Caracterización de los pacientes con cáncer de colon
Characterization of patients with colon cancer
Dr. Luis Andrés Guibert Adolfo; Dr. Luis Ernesto Quiroga Meriño; Dra. Yarima Estrada Brizuela; Dr. Osmany Mario Maestre Ramos; Dr. Germán Guilarte León.
Hospital Militar Universitario Dr. Octavio de la Concepción de la Pedraja. Universidad de Ciencias Médicas de Camagüey. Camagüey, Cuba.
DeCS: NEOPLASIAS DEL COLON/cirugía; ADENOCARCINOMA; ESFINTEROTOMÍA ENDOSCÓPICA; ANCIANO; ESTUDIOS TRANSVERSALES.
ABSTRACT
Background: colon cancer is the third more frequent cause of morbidity and mortality for cancer in the world.
Objective: to characterize the patients with colon cancer. ]]>
Methods: a transversal and descriptive study was carried out aimed at characterizing patients with colon cancer in the Service of General Surgery of the Military Hospital Octavio de la Concepción y la Pedraja from October 2013 to August 2017. The universe was compound for 61 patients diagnosed with colon cancer.
Results: women prevailed in the study. Patients older than 60 years were the majority, specifically those from the 70 to 79 age group. The hairy adenoma is the more frequent antecedent followed by the ulcerative colitis. The low digestive bleeding was the form of predominant presentation in the patients and the left localization of the tumor was the most frequent. In most of the patients the colon cancer was well differentiated. The adenocarcinoma is the more frequent histological type.
Conclusions: women prevailed between 70 and 79 years with adenomas as pathological antecedents. Digestive bleeding was the clinical form of more frequent presentation, and it was associated to left localization. A part of the studied patients required surgical intervention and the most used technique was the left hemicolectomy. Most of the neoplasias were well differentiated with chronic inflammation.
DeCS: COLONIC NEOPLASMS/surgery; ADENOCARCINOMA; SPHINCTEROTOMY, ENDOSCOPIC; AGED; CROSS-SECTIONAL STUDIES.
INTRODUCCIÓN
El cáncer colorrectal, como problema de salud pública, es creciente en el mundo, el aumento en la expectativa de vida de las poblaciones, la mayor exposición a carcinógenos reconocidos, la ampliación de la cobertura de los programas de salud, el continuo mejoramiento de las técnicas de tamizaje y la búsqueda activa de casos, son las razones por las cuales cada año se informa un aumento en el número global de casos diagnosticados con cáncer. Según datos del Instituto Nacional de Salud de Estados Unidos, en este país ocurren más de 500 000 muertes cada año a consecuencia de esta enfermedad. Incidencia de la cual no escapa Cuba donde se estima que el 35 % de la población sufrirá de un tumor maligno para alrededor del 2030. 1-3
El cáncer de colon es la tercera causa más frecuente de morbilidad y mortalidad por cáncer en el mundo tanto para hombres como mujeres. Las tasas de incidencia y mortalidad estandarizadas por edad por 100 000 personas-año para 2008 fueron 17,2 y 8,2. El cáncer de colon es un importante problema de salud pública en todo el mundo, en especial en los países ricos. 4,5
Aunque la incidencia y la mortalidad por cáncer de colon han declinado en los últimos años en América, es la tercera causa más común de mortalidad por cáncer. Más de 155 000 personas mueren cada año por esta causa y se diagnostican 140 000 nuevos casos al año. 6-9
En Cuba en el año 2016 fallecieron 2 331 pacientes por esta causa. Lo cual constituyó la cuarta causa de muerte por tumores malignos, lo que representa 20,7 pacientes cada 100 000 habitantes. 2-7
]]> El tratamiento más efectivo para este tipo de neoplasia es el quirúrgico y su objetivo es extirpar todo el tejido maligno y un margen adecuado de tejido sano, al mismo tiempo con su territorio de drenaje linfático, disminuye al mínimo la morbilidad y mortalidad relacionada con este procedimiento. La técnica quirúrgica en cada caso depende de su estadio, de su localización y de la presencia de otras lesiones colorrectales y de la extensión a otros órganos. 10El pronóstico de estos tumores está relacionado de manera directa con la precocidad del diagnóstico y está demostrado que guarda una estrecha relación con su grado de penetración en las paredes del órgano, con la afectación de los ganglios linfáticos regionales, con la invasión de los órganos vecinos y con la existencia de metástasis a distancia, por ello es tan útil su estadificación para establecer un pronóstico. La aparición de complicaciones, que por lo general está relacionada con la demora en el diagnóstico, es un hecho que influye de manera negativa en el pronóstico, pues aumenta de manera notable la mortalidad. 11,12
Por lo que se decidió realizar el estudio y caracterizar a los pacientes con cáncer de colon en el servicio de Cirugía General con el propósito de ampliar los conocimientos del mismo y las formas más eficaces de tratarlo.
MÉTODOS
La investigación constituyó un estudio de desarrollo de tipo descriptivo transversal con el objetivo de caracterizar los pacientes con cáncer de colon en el Servicio de Cirugía General del Hospital Militar Octavio de la Concepción de la Pedraja desde octubre de 2013 hasta agosto de 2017. El universo estuvo compuesto por 61 pacientes con diagnóstico de cáncer de colon, atendidos en el Servicio de Cirugía General durante el periodo de tiempo antes señalado. Los criterios de inclusión fueron: ser diagnosticado con cáncer de colon y la confirmación del tipo histológico por biopsia, mientras los de exclusión fueron: la imposibilidad para recolectar la información y la no confirmación por biopsia.
Recolección y análisis de la información
Los datos provenientes de la revisión de las historias clínicas fueron recogidos en un formulario, que incluyó las variables tales como edad, sexo, antecedentes patológicos personales, formas de presentación clínica y características patológicas de las neoplasias, este se confeccionó a propósito de la investigación y basado en la información teórica revisada. Se creó una base de datos en SPSS que permitió el procesamiento de los mismos mediante técnicas de estadística descriptiva e inferencial.
Se emplearon herramientas de estadística descriptivas consistentes en distribución de frecuencias absolutas y relativas, contraste de proporciones y determinación de la significación del contraste mediante X2 con nivel de significación de 95 %.
]]> RESULTADOS
El aumento progresivo de pacientes con cáncer, constituyen un reto para la medicina actual; el desarrollo de métodos diagnósticos y el acceso a la medicina han reducido el tiempo para el diagnóstico en fases más tempranas de la enfermedad y con ello un incremento en las cifras reportadas cada año.
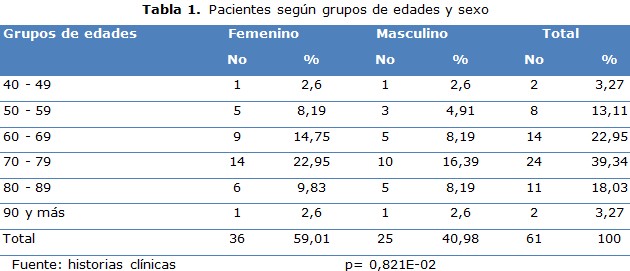
Se distribuyeron pacientes según grupos de edades y sexo en la cual predominaron las mujeres (59,01 %) sobre los hombres (40,98 %). En cuanto a los grupos de edades, los pacientes mayores de 60 años resultaron la mayoría y en específico los situados en el grupo de 70-79 años (39,34 %) (tabla 1).
Se analizó la distribución de los pacientes según antecedentes patológicos personales, alrededor de un tercio de los pacientes carecía de antecedentes patológicos personales relacionados con el cáncer de colon (29,50 %). El adenoma velloso resultó el antecedente más frecuente (34,42 %) seguido de la colitis ulcerativa (14,75 %). La diverticulosis de colon (11,47 %) y poliposis (9,83 %) se reportaron en menor número de pacientes (tabla 2).
La distribución de los pacientes según presentación clínica en relación a la localización de la neoplasia, el sangrado digestivo bajo resultó la forma de presentación predominante en los pacientes estudiados (37,60 %), seguido del síndrome anémico (29,50 %), síndrome oclusivo (24,59 %) y síndrome general (8,06 %). El cáncer de colon predominó en la localización izquierda (60,65 %) (tabla 3).
En la se analizó las características patológicas de las neoplasias, en la mayor parte de los pacientes el cáncer de colon estaba bien diferenciado (47,64 %) y presentaba evidencias de inflamación crónica (70,49 %) (tabla 4).
]]>DISCUSIÓN
En la investigación se encontró predominio del sexo femenino y pacientes mayores de 60 años, lo cual coincide con lo reportado por Ferreira EJ y Meléndez HJ, 13 en su estudio donde evidenciaron que la media de edad de sus pacientes con cáncer de colon fue de 62 años y existió un predominio del sexo, resultados estos que a pesar de incluir en su serie a pacientes intervenidos de urgencia coinciden con lo reportado en el trabajo.
Montes de Oca Megías E et al. 14 reportan un promedio de edad de 61,5 años, con predominio del sexo femenino, señalan además que el 85 % de los casos de cáncer de colon ocurre en individuos de más de 60 años y que en Europa la incidencia del mismo aumenta con la edad, a esto contribuyen factores ambientales y del estilo de vida, con una tendencia al aumento en el sexo masculino a partir de los 50 años.
Neuhouser ML et al. 15 en Estados Unidos reportan incidencia similar del cáncer de colon para ambos sexos, con un incremento después de los 40 años y que el 90 % de los casos ocurren en mayores de 50 años; en la actualidad existe una tendencia a diagnosticarse en personas más jóvenes, se encuentra dentro de los 10 diagnósticos más comunes en individuos entre los 20 y 49 años. 16
En la región de Latinoamérica se han descrito resultados similares. En Colombia, reportan que la edad media para padecer de cáncer de colon es de 54 años, con predominio femenino. 17-19
Otros autores como Ojima T et al. 20 reportan en los 76 informes estudiados sobre caracterización videoendoscópica de cáncer de colon, que el paciente de menor edad tenía 26 años y el de mayor edad 86 años, para un promedio de edad de 62 años, predominaron los pacientes en edades entre 50 y 64 años.
La presencia de adenomas vellosos se ha asociado a la aparición de cáncer de colon la mayor parte de ellos, sea cual sea su causa, derivan de pólipos adenomatosos. Sólo los adenomas son premalignos, y una minoría de ellos se transforma en cáncer. Los estudios de detección sistemática en la población y las necropsias han revelado que los pólipos adenomatosos de colon se pueden encontrar en más del 30 % de las personas de edad mediana o avanzada. A pesar de esto, menos de 1 % de los pólipos llegan a hacerse malignos y una gran parte de los pólipos no producen síntomas y permanecen sin ser detectados de forma clínica. 21-24
Los antecedentes patológicos familiares y personales de cáncer de colon, constituyen factores de riesgo importantes para el desarrollo de este tumor según Malvezzi M et al. 25 estos señalan además que los pacientes que presentan antecedentes de cáncer de colon familiar, presentan un riesgo incrementado de dos a seis veces de padecer la enfermedad, a lo que se le suma el número de familiares afectos, el grado de parentesco y la edad de diagnóstico de la neoplasia; de la misma forma, el riesgo aumenta cuando existen antecedentes familiares de pólipos adenomatosos colónicos, en especial si han sido diagnosticados antes de los 60 años de edad.
En cuanto a la presentación clínica, el sangramiento digestivo bajo predominó en la mayoría de los pacientes de la investigación, lo que pudiera estar en relación a la localización predominante del cáncer en el sigmoides, autores como Adams SA et al. 26 reportan resultados similares.
]]> Otros autores como Hano García OM, et al, 28 reportan como principal hallazgo al examen físico la presencia de masa abdominal y como hallazgo inespecífico, el dolor a la palpación fue positivo en más de un tercio de los pacientes. Lynch HT et al. 29 señalan que la prueba de sangre oculta en heces fecales empleada, presenta una sensibilidad y especificidad alta para el cáncer colorrectal, no así para los pólipos del colon. 30Kwakman R et al. 31 señalan en su trabajo que las principales indicaciones de colonoscopia entre los pacientes diagnosticados de cáncer de colon la indicación más frecuente fue la hematoquezia, seguida de anemia, dolor abdominal, rectorragia, sospecha de cáncer de colon, diarrea crónica, sospecha radiológica, síndrome consuntivo, estudio de metástasis hepática, síndrome rectal, tumor abdominal, seguimiento de pólipos y pesquizaje.
Leake I, 32 señala que el dolor abdominal, el cambio del hábito intestinal y la pérdida de peso fueron los síntomas más frecuentes. Laskar RS et al. 33 señalan que las neoplasias distales (colon descendente a recto) pueden presentarse con alteraciones como la disminución del calibre y deposiciones con sangre como hematoquezia, datos que coinciden con lo obtenido en la investigación donde predominó el sangrado digestivo bajo y los síntomas relacionados con la oclusión intestinal.
En el estudio predominó el cáncer en el colon izquierdo, datos que se asemejan a lo encontrado por Karel MJ et al. 34 y Zanella ER et al. 35 donde más de la mitad de los pacientes tamizados presentaron el tumor desde el ciego hasta la mitad del colon transverso.
El adenocarcinoma resultó la variedad histológica más frecuente en la serie de pacientes estudiado. 36,37 En opinión de estos autores los adenocarcinomas constituyen la variedad histológica más común del cáncer de colon, representando alrededor de 95 % de estos. A su vez por el grado de diferenciación, los bien diferenciados predominaron en el estudio, asociados a inflamación crónica, datos que coinciden con lo hallado por Wang L et al. 38
CONCLUSIONES
En la investigación predominaron las mujeres entre 70 y 79 años, de piel blanca y con antecedentes patológicos personales de adenomas vellosos. El sangrado digestivo bajo resultó la forma clínica de presentación más frecuente, y se asoció a localización izquierda. Una parte de los pacientes estudiados requirió intervención quirúrgica y la técnica más empleada fue la hemicolectomía izquierda. La mayor parte de las neoplasias estaban bien diferenciadas, con inflamación crónica y atravesaban la muscular propia sin afectación de los ganglios (Estadio B2 de Astler y Coller). El adenocarcinoma resultó la variante histológica más frecuente. Las complicaciones resultaron pocas y las más frecuentes fueron la hemorragia e infección de la herida quirúrgica.
REFERENCIAS BIBLIOGRÁFICAS
]]> 1.Zhu H, Zhang G, Yi X, Zhu X, Wu Y, Liang J, et al. Histology subtypes and polyp size are associated with synchronous colorectal carcinoma of colorectal serrated polyps: a study of 499 serrated polyps. Am J Cancer Res [Internet]. 2015 Jan [cited 2015 Dec 24];5(1):[about 12 p.]. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4300721/.
2.Zhou L, Xie J, Gu EL, Huang Y, Qu Y, Xu AP, et al. Common genetic variant on BMP4 contributes to colorectal adenoma and cancer: A meta-analysis based on 15 studies. Cytokine [Internet]. 2015 Abr [cited 2015 Dec 24];72(2):[about 9 p.]. Available from: http://www.sciencedirect.com/science/article/pii/S1043466614006541
3.Xie J, Dong H, Chen H, Zhao R, Sinko PJ, Shen W, et al. Exploring cancer metastasis prevention strategy: interrupting adhesion of cancer cells to vascular endothelia of potential metastatic tissues by antibody-coated nanomaterial. J Nanobiotechnology [Internet]. 2015 .[cited 2015 Dec 24];13(9):[about 10 p.]. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4320453/.
4.Vrinten C, Waller J, von Wagner C, Wardle J. Cancer fear: facilitator and deterrent to participation in colorectal cancer screening. Can Epidemiol Biom Prev [Internet]. 2015 [cited 2015 Dec 24];24(2):[about 9 p.]. Available from: http://cebp.aacrjournals.org/content/24/2/400.short
5.Tanday S. Less surgery improves survival for advanced colorectal cancer. Lancet Oncol [Internet]. 2015 Jan [cited 2015 Dec 12];16(3):[about 2 p.]. Available from: http://www.thelancet.com/journals/lanonc/article/PIIS1470-2045%2814%2971202-1/abstract
6.Tamandl D, Butte JM, Allen PJ, D'Angelica MI, DeMatteo RP, Groeger JS, et al. Hospital readmissions after liver surgery for metastatic colorectal cancer. Surgery [Internet]. 2015 Feb [cited 2015 Dec 24];157(2):[about 10 p.]. Available from: http://www.sciencedirect.com/science/article/pii/S0039606014006096
7.Bachmayr-Heyda A, Reiner AT, Auer K, Sukhbaatar N, Aust S, Bachleitner-Hofmann T, et al. Correlation of circular RNA abundance with proliferation - exemplified with colorectal and ovarian cancer, idiopathic lung fibrosis, and normal human tissues. Sci Rep [Internet]. 2015 Jan [cited 2015 Dec 24]; 8057:[about 12 p.]. Available from: http://www.nature.com/articles/srep08057
8.Choe EK, Park KJ, Chung SJ, Moon SH, Ryoo SB, Oh HK. Colonoscopic surveillance after colorectal cancer resection: who needs more intensive follow-up?. Digestion [nternet]. 2015 [cited 2015 Apr 12];91(2):[about 7 p.]. Available from: http://www.karger.com/Article/FullText/370308
9.Crncec I, Pathria P, Svinka J, Eferl R. Induction of colorectal cancer in mice and histomorphometric evaluation of tumors. Methods Mol Biol [Internet]. 2015 [cited 2015 Jan 14];1267:[about 12 p.]. Available from: http://link.springer.com/protocol/10.1007/978-1-4939-2297-0_7#page-1
10.Sugano K, Maeda K, Ohtani H, Nagahara H, Shibutani M, Hirakawa K. Expression of xCT as a Predictor of Disease Recurrence in Patients with Colorectal Cancer. Anticancer Res [nternet]. 2015 Feb [cited 2015 Apr 12];35(2):[about 9 p.]. Available from: http://ar.iiarjournals.org/content/35/2/677.short#
11.Suenaga M, Mizunuma N, Shinozaki E, Matsusaka S, Ozaka M, Ogura M, et al. Anticoagulant therapy for venous thromboembolism detected by Doppler ultrasound in patients with metastatic colorectal cancer receiving bevacizumab. Onco Targets Ther [Internet]. 2015 Feb [cited 2015 Jan 23];8(2):[about 10 p.]. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4315555/.
12.Sturludóttir M, Martling A, Carlsson S, Blomqvist L. Synchronous rectal and prostate cancer - The impact of MRI on incidence and imaging findings. Eur J Radiol [Internet]. 2015 Jan [cited 2015 Nov 23];84(4):[about 12 p.]. Available from: http://www.sciencedirect.com/science/article/pii/S0720048X15000194
13.Ferreira Bohórquez EJ, Meléndez Héctor J. Características clínicas, demográficas e histopatológicas de los pacientes con cáncer colorrectal del Hospital Universitario de Santander. Rev Colomb de Cir [Internet]. Jul-Sep 2012 [citado 23 Oct 2015]; 27(3):[aprox. 12 p.]. Disponible en: http://bases.bireme.br/cgi-bin/wxislind.exe/iah/online/?IsisScript=iah/iah.xis&src=google&base=LILACS&lang=p&nextAction=lnk&exprSearch=657000&indexSearch=ID
14.Montes de Oca Megías E, Soler Porro LL, Noa Pedroso G, Agüero Betancourt CdlM, González Gutiérrez JL, Barreto Suárez E. Comportamiento del cáncer colorrectal esporádico en un hospital provincial. Rev cubana med [Internet]. Oct-Dic 2012 [citado 12 Dic 2015];51(4):[aprox 10 p.]. Disponible en: http://www.imbiomed.com.mx/1/1/articulos.php?method=showDetail&id_revista=68&id_seccion=489&id_ejemplar=9195&id_articulo=94017
15.Neuhouser ML, Cheng TY, Beresford SA, Brown E, Song X, Miller JW, et al. Red blood cell folate and plasma folate are not associated with risk of incident colorectal cancer in the Women's Health Initiative Observational Study. Int J Cancer [Internet]. 2015 Aug [cited 2015 Nov 23];137(4):[about 11 p.]. Available from: http://onlinelibrary.wiley.com/doi/10.1002/ijc.29453/full
16.Liu Z, Zhang Y, Franzin L, Cormier JN, Chan W, Xu H, et al. Trends and variations in breast and colorectal cancer incidence from 1995 to 2011: A comparative study between Texas Cancer Registry and National Cancer Institute's Surveillance, Epidemiology and End Results data. Int J Oncol [Internet]. 2015 Apr [cited 2015 Nov 23];46(4):[about 9 p.]. Available from: http://www.spandidos-publications.com/10.3892/ijo.2015.2881
17.Barrera E, Bannura CG, Illanes FF, Esperguel GC, Melo LC. Resultados precoces de la cirugía electiva del cáncer de colon en mayores de 75 años. Rev Chil Cir [Internet]. Feb 2012 [citado 3 Mar 2016];64(1):[aprox.12 p.]. Disponible en: http://www.scielo.cl/scielo.php?script=sci_arttext&pid=S0718-40262012000100010&lng=es
18.Chacaltana Mendoza A, Rodriguez Ulloa C, Frisancho Velarde O. Valoración de las indicaciones de colonoscopía en la predicción diagnóstica de cáncer de colon. Rev gastroenterol [Internet]. Dic 2011 [citado 3 Mar 2016];31(4):[aprox. 12 p.]. Disponible en: http://www.scielo.org.pe/scielo.php?script=sci_arttext&pid=S1022- 51292011000400009&lng=es&nrm=iso
19.Juliao Baños F, Agudelo Zapata Y, Yepes Delgado C. Variación en el cuidado de pacientes con Enfermedad Inflamatoria Intestinal (EII): resultado de una encuesta. Rev Colomb Gastr [Internet]. Ene-Mar 2014 [citado3 Mar 2016];29(1):[aprox. 8 p.]. Disponible en: http://www.scielo.org.co/pdf/rcg/v29n1/v29n1a03.pdf
20.Ojima T, Nakamori M, Nakamura M, Katsuda M, Iida T, Hayata K, et al. Laparoscopic combined resection of synchronous gastric and colorectal cancer. Surg Laparosc Endosc Percutan Tech [Internet]. 2015 Feb [cited 2015 Nov 23];25(1):[about 9 p.]. Available from: http://journals.lww.com/surgicallaparoscopy/Abstract/2015/02000/Laparoscopic_Combined_Resection_of_Synchronous.11.aspx
21.Ling C, Wang L, Wang Z, Xu L, Sun L, Yang H, et al. A pathway-centric survey of somatic mutations in chinese patients with colorectal carcinomas. PLoS One [Internet]. Jan 2015 [cited 2015 Nov 23];10(1):[about 8 p.]. Available from: http://journals.plos.org/plosone/article?id=10.1371/journal.pone.0116753
22.Loyde KJ De, Harrison JD, Durcinoska I, Shepherd HL, Solomon MJ, Young JM. Which information source is best? Concordance between patient report, clinician report and medical records of patient co-morbidity and adjuvant therapy health information. J Eval Clin Pract [Internet]. 2015 Apr [cited 2015 Nov 23];21(2):[about 7 p.]. Available from: http://onlinelibrary.wiley.com/doi/10.1111/jep.12327/full
23.Eng OS, Melstrom LG, Carpizo DR. The relationship of perioperative fluid administration to outcomes in colorectal and pancreatic surgery: A review of the literature. J Surg Oncol [Internet]. 2015 Mar [cited 2015 Nov 23];111(14):[about 10 p.]. Available from: http://onlinelibrary.wiley.com/doi/10.1002/jso.23857/full
24.Kingham TP, Correa-Gallego C, D'Angelica MI, Gonen M, DeMatteo RP, Fong Y, et al. Hepatic Parenchymal Preservation Surgery: Decreasing Morbidity and Mortality Rates in 4,152 Resections for Malignancy. J Am Coll Surg [Internet]. 2014 Apr [cited 2015 Nov 23];220(4):[about 7 p.]. Available from: http://www.sciencedirect.com/science/article/pii/S1072751514019231
25.Malvezzi M, Bertuccio P, Rosso T, Rota M, Levi F, La Vecchia C, et al. European cancer mortality predictions for the year 2015: does lung cancer have the highest death rate in EU women? Ann Oncol. [Internet]. 2015 Jan [cited 2015 Feb 12];26(4):[about 11 p.]. Available from: https://www.researchgate.net/profile/Matteo_Rota/publication/271595593_European_cancer_mortality_predictions_for_the_year_2015_does_
lung_cancer_have_the_highest_death_rate_in_EU_women/links/5586aa3308aef58c039f13e3.pdf
26.Adams SA, Choi SK, Khang L, D AC, Friedman DB, Eberth JM, et al. Decreased Cancer Mortality-to-Incidence Ratios with Increased Accessibility of Federally Qualified Health Centers. J Community Health [Internet]. 2015 Jan [cited 2015 Mar 7];40:[about 9 p.]. Available from: http://link.springer.com/article/10.1007/s10900-014-9978-8#/page-1
27.Anuario Estadístico de Salud [Internet]. La Habana: Ministerio de Salud Pública .1972-2017 [citado 4 Nov 2017]. Mortalidad por Tumores Malignos según localización. 2015-2016 [aprox. 1 pantalla]. Disponible en: http://bvscuba.sld.cu/anuario-estadistico-de-cuba/.
28.Hano García OM, Wood Rodríguez L, Galbán García E, Abreu Vázquez MdR. Factores de riesgo para el cáncer colorrectal. Rev cubana med [Internet]. Abr-Jun 2011 [citado 12 Dic 2015];50(2):[aprox. 4 p.]. Disponible en: http://scielo.sld.cu/scielo.php?script=sci_arttext&pid=S0034-75232011000200002&nrm=iso
29.Lynch HT, Snyder CL, Shaw TG, Heinen CD, Hitchins MP. Milestones of Lynch syndrome: 1895-2015. Nat Rev Cancer [Internet]. 2015 Feb [citado 2016 Mar 3];15(3):[about 15 p.]. Available from: http://www.nature.com/nrc/journal/v15/n3/abs/nrc3878.html
30.Larkey LK, McClain D, Roe DJ, Hector RD, Lopez AM, Sillanpaa B, et al. Randomized Controlled Trial of Storytelling Compared to a Personal Risk Tool Intervention on Colorectal Cancer Screening in Low-Income Patients. Am J Health Promot Internet]. 2015 Nov-Dic [cited 5 Feb 2015];30(2):[about 3 p.]. Available from: http://www.ncbi.nlm.nih.gov/pubmed/25615708
31.Kwakman R, Cuba EM de, Winter JP de, Hingh IH de, Delis-van Diemen PM, Tijssen M, et al. Tailoring heated intraperitoneal mitomycin C for peritoneal metastases originating from colorectal carcinoma: a translational approach to improve survival. Br J Cancer. [Internet]. 2015 Feb [cited 2016 Mar 3];112:[about 9 p.]. Available from: http://www.nature.com/bjc/journal/v112/n5/abs/bjc201518a.html
32.Leake I. Colorectal cancer: Combining drug therapies to improve treatment efficacy in metastatic colorectal cancer. Nat Rev Gastroenterol Hepatol [Internet]. 2015 Feb [cited 2016 Mar 3];12(121):[about 13 p.]. Available from: http://www.nature.com/nrgastro/journal/v12/n3/full/nrgastro.2015.29.html
33.Laskar RS, Talukdar FR, Choudhury JH, Singh SA, Kundu S, Dhar B, et al. Association of HPV with genetic and epigenetic alterations in colorectal adenocarcinoma from Indian population. Tumour Biol [Internet]. 2015 Feb [cited 2016 Mar 3];36:[about 9 p.]. Available from: http://link.springer.com/article/10.1007/s13277-015-3114-y#page-1
34.Karel MJ, Mulligan EA, Walder A, Martin LA, Moye J, Naik AD. Valued life abilities among veteran cancer survivors. Health Expect [Internet]. 2015 Jan [citado 2015 Mar 3];19(1):[about 11 p.]. Available from: http://onlinelibrary.wiley.com/doi/10.1111/hex.12343/full
35.Zanella ER, Galimi F, Sassi F, Migliardi G, Cottino F, Leto SM, et al. IGF2 is an actionable target that identifies a distinct subpopulation of colorectal cancer patients with marginal response to anti-EGFR therapies. Sci Transl Med [Internet]. 2015 Jan [cited 2015 Mar 20];7(272):[about 8 p.]. Available from: http://stm.sciencemag.org/content/7/272/272ra12.short
36.Ying J, Tsujii M, Kondo J, Hayashi Y, Kato M, Akasaka T, et al. The effectiveness of an anti-human IL-6 receptor monoclonal antibody combined with chemotherapy to target colon cancer stem-like cells. Int J Oncol [Internet]. 2015 Jan [cited 2015 Mar 20];46(4):[about 9 p.]. Available from: http://www.spandidos-publications.com/ijo/46/4/1551?text=fulltext
37.Yin DD, Liu ZJ, Zhang E, Kong R, Zhang ZH, Guo RH. Decreased expression of long noncoding RNA MEG3 affects cell proliferation and predicts a poor prognosis in patients with colorectal cancer. Tumour Biol [Internet]. 2015 Feb [cited 2015 Mar 20];36:[about 13 p.]. Available from: http://link.springer.com/article/10.1007/s13277-015-3139-2#page-2
38.Wang L, Shen X, Wang Z, Xiao X, Wei P, Wang Q, et al. A molecular signature for the prediction of recurrence in colorectal cancer. Mol Cancer [Internet]. 2015 Feb [cited 2015 Mar 20];14(22):[about 7 p.]. Available from: http://molecular-cancer.biomedcentral.com/articles/10.1186/s12943-015-0296-2
Recibido: 11 de diciembre de 2017
Aprobado:3 de marzo de 2018
Dr. Luis Andrés Guibert Adolfo. Especialista de I Grado en Medicina General. Especialista de I Grado en Cirugía General. Profesor Instructor. Hospital Militar Clínico Quirúrgico Docente Dr. Octavio de la Concepción de la Pedraja. Universidad de Ciencias Médicas de Camagüey. Camagüey, Cuba. Email: luis.cmw@infomed.sld.cu
]]>