RESEARCH
Can Heberprot-P change the surgical concepts on treating diabetic foot?
¿Puede el Heberprot-P cambiar conceptos quirúrgicos en el pie diabético?
José I Fernández-Montequín1 and Llipsy Santiesteban2
1 Instituto de Angiología y cirugía vascular Calzada del Cerro # 1551, CP 12 000, Cerro, Ciudad de La Habana, Cuba ]]>
2 Hospital Hermanos Ameijeiras, Ciudad de La Habana, Cuba
ABSTRACT
Fourteen patients having diabetic foot ulcers on their limbs and who received amputation criteria at certain degree were included in this study, giving their consent to be treated. They were subjected to traditional medical-dietary and hygienic medical care, together with injections of Heberprot-P of 75 µg per vial being administered intralesionally in alternate days. A useful granulation tissue was developed in all the cases. All the patients preserved their limbs, regardless of the previous amputation criteria, following the ambulatory treatment.
Keyword: Heberprot-P, diabetic foot ulcer, surgical concept, Wagner classification
RESUMEN
El estudio incluyó catorce pacientes que presentaban úlceras de pie diabético, con criterio de amputación de cierto grado, quienes dieron su consentimiento para ser tratados. Se les aplicó los cuidados médico-dietéticos e higiénicos tradicionales, de conjunto con la administración de Heberprot-P de vial de 75 µg mediante inyección intralesional en días alternos. En los casos se pudo inducir tejido de granulación útil. Todos los pacientes preservaron sus extremidades, independientemente del criterio de amputación previo al tratamiento.
Palabras clave: Heberprot-P, úlcera de pie diabético, concepto quirúrgico, Clasificación de Wagner
]]> INTRODUCTION
Diabetic foot is currently recognized as a significant incapacitating illness among diabetic patients (1). Therefore, it has been declared as a relevant health problem by sanitary systems throughout the world. Considering that 60% of major amputations are applied to patients suffering from a vascular disease, and at the same time 60% of them are diabetic, then we have a tremendously important data in our hands. All these give us a warning on the risk for physical disability in those patients and their related irreversible depressing processes, which ultimately consolidate a new problem on their families and communities.
Surgical measures according to the anatomical damage of the foot are the response of the surgeon to these eventual complications (2), in a diabetic patient showing a lesion on his foot which is classified attending to the risk for the anatomy of that limb. Minor amputations are applied to necrotic and infected ulcers or bone damage, and major amputations to osteomyelitic ulcers of the calcaneous bone or when having tendon exposure. These procedures are presented to patients and their relatives who accept them with resignation in most of the cases, considering this apparently inevitable.
The search continues for medical solutions to treat the diverse lesions detected in the feet of diabetic patients. That led us to challenge the possibility of searching for cautious measures, to find optimistic and efficacious answers which would provide happiness to our patients.
How much is it possible to modify minor and major amputation ancestral criteria, established as medical practice, when deciding the treatment for an exposed bone, tendon, bone capsule, or a finger with a fistula affecting down into the bone?
Since 1999, the Center for Genetic Engineering and Biotechnology of Havana has created a new product based on Nepidermine. There has been also acquired a vast experience on using it to treat the diabetic foot, what was demonstrated through four research phases in more than 1000 cases from different countries. The product, commercially known as Heberprot-P® (3), has shown statistically significant scores with up to 85% of efficacy among the groups of diabetic foot patients to whom it was administered. There are no reports on the availability of any other product to treat this entity with such an amount of positive results.
Heberprot-P is a white lyophilized, sterile product, free from preservatives and designed for parenteral administration. It contains EGF at a dose of 75 µg per vial.
Its relevant pharmacological properties, according to previous clinical trials, are: 1) It makes it possible to establish and consolidate a useful and productive granulation tissue in diabetic patients with difficult cicatrization, including angiogenesis at the wound; 2) it stimulates the secretory phase within granulation, particularly in neuropathic patients whose granulation tissue is usually sloughed; and 3) it stimulates wound contraction and remodeling; these processes are normally absent, in part or completely, with diabetic complications.
The product was applied by the intralesional and perilesional routes. After diluting in 5 mL of injection water, 0.5 to 1.0 mL were infiltrated into the lesion with an appropriately thin needle at a depth of 0.1 cm. Antiseptic procedures were always followed when applying the drug. A phase of maximal clinical infection was avoided.
Therefore, our goal was to evaluate whether or not Heberprot-P would be able to avoid minor or major amputation of toes or the whole limb when administered to a group of diabetic foot patients, even in the presence of severe bone or tendon lesions.
]]> MATERIALS AND METHODSThe trials included 14 diabetic patients with lesions on their limbs, who had been informed of the need for limb amputation or partial exeresis due to the severity of their wounds. They received the traditional medical-dietary and hygienic medical care, and were treated at the diabetic foot service of the “Carlos Arvelo” Hospital in Caracas, Venezuela, every day or every two days, according to their clinical condition.
Treatment was given in an ambulatory manner. The studies and normal investigations used for this type of therapy were practiced for each patient; they always gave their consent before applying the product.
The lesions were:
- Ulcerative lesions of over 190 cm2 affecting the dorsal and plantar parts of the foot.
- Lesions with tendon and bone exposure.
- Ischemic calcaneous bone ulcers.
- Residual lesions at the post-surgical beds of the extraction of the internal saphenous vein for myocardial revascularization.
- Reconstruction of toes with bone lesions.
- Ulcerative-necrotic lesions of over 170 cm2 at the plantar area and at the calcaneus bone.
]]> - Osteomyelitic calcaneus bones.- Plantar perforating ulcer with bone fracture.
All patients were photographed before and after the treatment.
RESULTS
Ulcerative lesions of over 190 cm2 affecting the dorsal and plantar parts of the foot
Patient APA, a 57 year old male (Figure 1), insulindependent diabetic, classified as having an ischemic component since there was an absence of pedial pulses and a posterior tibial pulse at that limb. He had a large lesion affecting the plantar and dorsal parts of the foot. Dressings were carried out on alternate days. Necrotic and sloughed tissue was removed with a scalpel and forceps, without using any substance other than the locally applied physiological saline. He received up to 18 applications of Heberprot-P, having completed the treatment in 51 days. The doctor had proposed a supracondylar amputation of his limb before starting the treatment. Such indication was in agreement with international standards, since it was impossible to anatomically reconstruct the foot. The lesion healed completely and the patient was able to return to his work and social activities.
Two patients having lesions with bone and tendon exposure on the leg and foot
Patient MAV, a 49 year old male, with a perforating plantar ulcer as the gate of entrance of a Gram-negative bacterium producing abscesses at the dorsal part of the right foot, tendinous necrosis of tissues with the exposure at the external border of the astragalus bone and part of the calcaneus bone. The flexor tendon and muscles were exposed at the external area of the leg. It was classified as a Wagner grade 4 in spite of its neuroinfectious diabetic foot classification, due to the destruction of tissues and bone and tendon exposure (Figure 2).
Surgical treatments were applied under anesthesia and after hospitalization. Once the infection was controlled, the patient was sent to the diabetic foot service at the military hospital in an attempt to recover the limb. Local cures with surgical debridement were carried out in all the exposed areas, and an adequate hygienic-dietary and drug treatment was followed for all background diseases, including nephropathy.
The patient was informed on a possible recovery after eighteen months, although considered of poor prognosis due to the numerous exposed anatomical areas.
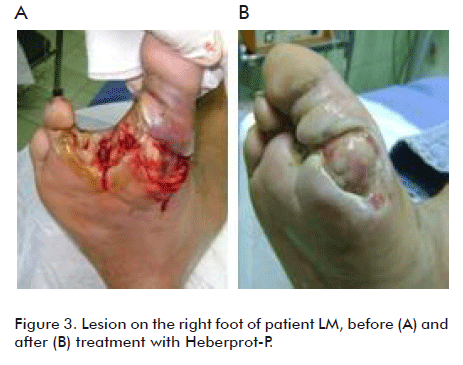
]]> In addition to the local cures indicated, local infiltrations of 75 µg Heberprot were applied at the bottom and the edges of the lesion to induce granulation in order to cover the exposed tendon and bone. The required granulation was achieved after 28 applications of Heberprot-P, covering the tendon area in 4 weeks. The patient was under treatment for 52 days and notably decreased blood creatinine during that time. Noteworthy, this product has also being reported as having cytoprotective properties.Patient LM, 39 year old male, an insulin-dependent diabetic, who entered the Surgery service with a completely abscessed lesion on his toes, for which reason several toes were amputated. Considering that limb amputation was imminent, the patient was taken as a last alternative to the diabetic foot service of the hospital, where an ambulatory treatment was started. A great deal of necrotic tissue was found with bone and tendon exposure at the base of his first toe. The posterior tibial pulse was absent, thereby evaluating the patient as ischemic. The patient was classified as having a Wagner grade 4 lesion because of the tissue damage present on the entire forefoot.
The dressings were very intensive with constant debridement of the lesion. Other physicians had indicated amputation following the surgical guidelines for bone and tendon exposure, a decision very discouraging for the patient. Very patiently, the bone capsule of the first toe and the flexor tendon were completely covered by useful granulation tissue after 30 applications of Heberprot-P. The treatment lasted 60 days (Figure 3).
In addition to the diabetes mellitus, this patient was a drug addict, but this was not a restriction for the application of the product.
Patient with an ischemic ulcer at the calcaneus bone
Patient JRL, a 66 year old male, insulin-dependent diabetic; he had had a stroke two years before and presented arterial hypertension. While under rehabilitation he presented an ischemic ulcer at the calcaneus bone (Figure 4). During the surgical treatment he underwent two surgical dressings under anesthesia to resect sloughed and ischemic tissue at the calcaneus area. The calcaneous bone was exposed and therefore limb amputation was indicated. The patient did not accept amputation and was taken to the Hospital, where he underwent the ambulatory treatment. He was classified as having ischemic Wagner grade 3 diabetic foot.
The local resection of the persistent sloughed and necrotic tissue was accompanied by 75 µg of Heberprot- P applied every two days to induce the production of granulation tissue. Hygienic-dietary and drug treatments were maintained for his original disease.
The patient received 18 applications until a useful granulation was achieved. He is currently under rehabilitation for the hemiplegia. Treatment was ambulatory.
Two patients with residual lesions at the post-surgical beds from the extraction of the internal saphenous vein for myocardial revascularization
]]> Patient MQM, 64 year old female, with diabetes type 1, having a successful myocardial revascularization by a coronary bypass with the internal safenous vein. However, since she had no peripheral pulses compromising the popliteal artery, the patient has developed a large 104 cm2 lesion at the inner face of the right leg, from where the safenous vein was extracted for the revascularization (Figure 5). Limb amputation was indicated, and the patient was then referred to the hospital.Treatment was started by infiltrating the bottom and edges of the lesion with 75 µg of Heberprot-P on alternate days, together with surgical debridement under local anesthesia. Granulation tissue and epithelialization on the edges of the lesion were obtained after 76 days with 36 applications through an ambulatory treatment.
Significantly, Heberprot-P is compatible for application in patients suffering from several conditions, since in this case, the patient is blind due to diabetic retinopathy, and also has a severe ischemic cardiopathy. No complications were observed during the treatment with the epidermal growth factor.
Patient JD, 77 year old male with type 2 diabetes who was subjected to myocardial revascularization to treat an ischemic cardiopathy, which left as a sequel a residual ulcer with a severe ischemic component at the inner face of the right leg (Figure 6). Limb amputation was indicated because no cure was possible, then his relatives brought him to the diabetic foot service at our clinic. The lesion was classified as being ischemic based on the absence of posterior tibial pulses and because it was classified as a Wagner grade 4.
Physical examination showed a long ulcer that was wide in the middle with an exposure of the tibia, which measured about 70 cm2. The treatment was started with local cures and continuous debridement. Twenty-five doses of Heberprot-P of 75 µg per vial were administered until granulation was obtained; the infiltrations were made at the bottom and the edges of the lesion.
This indication can be considered very novel within the Heberprot-P application guidelines.
Reconstruction of toes with bone lesions in three patients
Patient PA, 70 year old male, with type 2 diabetes showing a severe ischemic lesion resulting from trauma that became necrotic and gangrenous and was located at the distal portion of the middle toe. The lesion was classified as Wagner grade 3 (Figure 7). After a 30 day evolution toe amputation was indicated. After the routine tests were made, the physicians decided to apply 8 infiltrations of Heberprot-P. The procedure consisted of infiltrations made beneath the necrotic area of the toe, to delimit and raise the entire necrotic plaque. A final granulation area was established, which was used for the surgical reconstruction of the distal part of the toe. When the patient was discharged he was completely healed and very grateful because his toe remained with its original anatomy.
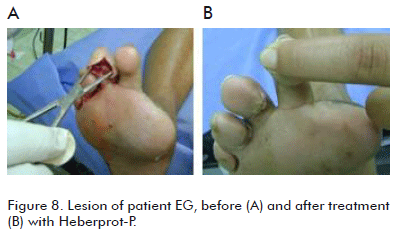
Patient EG, 53 year old female, having DM type 2; with a neuroinfectious Wagner grade 2 diabetic foot and having an abscess for ten day on her middle toe. After examining the lesion it was found that it covered up to the corresponding metatarsal bone with an osteoporotic lesion and an osteolytic area at one border as shown by the X-rays (Figure 8). Wound depth was verified by introducing a Kelly forceps. Local dressings were made on the toe, which was at risk of amputation. Heberprot-P was applied seven times within the lesion that was measured with the forceps, so as to generate a useful granulation tissue covering the bone area. The granulation tissue formed covered the bone and the toe was reconstructed, for the pleasure and well-being of the patient. The patient was finally discharged, completely healed.
Ulcerative-necrotic lesions in the plantar and calcaneus areas and larger than 170 cm2
Patient CO, 60 year old female, with type 2 diabetes mellitus for two years. She had a clinical record of a lesion with abscesses in the plantar area with an evolution of 180 days (Figure 10). After debridement, limb amputation was indicated but the patient refused and began to dress the lesion herself at home, disinfecting it. Upon arrival at the service, she presented a lesion of 172 cm2 that was classified as neuroinfectious Wagner grade 3 diabetic foot. The lesion affected the plantar and calcaneus areas, with a complete separation between the tissue and the heel bone. Surgical debridement was carried out and 24 infiltrations of injectable Heberprot-P were applied, achieving a useful granulation and successful attachment of the tissue to the heel bone. The patient also recovered from a lesion at the border of the foot. This represented another possible recovery for an anatomically highly compromised foot.
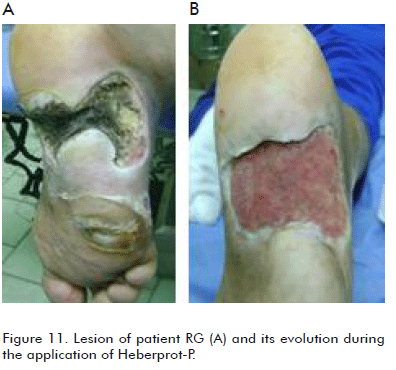
Patient RG, a 29 year old female, with known type 1 diabetes mellitus for six years. She had a huge abscess at the plantar area, plenty of necrotic tissue and an aggressive Pseudomonas aeruginosa infection in that area, infiltrating the calcaneus bone. The plantar zone was compromised not only because of the pus it was draining, but also because of the anatomical separation of the bottom and edges (Figure 11). The case was classified as Wagner grade 4 neuroinfectious diabetic foot. Repetitive surgical scrubs at the outpatient service were required, with intravenous antibiotic treatment. After having improved clinically from the local infection, Heberprot-P was infiltrated to obtain local granulation. The lesion was of 420 cm2; it was completely covered by the granulation tissue, and above all, through serial infiltrations in the two laminae of the tissue of the calcaneus area, we were able to attach both parts thereby covering the entire bone area. Therefore, the patient preserved her limb from the two major amputations previously indicated.
Patient GP, 50 year old male, with known type 2 diabetes mellitus for more than 10 years. He had a lesion with abscess at the plantar aspect and forefoot with an evolution of 120 days. It was classified as a neuroinfectious very large Wagner grade 4 diabetic foot. Surgical scrubs were applied and the lesion was infiltrated with 19 applications of Heberprot-P, producing a reduction of the area of up to 18 cm2. The patient developed a hypergranulation response which was treated with silver nitrate to favor epithelialization (Figure 12).
Osteonecrotic calcaneus bone
Patient GB, 77 year old male with type 2 diabetes mellitus, who was very careless; had a lesion at the heel of the right foot, with an exposure of the calcaneus bone due to loss of the surrounding tissue. In addition to the medical control, hygiene and dietetic measures, local surgical dressings were applied and all the osteonecrotic area was resected with a gouge down to near the marrow. Thirty two Heberprot-P infiltrations were made around the calcaneus bone, so that the tissue would cover all the resected area. A useful granulation tissue was induced. This patient was treated abroad, and returned home 60 days after ending the treatment. Only local dressings were applied on the ulcer with physiological saline, which was completely healed 45 days after he was discharged (Figure 13).
Plantar perforating ulcer with added bone fracture
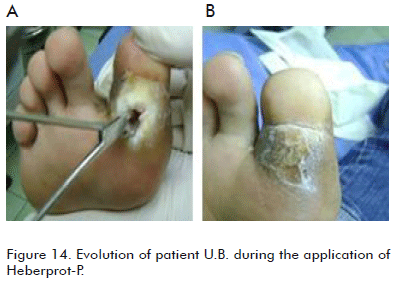
Patient UB, a 28 year old female and with type 1 diabetes mellitus for 18 years. She had a plantar perforating ulcer for 60 days at the base of her first toe, which penetrated into the bone. (Figure 14). Through X-rays we found that the wounded toe had a distal fracture of that phalange. Local surgical cures were applied and five doses of Heberprot-P were infiltrated into the walls of the ulcer to favor the granulation covering the bone fracture, which was achieved after 15 days. The patient then returned to her normal life.
]]>
DISCUSSION
All the fourteen cases presented here had been previously submitted for amputation, either minor or major, of the affected limb. Major amputations have been commonly associated to the diabetic foot diagnosis, with some authors reporting up to a 60% probability for applying such procedures to the affected population.
The use of a proper technique to deal with a diabetic foot while having a product like Heberprot-P available, which is able to consistently induce the growth of productive granulation tissue after the first six doses, replaces the amputation criteria as first choice to manage this type of lesions.
CONCLUSIONS
The surgical experience carried out on these fourteen patients was presented, and the responses for the different types of lesions were shown. These were lesions that may be found in the limbs of diabetic patients and that may be treatment variants to normal surgery, in spite of the reports in the literature. The Cuban product Heberprot-P offers many therapeutic possibilities for these patients.
REFERENCES
1. Wild S, Roglic G, Green A, Sicree R, King H. Global prevalence of diabetes: estimates for the year 2000, and projections for 2030. Diabetes Care. 2004; 27(5):1047-53.
2. Boulton AJ, Vileikyte L, Ragnarson-Tennvall G, Apelqvist J. The global burden of diabetic foot disease. Lancet 2005; 366(9498):1719-24.
3. Heberprot-P - Atención integral al paciente con pie diabético + Heberprot-P (página web). Disponible en: http://heberprot-p.cigb.edu.cu/ (Consultado: 24 de agosto de 2010).
Received in August, 2010.
Accepted for publication in September, 2010.
José I Fernández-Montequín, Instituto de Angiología y cirugía vascular Calzada del Cerro # 1551, CP 12 000, Cerro, Ciudad de La Habana, Cuba. E-mail: fdez_montequin@yahoo.es
]]>