Pemphigus vulgaris: a review of 12 cases
Pénfigo vulgar: revisión de 12 casos
Ana Carolina Vasconcelos,I Sergio Augusto Miguens Jr,II Maria Antonia Figueiredo,I Fernanda Gonçalves Salum,I Karen CherubiniI
I Pontifical Catholic University of Rio Grande do Sul Brasil/Dental School. Brasil.
II Universidade Luterana do Brasil/Dental School. Brasil.
ABSTRACT
Introduction: pemphigus vulgaris is an autoimmune mucocutaneous disease, which presents at clinical examination as blisters, erosions and ulcerations of the skin and mucous membranes.
Objective: the aim of this study was to review 12 cases of pemphigus vulgaris diagnosed at the Stomatology Department of São Lucas Hospital, Pontifical Catholic University of Rio Grande do Sul.
Methods: the medical charts were analyzed considering patients age and sex; anatomic site and clinical aspect of the lesions; as well as symptoms, duration and clinical course of the disease.
Results: the mean age of the patients was 46.7 years; most of cases occurred in females (75.0 %); buccal mucosa was the site most frequently affected (83.3 %), and 25 % of cases showed extraoral manifestations. Erosion/ulceration was the most prevalent clinical appearance (83.3 %), and pain occurred in 100% of cases. The mean time of development of the lesions reported by the time of the diagnosis was 12.3 months, and the mean time of follow-up was 2 years. All patients received systemic therapy with prednisone, meanwhile in 58.3 % of cases it was associated with topic therapy and in 25 %, with systemic immunosuppressive therapy. One case (8.3 %) remained in remission regardless of the treatment withdrawal.
Conclusion: Pemphigus vulgaris is a disease with important morbidity, which requires the attention of the dentist as a way to achieve early diagnosis.
Key words: pemphigus vulgaris, mouth disease, immunosuppressive therapy.
RESUMEN
]]> Introducción: el pénfigo vulgar es una enfermedad autoinmune mucocutánea, que presenta al examen clínico ampollas, erosiones y ulceraciones de la piel y de las membranas mucosas.Palabras clave: pénfigo vulgar, enfermedad oral, terapia inmunosupresora.
INTRODUCTION
The word pemphigus comes from the Greek (pemphix= blister) and calls a rare group of autoimmune mucocutaneous diseases, which presents at clinical examination as blisters, erosions and ulcerations of the skin and mucous membranes1-4 as a result of loss of cellular adhesion.1-5 The group comprises different forms of pemphigus: vulgaris, foliaceous, vegetans, erythematosus and paraneoplastic.5 Pemphigus vulgaris is the most prevalent, even though its incidence is low, which ranges from 0.1 to 0.5 cases per 100,000 individuals.6-9 The condition can be observed more frequently in people from the Mediterranean area and among those of Jewish ancestry, which suggests a genetic predisposition.2,3,5-7 The disease affects wide age range, with higher prevalence in the fifth and sixth decades of life.6,8,9 Some studies have reported preference for female,9-11 whereas others show no difference of prevalence between sexes.6,12
Pemphigus develops as a result of the interaction between genetic and environmental factors. Among the latter, vaccines, herpes simplex virus, varicella zoster, Epstein Barr virus, cytomegalovirus and human immunodeficiency virus have been associated as triggers or agonists. It is believed that such agents are able to stimulate an immune response in genetically susceptible people.3,4 Autoantibodies IgG, particularly IgG1 and IgG4, are directed against cell adhesion glycoproteins, the desmogleins.2,5,6 Desmoglein 3 is preferentially expressed in oral epithelium, while desmoglein 1 can be observed in the superficial layer of epidermis.7
In approximately 70 % to 90 % of cases, the oral mucosa is the first site of disease manifestation, and it can be the only site affected in more than 50 % of patients.10 Pemphigus vulgaris is characterized clinically by the presence of blisters affecting skin and/or mucosa, especially in the buccal mucosa, palate, ventral surface of the tongue and lips. The blisters rupture quickly leading to the appearance of painful erosions and ulcerations 2,5. Positive Nikolsky's sign highlights the fragility of the mechanism of cellular adhesion.13,14 The ulcers can also affect other mucous membranes including nasal, genital, conjunctiva, pharynx, larynx and esophagus.6,10,15 Erythema multiforme, erosive lichen planus, candidiasis, pemphigoid, herpes simplex and recurrent aphthous ulceration should be included in the differential diagnosis.6,13,15,16
The diagnosis is based on clinical and histological examination. The latter shows an intraepithelial gap above the basal layer of the epithelium, whereas this layer remains firmly attached to the connective tissue, with cells in a tombstone-like arrangement. Within the intraepithelial cleft, there are the typical rounded acantholytic Tzanck cells, which stand out from the spinous layer of the epithelium,7,8,13,15 and can be observed also in exfoliative cytology. An inflammatory infiltrate, ranging from mild to moderate, is observed in the connective tissue.4,9.14 Diagnostic confirmation is provided by direct immunofluorescence of fresh perilesional tissue presenting intercellular antibodies IgG, IgM and complement components (C3).15 Indirect immunofluorescence shows circulating (serum) antibodies.7,8 This test is typically positive in about 90 % of cases, and may be useful in patients who have contraindication for biopsy.7,12,13 Upper endoscopy should be recommended in cases of pemphigus vulgaris in which there is complaint of dysphagia, to detect possible esophageal involvement.10
]]> Corticosteroid is the drug of choice for the treatment of pemphigus vulgaris. Its introduction in the pharmaceutical market in the early 50's, reduced the mortality of the disease in a range of 10 %-90 %.2,6,8,12,17,18 The association with topical therapy and with immunosuppressive agents is indicated because it allows the use of lower doses of corticosteroid and thus reduce its side effects.19 The present study reviewed 12 cases of pemphigus vulgaris, considering clinical features and therapeutic approach to the disease.
METHODS
The medical charts of 12 patients with pemphigus vulgaris attended at the Stomatology Department of São Lucas Hospital - Pontifical Catholic University of Rio Grande do Sul (PUCRS) were evaluated. All cases had diagnosis confirmed by histological examination performed using hematoxylin and eosin stain (H & E). The charts were reviewed considering the following variables: patients age and sex, anatomical site and clinical aspect of lesions, symptoms, duration and clinical course of the disease. The results were analyzed using descriptive statistics.
RESULTS
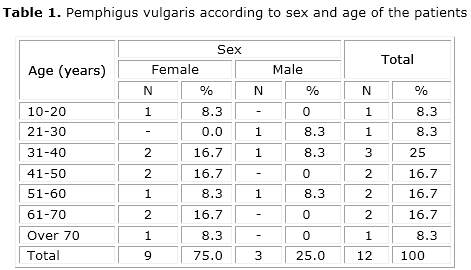
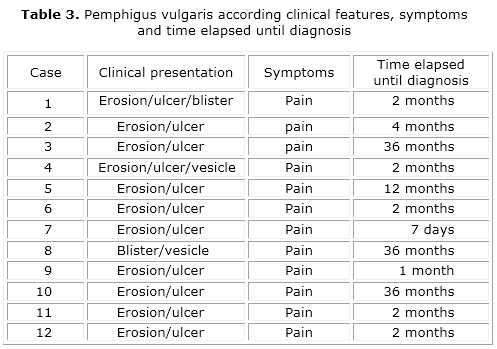
The mean age was 46.7 years, whereas the youngest patient was 19 years old and the oldest was 74. Women were the most affected, representing 75 % of cases (table 1). Buccal mucosa was the most frequent site (83.3 %), and 25 % of the cases had extraoral manifestations (table 2). Table 3 displays the distribution of lesions according to clinical presentation, symptoms and time elapsed until diagnosis. The ulcerated/erosive clinical presentation was the most prevalent (91.7 %), and pain was present in 100 % of cases. The time course of lesions development reported at the patients’ first visit ranged from 7 days to 36 months, with a mean of 12.3 months. Table 4 shows the distribution of cases according to the clinical course. All patients received systemic therapy with prednisone. In 58.3 % of cases there was association with topical therapy and in 25 %, with immunosuppressive therapy. One case (8.3 %) remained in remission after therapy withdrawal.
]]>
DISCUSSION
In the present study, the age most affected by pemphigus vulgaris ranged from 31 to 40 years, with a mean age of 46.7 years, which confirms reports in the literature.10,11,13 We also observed that occurred mainly in women. Although some studies claim there is no predilection for sex,6,12 preference for females has been observed by some other authors.9-11,17
Buccal mucosa was the most frequently affected site, erosive/ulcerated clinical presentation was the most prevalent, and pain was present in all of cases. These findings are similar to those observed by Sirois et al.13 in a retrospective study of 42 cases of pemphigus vulgaris. Skin was the main affected extraoral site, which is in accordance to Ishii et al.11 and Robinson et al.9
Similarly to the study of Robinson et al.,9 all cases in this study started treatment with prednisone in doses ranging from 40 mg to 80 mg. Other therapies such as azathioprine, cyclophosphamide, cyclosporine, methotrexate, and dapsone are usually given to the patients unresponsive to conventional therapy or who have complications from corticotherapy.17,20-23 Plasmapheresis, cholinergic agonists and immunoglobulin administered intravenously are recent therapies for autoimmune diseases.9,10,17,24-28 Dexamethasone, triamcinolone acetonide and fluticasone propionate have also been used successfully as topical therapy in oral lesions.6,20 In this study, patients received immunosuppressive therapy associated with systemic steroids, systemic steroids were associated with topical therapy. Robinson et al.9 found that 12 patients (100 %) received immunosuppressants, as well as systemic and topical steroids. This represents the different pathways in monitoring immunosuppressive therapy, which varies according to clinical response of each patient. Approximately 75 % of the pemphigus vulgaris patients show remission of the symptoms after 10 years of treatment.9 In this study, we observed one case with complete remission after 4 months of therapy withdrawal. In neither case follow-up treatment it lasted more than 10 years, due to death or treatment abandonment. Robinson et al.9 found that in 75 % of cases there was at some point, complete remission without the use of any medication. These authors also noted that the time between recurrences was significantly increased in patients treated for over 6 years indicating that the severity of the disease tends to diminish with continued treatment. Pemphigus vulgaris is a serious disease with important morbidity, whose first signs often occur in oral mucosa. The knowledge and attention of the dentist to its clinical manifestations can favor the early diagnosis of the disease.
1. Mimouni D, Nousari CH, Cummins DL, Kouba DJ, David M, Anhalt GJ. Differences and similarities among expert opinions on the diagnosis and treatment of pemphigus vulgaris. J Am Acad Dermatol. 2003;49(6):1059-62.
2. Scully C, Mignogna M. Oral mucosal disease: pemphigus. Br J Oral Maxillofac Surg. 2008;46(4):272-7.
]]>3. Sagi L, Sherer Y, Trau H, Shoenfeld Y. Pemphigus and infectious agents. Autoimmun Rev. 2008;8(1):33-5.
4. De Simone C, Caldarola G, D'agostino M, Zampetti A, Amerio P, Feliciani C. Exacerbation of pemphigus after influenza vaccination. Clin Exp Dermatol. 2008;33(6):718-20.
6. Guillen S, Khachemoune A. Pemphigus vulgaris: a short review for the practitioner. Dermatol Nurs. 2007;19(3):269-72.
8. Khelifa E, Benmously R, Badri T, Debbiche A, Ben Ayed M, Mokhtar I, Fenniche S. Pemphigus vulgaris presenting as an isolated crusted plaque of the cheek. Dermatol Online J. 2009;15(6):6.
]]>9. Robinson JC, Lozada-Nur F, Friden I. Oral pemphigus vulgaris: a review of the literature and a report on the management of 12 cases. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1997;84(4):349-55.
10. Mignogna MD, Lo Muzio L, Galloro G, Satriano RA, Ruocco V, Bucci E. Oral pemphigus: clinical significance of esophageal involvement: report of eight cases. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1997;84(2):179-84.
11. Ishii N, Maeyama Y, Karashima T, Nakama T, Kusuhara M, Yasumoto S, Hashimoto T. A clinical study of patients with pemphigus vulgaris and pemphigus foliaceous: an 11-year retrospective study (1996-2006). Clin Exp Dermatol. 2008;33(5):641-3.
12. Perez OA, Patton T. Novel therapies for pemphigus vulgaris: an overview. Drugs Aging. 2009;26(10):833-46.
13. Sirois D, Leigh JE, Sollecito TP. Oral pemphigus vulgaris preceding cutaneous lesions: recognition and diagnosis. J Am Dent Assoc. 2000;131(8):1156-60.
]]>14. Mignogna MD, Fortuna G, Leuci S, Ruoppo E, Marasca F, Matarasso S. Nikolsky's sign on the gingival mucosa: a clinical tool for oral health practitioners. J Periodontol. 2008;79(12):2241-6.
15. Dagistan S, Goregen M, Miloglu O, Cakur B. Oral pemphigus vulgaris: a case report with review of the literature. J Oral Sci. 2008;50(3):359-62.
16. Daneshpazhooh M, Chams-Davatchi C, Ramezani A, Moinedin F, Hemami MR. Abortive aphthous-like oral lesions: an underreported initial presentation of pemphigus vulgaris. J Eur Acad Dermatol Venereol. 2009;23(2):157-9.
17. Mignogna MD, Leuci S, Fedele S, Ruoppo E, Adamo D, Russo G, Pagliuca R. Adjuvant high-dose intravenous immunoglobulin therapy can be easily and safely introduced as an alternative treatment in patients with severe pemphigus vulgaris: a retrospective preliminary study. Am J Clin Dermatol. 2008;9(5):323-31.
18. Sethy PK, Khandpur S, Sharma VK. Randomized open comparative trial of dexamethasone-cyclophosphamide pulse and daily oral cyclophosphamide versus cyclophosphamide pulse and daily oral prednisolone in pemphigus vulgaris. Indian J Dermatol Venereol Leprol. 2009;75(5):476-82.
]]>19. Miletta N, Miller ME, Lam T, Chung KK, Hivnor C. The Management of Pemphigus Vulgaris in a Burn Intensive Care Unit: A Case Report and Treatment Review. J Burn Care Res . 2014 Feb 25. [Epub ahead of print].
20. Hapa A, Gurpinar A, Akan T, Gokoz O. A resistant case of pemphigus gestationis successfully treated with intravenous immunoglobulin plus cyclosporine. Int J Dermatol. 2014;53(4):e269-71.
21. Hocar O, Zidane W, Laissaoui K, Akhdari N, Amal S. Herpes infection in pemphigus. Med Mal Infect. 2009;39(1):64-5.
22. Tran KD, Wolverton JE, Soter NA. Methotrexate in the treatment of pemphigus vulgaris: experience in 23 patients. Br J Dermatol. 2013;169(4):916-21.
23. Moreno AC, Santi CG, Gabbi TV, Aoki V, Hashimoto T, Maruta CW. IgA pemphigus: case series with emphasis on therapeutic response. J Am Acad Dermatol. 2014;70(1):200-1.
]]>24. Fania L, Zampetti A, Guerriero G, Feliciani C. Alteration of cholinergic system in keratinocytes cells produces acantholysis: a possible use of cholinergic drugs in pemphigus vulgaris. Antiinflamm Antiallergy Agents Med Chem . 2012;11(3):238-42.
25. Gürcan HM, Ahmed AR. Analysis of current data on the use of methotrexate in the treatment of pemphigus and pemphigoid. Br J Dermatol. 2009;161(4):723-31.
26. Arnold DF, Burton J, Shine B, Wojnarowska F, Misbah SA. An 'n-of-1' placebo-controlled crossover trial of intravenous immunoglobulin as adjuvant therapy in refractory pemphigus vulgaris. Br J Dermatol. 2009;160(5):1098-102.
27. Grando SA, Bystryn JC, Chernyavsky AI, Frusić-Zlotkin M, Gniadecki R, Lotti R, et al. Apoptolysis: a novel mechanism of skin blistering in pemphigus vulgaris linking the apoptotic pathways to basal cell shrinkage and suprabasal acantholysis. Exp Dermatol. 2009;18(9):764-70.
28. Ruocco E, Wolf R, Ruocco V, Brunetti G, Romano F, Lo Schiavo A. Pemphigus: associations and management guidelines: facts and controversies. Clin Dermatol. 2013;31(4):382-90.
]]>
Recibido: 22 de enero de 2015.
Aprobado: 6 de febreo de 2015.
Ana Carolina Vasconcelos. Av. Ipiranga, 6681 - Partenon, Porto Alegre - RS, Zip Code: 90619-900, Brazil.
Correo electrónico: carolinauv@hotmail.com