology at Mar de Barcelona Hospital and 3 other dialysis centers for which the said hospital is a reference center. All patients gave their informed consent in writing. A review was made of the medical records contained in databases at the said centers, and descriptive statistics were applied.
Results: mean age was 69.19±14.03; 71.5 % of patients were male; mean treatment time was 62.26 ± 84.79 months. The frequency of classical CVRFs was the following: hypertension (82.5 %), diabetes mellitus (DM, 32.2 %), male sex (71.6 %) and dyslipemia (55.7 %). CVD was present in 60.5% of patients; 53.9 % was of cardiac origin proper. The following risk factors were associated with cardiovascular disease: smoking, dyslipidemia, DM, arterial hypertension (AHT), LVH, age, and Charlson comorbidity index, with a statistical significance of (p< 0.05).
Conclusions: patients with chronic renal disease on hemodialysis have a high frequency of CVD and classical CVRFs. The factors predicting clinical CVD in our population were age, the presence of subclinical CVD, LVH, and classical CVRFs (AHT, DM, dyslipidemia, smoking, age and Charlson comorbidity index).
Key words: chronic renal disease, cardiovascular disease, hemodialysis, cardiovascular risk factor.
INTRODUCCIÓN
La elevada prevalencia de
La morbimortalidad en hemodiálisis (HD) no ha disminuido sensiblemente en los últimos años a pesar de los avances técnicos de la misma.2 Esto se debe en parte, al incremento progresivo de la edad y comorbilidad de los pacientes incidentes. La propia ERC empeora el pronóstico CV3 y por ello se incluye como factor de riesgo (FR) independiente en la actualización del JNC (JAMA) VII.4 Por otro lado, la presencia de patología CV acelera la progresión de
Según datos recientes explican que un porcentaje importante de muerte CV en los pacientes en HD no es de origen aterotrombótico, por lo que se ha postulado que la enfermedad microvascular y la disminución de la compliance arterial (mayor rigidez) al nivel de la aorta y grandes vasos de conductancia, podrían desempeñar un papel relevante.8,9 Se le sumará una serie de agresiones químicas, inmunológicas, biológicas y psicosociales producidas por los métodos dialíticos, por lo que a las variables de los factores de riesgo “tradicionales” o clásicos, definidos en la población general por el estudio de Framinghan,10 se le incluyen las anormalidades hemodinámicas y metabólicas, asociadas con
El objetivo de este estudio fue describir la frecuencia y distribución de los factores de riesgo CV a fin de evaluar el papel de dichos factores sobre los eventos CV y su relación con morbi-mortalidad en los pacientes portadores de ERC en hemodiálisis (HD) en nuestra área.
MÉTODOS
]]> Se realizó una investigación observacional, descriptiva, de corte transversal donde se incluyeron 345 pacientes prevalentes adultos (25 pacientes del Hospital del Mar, 115 pacientes de Diagonal, 135 pacientes del centro de Granollers y 75 pacientes de Julio Verne), de ambos sexos, en programa de HD convencional, durante al menos 3 meses, por cualquier etiología en el Hospital del Mar de Barcelona y dichos centros de diálisis extrahospitalarios de los que dicho hospital es centro de referencia de nivel I según el Plan de Ordenación de Nefrología deSe evaluaron las siguientes variables en la visita de inicio: datos demográficos y antropométricos del paciente (edad, sexo, peso, talla, índice de masa corporal, fecha de inicio de HD, si existían o no trasplantes previos y de existir, número de estos), así como la presencia de ECV de origen cardíaco, definida por la existencia de enfermedad coronaria de origen isquémico, enfermedad valvular, antecedentes de episodios de insuficiencia cardíaca o arritmia, presencia de ECV de origen no cardíaco: cerebral (accidente vascular cerebral o accidente isquémico transitorio) o periférica (vasculopatia periférica en las extremidades inferiores, amputación por isquemia, isquemia intestinal, etc.), presencia de diabetes, historia de HTA, dislipemia, tabaquismo y características de
Análisis estadísticos
A partir de las historias clínicas informatizadas de los diferentes centros de hemodiálisis se recogió toda la información y se plasmaron en el MRDP (modelo de recolección del dato primario) diseñado para la investigación creándose una base de datos utilizando el SPSS-PC (Stadistical Package for Personal Computer) versión 18.0 para Windows. El análisis descriptivo de los datos para variables cualitativas se realizó mediante números absolutos y porcentajes. Las variables cuantitativas se expresadaron a través de las medidas de tendencia central y dispersión (media ± DS, valores mínimos y máximos, intervalos de confianza al 95 %) y se compararon mediante la prueba de t de Student para muestras independientes en variables cuantitativas y en variables cualitativas, la prueba de Chi cuadrado, nivel de significación p< 0,05.
RESULTADOS
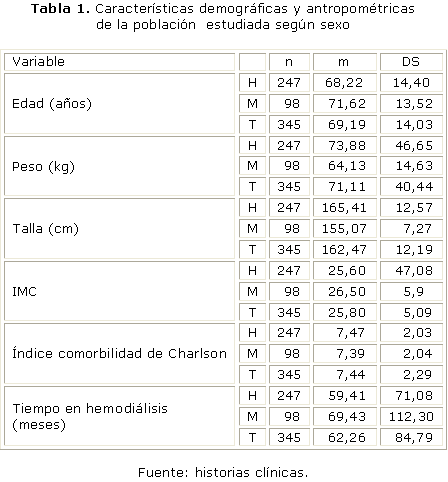
En la tabla 1 se muestra la distribución de nuestra población en cuanto a demografía y antropometría. Existió diferencia importante entre ambos sexos y esto nos condujo a establecer comparaciones de medias y porcentajes entre ellos. Nuestra muestra estuvo constituida por 345 pacientes (71,6 % varones y 28,4 % mujeres), con una media de edad de 69,19 ± 14,03 años y el tiempo medio en programa de HD de 62,26 ± 84,79 meses. El índice de comorbilidad de Charlson fue de 7,44 ± 2,29 puntos, el índice de masa corporal (IMC) reflejado fue de 25,8 ± 5,9 y solo el 10,7 % (37) de los pacientes tenían antecedentes de trasplante renal previo.
]]>
Se observa en la tabla 2 la frecuencia y porcentaje de los factores de riesgo cardiovascular en la población estudiada, donde se destaca
La tabla 3 refleja el comportamiento de dichos factores de riesgo cardiovascular clásicos con el sexo en esta muestra, donde se observa
La tabla 4 muestra la distribución de la enfermedad cardiovascular prevalente en los pacientes de esta serie (caso/frecuencia). Se encontró que la prevalencia de enfermedades cardiovasculares era del 60,5 %, con un 53,9 % de enfermedad cardíaca y dentro de ellas
En el análisis de los factores de riesgo o parámetros clínicos que se asociaron con ECV prevalente, tal y como se muestra en la tabla 5, se dividieron entre pacientes con y sin ECV. Se observa que la edad, el peso, el índice de comorbilidad y el tiempo en hemodiálisis, presentaron significación estadística (p< 0,05). Dentro de los factores de riesgo clásicos encontramos que el tabaquismo, HTA, DM, dislipidemia,
Muchos son los trabajos publicados sobre FRCV y enfermedades asociadas con esta. Tan vasta es la literatura sobre el tema, que al profundizar en su estudio, surge la duda, de qué aspectos son en los que habría que hacer énfasis al investigar.
En nuestro estudio, de una población de 345 pacientes, la demografía y antropometría es similar a los resultados de otros estudios realizados y así se sabe que la frecuencia de la población en métodos dialíticos aumenta con la edad. En el Reino Unido,16 en el año 2000, la media de la población en terapia de remplazo renal era de más de 55,1 años y en el año 2002 el 30 % era mayor de 65 años y 11 % era mayor de 75 años. En España, Pérez García17 en estudio en 2 618 enfermos observó que la edad media era de 66 ± 12 años, con un rango de
Cuando vemos los otros aspectos demográficos y antropométricos, nuestros resultados coinciden en su gran mayoría con estudios publicados,20,21 que son el reflejo de la población que entra en los programas de diálisis en la actualidad en España.
Charlson23 validó en 1987 el índice de comorbilidad asociado con edad (ICCE) para predecir la mortalidad al cabo de 10 años. Este índice se utilizó posteriormente en pacientes en hemodiálisis.24 En el estudio MAR (Morbidity and Mortality Anemia Renal Study)25,26 se calcula el ICCE y se obtiene un valor medio de 6,5 ± 2,3, que es algo inferior al encontrado en nuestro trabajo (7,44 ± 2,29). De los pacientes incluidos en nuestro trabajo, únicamente 2 no presentaban comorbilidad asociada con la enfermedad renal crónica, es decir, su puntuación en el ICC fue solo de 2 (la puntuación correspondiente a la enfermedad renal). El resto de pacientes, presentaron alguna de las patologías incluidas en el índice de Charlson, lo que refleja la elevada prevalencia de enfermedades asociadas en nuestra muestra de pacientes hemodializados. Nuestros resultados coinciden con los encontrados por Anaya Fernández y otros27 en España, con una puntuación de 7,4± 2,29 en su estudio.
Hay 2 razones que pueden explicar la alta tasa de morbi-mortalidad cardiovascular de los pacientes con IRC en los programas de terapia de remplazo de la función renal. La primera es la prevalencia aumentada de enfermedad cardiovascular entre los pacientes incidentes en diálisis, que se explica por el llamado síndrome cardiorrenal, ya que ambas entidades comparten similares factores de progresión. La segunda es el pronóstico fatal de los pacientes que ya tienen enfermedad cardiovascular previa. Por todo ello, estos pacientes deben ser considerados como un grupo de alto riesgo cardiovascular.
Todos estos sucesos se relacionan con el hecho de que en el paciente urémico, la patología cardiovascular no se explica únicamente por la elevada prevalencia de factores de riesgo aterogénicos "clásicos": edad, HTA, DM, dislilipemia, tabaquismo, historia familiar de enfermedad cardiovascular, HVI, sedentarismo, etc. Se postula la presencia de factores de riesgo aterogénicos "nuevos": hiperhomocisteinemia, hiperfibrinogenemia, elevación de lipoproteína (a), el estrés oxidativo, la inflamación, etc. y de factores de riesgo relacionados con el estado urémico: anemia, el estado hiperdinámico inducido por el acceso vascular, alteraciones del metabolismo calcio-fósforo, hiperparatiroidismo, acumulación de inhibidores endógenos de la síntesis de óxido nítrico, etc.28
Según algunas series se reporta que
Nuestra investigación muestra una frecuencia del 82 % más baja comparada con Longenecker y otros,31 en 1 041 pacientes donde estudió la prevalencia de los factores de riesgo cardiovasculares tradicionales en pacientes con ERC en diálisis y lo comparó con la población general del NANHES III, con una prevalencia de HTA que fue del 96 %, y Pernod y otros32 en su estudio que incluyó a 279 pacientes seleccionados al azar de 8 centros de diálisis, también seleccionados al azar (Francia, Italia y Suiza), donde encontró una prevalencia del 90 %. EE. UU. presenta el 80 %33 que resulta alta comparada con los resultados en España y el Reino Unido. En el estudio multicéntrico PRESDIAL,34 en el cual participaron 25 centros sanitarios de Cataluña, se incluyeron pacientes estables en hemodiálisis (6 meses o más en programa), y se encontró que el 69 % de los pacientes padecía HTA como comorbilidad. El registro renal del Reino Unido observó en diciembre de 2002 el 63 %.
]]> Los eventos cardiovasculares en nuestra serie se corresponden con la encontrada en el estudio MAR25,26 en el estudio prospectivo de una muestra representativa de pacientes en hemodiálisis en España, donde se recogen datos de comorbilidad cardiovascular y control de anemia de 1 710 pacientes. Al comparar nuestros datos con este estudio (tablas 4 y 5), confirmamos una mayor prevalencia de patología cardiovascular como cardiopatía, HVI, insuficiencia cardíaca, enfermedad vascular periférica, enfermedad cerebrovascular, también en relación con las encontradas en otras series.20El elevado riesgo cardiovascular que presentan los pacientes en HD es muy superior al de la población general,20,36 e incluso al de otros grupos reconocidos de pacientes de alto riesgo cardiovascular, lo cual puede explicarse por la elevada prevalencia de ECV, tanto clínica como subclínica. Cuando analizamos los factores predictivos de ECV y que de manera significativa se asociaron con ellas, encontramos que la edad, DM, hábito de fumar, dislipidemia, HTA, HVI y otros no clásicos como el peso, índice de comorbilidad y el tiempo en hemodiálisis, han sido descritos de igual manera en otras series,36-38 que fueron significativos en la prevalencia de ECV en nuestra muestra.
CONCLUSIONES
- Los pacientes con enfermedad renal crónica en hemodiálisis tienen una elevada frecuencia de ECV.
- La prevalencia de FRCV clásicos es alta en esta población.
- Los factores predictores de ECV clínica en nuestra población fueron la edad, la presencia de ECV subclínica (HVI) y FRCV clásicos (HTA, DM, dislipidemia, hábito tabáquico y edad).
RECOMENDACIONES
Se precisa un esfuerzo para tratar precoz (tal vez desde la etapa prediálisis) e intensamente los FRCV en estos pacientes, para intentar reducir su elevada morbi-mortalidad CV, a su llegada a HD.
]]>REFERENCIAS BIBLIOGRÁFICAS
1. Johnson CA, Levey AS, Coresh J, Levin A, Lau J, Eknoyan G. K/DOQI clinical practice guidelines for chronic kidney disease: evaluation, classification, and stratification. Part 7. Stratification of risk for progression of kidney disease and development of cardiovascular disease. Am J Kid Dis. 2004 Sep 1;70(5):869-76.
2. Herzog CA, Ma JZ, Collins AJ. Poor longterm survival after acute myocardial infarction among patients on longterm dialysis. N Engl J Med. 2006;339:799-805.
3. Mann JF, Gerstein HC, Pogue J, Bosch J, Yosuf S. Renal insufficiency as a predictor of cardiovascular outcomes and the impact of ramipril: the HOPE randomized trial. Ann Intern Med. 2001;134:629-36.
4. Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL Jr, et al. The seventh report of the joint national committee on prevention, detection, evaluation, and treatment of high blood pressure: the JNC 7 report. JAMA 2003;289:2560-2573.
5. Samak MJ, Coronado BE, Greene T. Cardiovascular disease risk factors in chronic renal insufficiency. Clin Nephrol. 2002;57:327-35.
6. Best PJ, Holmes DR. Chronic kidney disease as a cardiovascular risk factor. Am Heart J. 2008;145:383-86.
7. European Best Practice Guidelines for hemodialysis (part 1). Section VII. Vascular disease and risk factors. Nephrol Dial Transplant. 2006;17(supl 7):88-109.
8. Lidner A, Charra B, Sherrard DJ, Scribner BH. Accelerated atherosclerosis in prolonged maintenance hemodialysis. N Engl J Med. 1974;290:697-701.
9. Guérin AP, Pannier B, Marchais SJ, London GM. Cardiovascular disease in the dialysis population: prognostic significance of arterial disorders. Curr Opin Nephrol Hypert 2006;15105-10.
10.
11. Goicoechea M, García de Vinuesa M, Verdalles U, Ruiz-Caro C, Ampuero J, Rincón, et al. Effect of allopurinol in chronic kidney disease progression and cardiovascular disease. Clin JASN. 2010;5:1388-93.
12. Jofré R, Rodríguez-Benítez P, López-Gómez JM, Pérez-García R. Inflammatory syndrome in patients on hemodialysis. J Am Soc Nephrol. 2006;17:S274-80.
13. Laurent S, Cockcroft J, Van Bortel L, Boutouyrie P, Giannattasio C, Hayoz D, et al. Expert consensus document on arterial stiffness: methodological issues and clinical applications. European Heart J. 2006;27:2588-2605.
14. Taal MW, Sigrist MK, Fakis A, Fluck RJ, McIntyre CW. Markers of arterial stiffness are risk factors for progression to end-stage renal disease among patients with chronic kidney disease stages 4 and 5. Nephron Clinical Practice. 2007;107:177-81.
15. Goicoechea M, García de Vinuesa S, Gómez-Campderá F, Luño J. Predictive cardiovascular risk factors in patients with chronic kidney disease. Kidney Int. 2005;93:35-38.
16. Ortega M, Martínez J, Gamarra G. Mortality in patients with chronic renal failure during the first 90 days of hemodialysis therapy. Acta Med Colomb. 2006 Jan./Mar;31(1).
17. Pérez-García R, Martín-Malo A. Baseline characteristics of an incident haemodialysis population in
18. Henry RM, Kostense PJ, Bos G, Dekker JM, Nijpels G, Heine RJ, et al. Mild renal insufficiency is associated with increased cardiovascular mortality: the Hoorn study. Kidney Int. 2007;62:1402-07.
19. Junyent M, Martínez M, Borràs M, Betriu A, Coll B, Craver L, et al. Predicting cardiovascular disease morbidity and mortality in chronic kidney disease in Spain. The rationale and design of NEFRONA: a prospective, multicenter, observational cohort study.Nephrology Department, Institut de Recerca Biomèdica de Lleida at Hospital Universitari Arnau de Vilanova,
20. Collado S, Coll E, Deulofeo R, Guerrero L, Pons M, Cruzado Josep M, et al. Prevalencia de enfermedad cardiovascular en la uremia y relevancia de los factores de riesgo cardiovascular. Nefrologia. 2010;30(3):342. 8doi: 10.3265/Nefrologia.pre2010.Apr.10410.
21.
22. Shah DS, Polkinghorne KR, Pellicano R, Kerr PG. Are traditional risk factors valid for assessing cardiovascular risk in end-stage renal failure patients? Nephrology. 2008;13:667-71.
23. Charlson M, Szatrowski TP, Peterson J, Gold J. Validation of a combined comorbidity index. J Clin Epidemiol. 1994;47:1245-51.
24. Di Lorio B, Cillo N, Cirillo M, De Santo NG. Charlson Comorbidity Index is a predictor of outcomes in incident hemodialysis patients and correlations with phase angle and hospitalization. Int J Artif Organs. 2004;27:330-36.
25. Portolés J, López-Gómez JM, Aljama P. On behalf of the MAR Study Group. A prospective multicentre study of the role of anaemia as a risk factor in haemodialysis patients: The MAR Study. Nephrol Dial Transplant. 2007;22(2);500-7.
26. Portolés J, López Gómez JM, Aljama P, Tato AM. Riesgo cardiovascular en hemodiálisis en España: prevalencia, pautas de actuación y objetivos (estudio MAR) Nefrología. 2005;25:297-306.
27. Anaya S, Rivera F, Rodríguez-Perez JC, Rodríguez F. Uso del Indice de Charlson como predictor de mortalidad en ERC en hemodiálisis. Dial Traspl. 2009;30(1):18-20.
28. Craver L, Marco MP, Sarró F, Martín ML, Borràs M, Valdivielso JM, et al. Mineral metabolism influences pulse pressureiIncrease provoked by chronic kidney disease. Clin Nephrol. 2007;68:87-92.
29. Ureña Torres P, Prie D, Molina-Biétry V, Beck L, Silve C, Friedlander G, et al. Klotho: An antiagingprotein involved in mineral and vitamin D metabolism. Kidney Int. 2007;71:730-7.
30. Burnett Sherri-Ann M, Gunawardene SC, Bringhurst FR, Jüppner H, Lee H, Finkelstein JS. Regulation of C-terminal and intact FGF-23 by dietary posphate in mn and wmen. J Bone Mineral Res. 2006;21.
31. Longenecker JC, Coresh J, Powe NR,
32. Pernod G, Bosson JL, Golshayan D, Barro C, Forneris G, Martina G, et al. The Diamant Alpin Dialysis Cohort Study: clinico-biological characteristics and cardiovascular genetic risk profile of incident patients. J Nephrol. 2004;17:66-75.
33. Kanjilal S, Gregg EW, Beckles GL, Zhang P, Nelson DE, Mensah G, et al. Evolución de los factores de riesgo en EE. UU.Archives of Internal Medicine 2006 Nov;166(21):2348-55.
34. Poch E, Martínez X, Rodrigo JA, Tovar JL. Análisis de prevalencia y factores asociados a hipertensión arterial en hemodiálisis en Cataluña. Estudio PRESDIAL. XXXV Congreso Nacional de
35. Lidner A, Charra B, Sherrard DJ, Scribner BH. Accelerated atherosclerosis in prolonged maintenance hemodialysis. N Engl J Med. 1974;290:697-701.
36. Guérin AP, Pannier B, Marchais SJ, London GM. Cardiovascular disease in the dialysis population: prognostic significance of arterial disorders. Curr Opin Nephrol Hypertens. 2006;15:105-110.
37. Zoccali C. Cardiorenal risk as a new frontier of nephrology: research needs and areas for intervention. Nephrol Dial Transplant. 2002;17(Supl 11):50-4.
38. Rakhit DJ, Marwick TH, Armstrong KA, Johnson DW, Leano R,
Recibido: 30 de marzo del 2012. ]]> Aprobado: 1 de junio del 2012.
MSc. Mirna Caridad Atiés Sánchez. Instituto Nacional de Nefrología "Abelardo Buch López".