Case Presentation
Aesthetic and functional rehabilitation using triamcinolone on patient suffered by facial firework injury
Rehabilitación de trauma facial ocasionado por fuegos artificiales utilizando triamcinolona
0000-0002-0381-9543Anne Caroline Gercina Carvalho Dantas
1
*
, 0000-0003-4693-1356Klinger de Souza Amorim
2
, 0000-0002-5961-2074Albert Vinícius Barboza Santana
1
, 0000-0002-8556-0546Rangel Cyrilo Lima de Melo
1
, 0000-0003-3012-0049Vanessa Tavares da Silva Fontes
1
, 0000-0003-0651-5470Liane Maciel de Almeida Souza
1
1Universidade Federal de Sergipe, Departamento de Odontologia. Aracaju, Brasil.
2Universidade Estadual de Campinas, Departamento de Farmacologia, Anestesiologia e Terapêutica. Piracicaba, Brasil.
ABSTRACT
Introduction:
Facial injuries are a common occurrence at the emergency room. Treatment for this type of trauma is complex in terms of re-establishing good oral and facial function, plus aesthetics. Objective: This paper aims to report a clinical case of aesthetic and functional rehabilitation using triamcinolone in a patient affected on the face by a fireworks explosion.
Case report:
A 26-year-old man was admitted to the oral and maxillofacial surgery service of the Sergipe Urgency Hospital presenting trauma after the explosion of a “Firework rocket” in his face. The patient had extensive soft tissue injury in gingival mucosa, right labial commissure, and tongue. There was also inferior incisive avulsion and dentoalveolar fracture. His clinical and tomographic evaluation presented comminuted mandibular fracture. After eighteen days he was discharged and sent to the dentistry service of the Federal University of Sergipe for aesthetic and functional rehabilitation of his facial damages. Two months later, the patient attended a University dental service to begin aesthetic and postoperative functional rehabilitation. First, the necrotic bone was removed, following intralesional infiltration of hexacetonide triamcinolone 20mg/mL into the scar of the labial region and the commissure of the lips was performed. Each application was performed after twenty days of interval. Later, lingual frenectomy and glossosplasty were done for improving his lingual mobility and then hexacetonide triamcinolone 20mg/mL infiltrations were also done in the tongue base in the following sessions.
Conclusions:
After five infiltrations, it was observed an improvement in the scar appearance and texture, which also had a lower contracture, as well as a lingual motricity improvement.
Key words: Injuries; maxillofacial; Cicatrix; Hypertrophic; Triamcinolone
RESUMEN
Introducción:
Las lesiones faciales son frecuentes en el servicio de emergencia. El tratamiento para este tipo de trauma es complejo en términos de restablecer una buena función bucal y facial, además de la estética.
Objetivo:
Reportar un caso clínico de rehabilitación estética y funcional a través del uso de hexacetónido de triamcinolona en un paciente afectado por una explosión de fuegos artificiales en su rostro.
Caso clínico:
Hombre de 26 años ingresado en el servicio de cirugía oral y maxilofacial del Hospital de Urgencia de Sergipe por presentar un traumatismo después de la explosión contra su rostro de un cohete de fuegos artificiales. El paciente tenía una lesión extensa de partes blandas en la mucosa gingival, comisura labial derecha y lengua. También hubo avulsión incisiva inferior y fractura dentoalveolar. A través de la evaluación clínica y de tomografía, fue posible observar fragmentación múltiple ósea en el sitio de la fractura, compatible con fractura mandibular conminuta. Después de dieciocho días fue dado de alta y enviado al servicio de odontología de la Universidad Federal de Sergipe para la rehabilitación estética y funcional de sus daños faciales. Dos meses después, el paciente asistió al servicio dental de la universidad para comenzar la rehabilitación funcional estética y posoperatoria. Primero, se retiró el hueso necrótico, luego se realizó la infiltración intralesional de hexacetónido de triamcinolona 20 mg/mL en la cicatriz de la región labial y se realizó la comisura de los labios; con un intervalo de 20 días entre cada aplicación. Posteriormente, se realizaron frenectomía lingual y glososplastia, para mejorar su movilidad lingual, y luego se realizaron infiltraciones de 20 mg/mL de hexacetónido de triamcinolona en la base de la lengua en las sesiones siguientes.
Comentarios principales:
Después de cinco infiltraciones se observó una mejora en el aspecto y la textura de la cicatriz, que también tenía una contractura más baja, así como una mejora de la motricidad lingual.
Palabras-clave: lesiones maxilofaciales; cicatriz hipertrófica; triamcinolona
Introduction
Facial injuries are of common occurrence on emergency entrances which depending on its severity, it can trigger aesthetic and functional damages.1,2
Usually, car accidents and urban or domestic violence are the main causes of oral and maxillofacial trauma.3,4) However, other causes such as fireworks can promote potentially dangerous facial trauma.
Treatment for maxillofacial trauma is complex in terms of re-establishing good oral and facial function, plus aesthetics. The extent of soft tissue injury results in extensive healing areas.5) Some scars result in physical limitations to basic functions such as eating or even speaking. Additionally, it may be found emotionally unpleasant and sometimes stigmatizing sequels to the affected patient. Thus, improving a function and esthetics related to post-traumatic healing are important steps in the rehabilitation of patients who have faced facial trauma.6
This paper aims to report a clinical case of aesthetic and functional rehabilitation using triamcinolone in a patient affected on his face by a fireworks explosion.
Case report
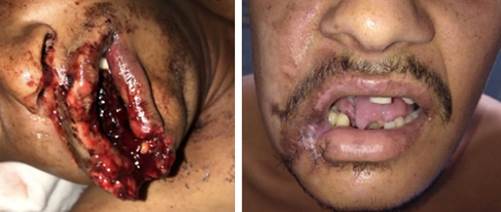
A 26-year-old man was admitted to the oral and maxillofacial surgery department of the Sergipe Urgency Hospital, Aracaju, Brazil, presenting trauma after the explosion of a “firework rocket” in his face. The patient had extensive soft tissue injury, loss of gingival mucosa, and wide laceration in his tongue and labial commissure of right side. There was also avulsion of inferior incisive teeth 24, 25 and 26 (Universal Numbering Sytem) and dentoalveolar fracture of 22, 23 and 27 (Fig. 1A).
The patient was conscious and responded to verbal stimuli, however, due to the extent of the injuries he was unable to speak. The clinical and tomographic evaluation presented comminuted mandibular fracture in symphysis and parasyphysis region. Immediately after diagnosis, the patient entered the operating room. Due to excessive bleeding, it was not possible to perform endotracheal intubation, for this reason, a tracheostomy was performed.
During surgery necrotic tissue debridement and bleeding control were executed while surgical procedures. Afterward, fracture reduction, and immobilization through odontosynthesis using Erich bar and steel wire were also performed. Furthermore, three titanium mini plates, 2.0 mm system were used on bone segments rigid fixation.
After fractures stabilization, the flaps were rotated and the wounds closed, as much as were possible since there was considerable loss of tissue. It was also performed, glossorafia and vestibular mucosa suture, as well as, inferior labial reconstruction. It was prescribed Cefazolin 1g every 8 hours, Dipyrone 1g every 6 hours, Ranitidine 50mg every 12 hours every day in the first week and Dexamethasone 10mg every 12 hours for 3 days, besides, he had the diet through the nasogastric tube and routine cares.
After seven days postoperative, it was noticed a volume increase in the region, plus sialorrhea and halitosis, which suggests an infectious condition 08 hours with rigorous oral hygiene with 0.12% Chlorhexidine associated.
This therapy was maintained for one more week, until the infectious condition remission. Then it began the tracheostomy weaning to total obliteration and removal of the tracheostomy tube. Nevertheless, the patient still presented a limitation on tongue motricity and speech due to the loss of substance. Moreover, bone exposure ocurred followed by the reconstruction plate exposure in the mandibular symphysis region caused by soft tissue retraction and the previous infection (Fig. 1B). The patient was discharged on the eighteenth day and sent to the Federal University of Sergipe dental service for aesthetic and functional rehabilitation of the facial damages.
Two months later, the patient attended the dental service at University dental service to begin aesthetic and postoperative functional rehabilitation. At the clinical examination, there was extensive hypertrophic and fibrotic scarring in the labial region, aesthetic defect in the region of the right labial commissure, and bone sequestration in the anterior part of the mandible. There was also a limitation of the lingual motricity due to the loss of substance and the glossorafia consequence, occasioning swallowing and speech difficulties.
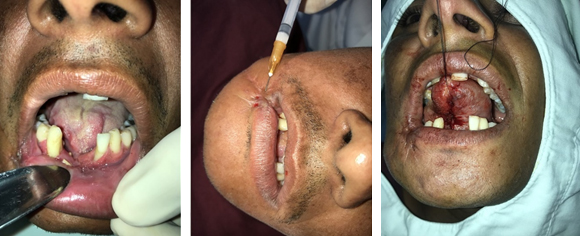
First, the necrotic bone was removed, the next intralesional infiltration of hexacetonide triamcinolone 20mg/mL into the scar of the labial region and the commissure of the lips was performed.
Each application was performed after twenty days of interval. Later, lingual frenectomy and glossosplasty were done to improve lingual mobility and the hexacetonide triamcinolone 20 mg/mL infiltrations were also performed in tongue base in the following sessions (Fig. 2).
After five infiltrations, it was observed an improvement in the scar appearance and texture, which also had a lower contracture, as well as a lingual motricity improvement.
The patient was then referred for rehabilitation with removable partial denture prosthetics (Fig. 3).
Discussion
Maxillofacial lesions can contribute to posttraumatic psychological consequences such as anxiety and depression, substance abuse or addiction, or posttraumatic stress disorders.7 This occurs mainly in injuries related to facial trauma and scars, leading to a social and functional impact. As can be seen in a study, which identified the prevalence of posttraumatic psychological symptoms following maxillofacial trauma among an Indian population sample and changes in these symptoms over a while.8 It revealed the abnormal psychological response to maxillofacial trauma included emotional distress, anxiety, and depression in immediate and follow-up periods. Besides, it is possible to observe a significantly higher unemployment incidence, and conjugal problems.9,10) Then, it is important to think of a treatment that involves from the beginning of the facial trauma treatment to the functional, aesthetic and social rehabilitation.
Numerous methods have been described for abnormal scars treatment. However, at the moment, the ideal type of treatment has not yet been established. These include surgical excision with or without grafting, and non-surgical pressure therapies, intralesional interferon, topical and intralesional corticosteroids, bleomycin sulfate, 5-fluorouracil (5-FU), laser therapy, and other therapies directed at collagen synthesis.11,12,13,14,15,16 Intralesional corticoids are considered to be the most common and predictable type of treatment and have been used in the hypertrophic keloids and scars treatment since 1960.13 The patient presented a fibrous and hypertrophic scar that resulted in labial and commissure asymmetry. Due to the explosive trauma amplitude, this patient ended up losing labial substance, hence, it was not considered surgical excision as treatment.
Triamcinolone can inhibit the vascular endothelial growth factor (VEGF) expression, fibroblast proliferation resulting in scar tissue atrophy, which might be the main mechanism of its effectiveness.14 Glucocorticoids can inhibit wound inflammation, reduce collagen and mucopolysaccharide synthesis, as well as inhibit fibroblast growth, and accelerate collagen and fibroblasts degeneration. Triamcinolone acetonide has been proven to prevent the expression of transforming growth factor-beta (TGF-β1) and induces fibroblasts apoptosis.15
Glucocorticoids are involved in organism physiological processes, and their effects can be accompanied by side effects such as pain, skin and subcutaneous tissues atrophy, development of steroid acne, angiotelectasis, a menstrual disorder in women, hyperpigmentation and depigmentation.14) More serious adverse reactions include local skin necrosis, ulceration and anaphylaxis are linked to a very high dose of the drug.17
There is still no consensus on the optimal dosage of triamcinolone in the scars treatment and the time interval between applications, there is also a non-consensus about the ideal dose should be used.16) Furthermore, one of the commercially available concentrations of triamcinolone is 20mg / ml. This dose of 20mg / mL was used in this case report following a 20-day interval based on the pharmacokinetics of the drug, which forms a local depot and produces its effect for 21 days on average.18,19 The patient did not present any adverse reactions during the whole treatment. The absence of collateral effects in this report may occur because the treatment has not been prolonged for more than five sessions, as well as the use of a non-excessive high dose of triamcinolone. This suggests the need for further studies regarding the effect of the use of triamcinolone at this and other dosages on controlled randomized clinical trials to a better understanding and demonstration of the triamcinolone effects on hypertrophic scars.
Conclusions
Triamcinolone local infiltration was effective when used to decrease the scar contraction and improvement on its visual appearance. Therefore, it can be utilized in the rehabilitation of post-trauma patients, aiming at both recovery of functionality and aesthetic improvement, contributing in an essential way to social inclusion.
References
1.
Lalloo R, Lucchesi LR, Bisignano C, Castle CD, Dingels Z V, Fox JT, et al1.
. Epidemiology of facial fractures: incidence, prevalence and years lived with disability estimates from the Global Burden of Disease 2017 study. Inj Prev. 2020 [access: 27/03/2020]; 26(Supp 1):i27-i35. Available from: Available from: http://www.ncbi.nlm.nih.gov/pubmed/31915268
1.
[ Links ]
2.
Zamboni RA, Wagner JCB, Volkweis MR, Gerhardt EL, Buchmann EM, Bavaresco CS. Epidemiological study of facial fractures at the Oral and Maxillofacial Surgery Service, Santa Casa de Misericordia Hospital Complex, Porto Alegre - RS - Brazil. Rev Col Bras Cir. 2017 [access: 27/03/2020]; 44(5):491-7. Available from: Available from: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S010069912017000500491
2.
[ Links ]
3.
Conceição LD, da Silveira IA, Nascimento GG, Lund RG, da Silva RHA, Leite FRM. Epidemiology and Risk Factors of Maxillofacial Injuries in Brazil, a 5-year Retrospective Study. J Maxillofac Oral Surg. 2018 [access: 27/03/2020]; 17(2):169-74. Available from: Available from: http://link.springer.com/10.1007/s12663-016-0994-3
3.
[ Links ]
4.
Xiao-Dong L, Qiu-Xu W, Wei-Xian L. Epidemiological pattern of maxillofacial fractures in northern China. Medicine (Baltimore). 2020 [access: 27/03/2020]; 99(9):1-7. Available from: Available from: http://journals.lww.com/10.1097/MD.0000000000019299
4.
[ Links ]
5.
Gao H, Wang W, Geng Y, Shao Y. Clinical Experience in Emergency Management of Severe Facial Trauma. J Craniofac Surg. 2020 [access: 27/03/2020]; 31(2):121-3. Available from: Available from: http://journals.lww.com/10.1097/SCS.0000000000006010
5.
[ Links ]
6.
Ardeshirpour F, Shaye DA, Hilger PA. Improving Posttraumatic Facial Scars. Otolaryngol Clin North Am. 2013 [access: 27/03/2020] ;46(5):867-81. Available from: Available from: https://www.ncbi.nlm.nih.gov/pubmed/24138743
6.
[ Links ]
7.
Choudhury-Peters D, Dain V. Developing psychological services following facial trauma. BMJ Qual Improv Reports. 2016 [access: 27/03/2020]; 5(1):1-7. Available from: Available from: http://qir.bmj.com/lookup/doi/10.1136/bmjquality.u210402.w4210
7.
[ Links ]
8.
Krishnan B, Rajkumar RP. Psychological Consequences of Maxillofacial Trauma in the Indian Population: A Preliminary Study. Craniomaxillofac Trauma Reconstr. 2018 [access: 27/03/2020]; 11(3):199-204. Available from: Available from: http://journals.sagepub.com/doi/10.1055/s-0037-1604426
8.
[ Links ]
9.
Islam S, Ahmed M, Walton GM, Dinan TG, Hoffman GR. The prevalence of psychological distress in a sample of facial trauma victims. A comparative cross-sectional study between UK and Australia. J Cranio-Maxillofacial Surg. 2012 [access: 27/03/2020]; 40(1):82-5. Available from: Available from: https://linkinghub.elsevier.com/retrieve/pii/S1010518211000308
9.
[ Links ]
10.
Levine E, Degutis L, Pruzinsky T, Shin J, Persing JA. Quality of Life and Facial Trauma. Ann Plast Surg. 2005 [access: 27/03/2020]; 54(5):502-10. Available from: Available from: https://insights.ovid.com/crossref?an=00000637-200505000-00010
10.
[ Links ]
11.
Aggarwal A, Ravikumar BC, Vinay KN, Raghukumar S, Yashovardhana DP. A comparative study of various modalities in the treatment of keloids. Int J Dermatol. 2018 [access: 08/07/2019]; 57(10):1192-200. Available from: Available from: http://www.ncbi.nlm.nih.gov/pubmed/29993130
11.
[ Links ]
12.
Lee H, Jang Y. Recent Understandings of Biology, Prophylaxis and Treatment Strategies for Hypertrophic Scars and Keloids. Int J Mol Sci. 2018 [access: 27/03/2020]; 19(3):711. Available from: Available from: http://www.mdpi.com/1422-0067/19/3/711
12.
[ Links ]
13.
Muneuchi G, Suzuki S, Onodera M, Ito O, Hata Y, Igawa HH. Long-term outcome of intralesional injection of triamcinolone acetonide for the treatment of keloid scars in Asian patients. Scand J Plast Reconstr Surg Hand Surg. 2006 [access: 22/02/2019]; 40(2):111-6. Available from: Available from: http://www.ncbi.nlm.nih.gov/pubmed/16537259
13.
[ Links ]
14.
Koc E, Arca E, Surucu B, Kurumlu Z. An Open, Randomized, Controlled, Comparative Study of the Combined Effect of Intralesional Triamcinolone Acetonide and Onion Extract Gel and Intralesional Triamcinolone Acetonide Alone in the Treatment of Hypertrophic Scars and Keloids. Dermatologic Surg. 2008 [access: 27/03/2020]; 34(11):1507-14. Available from: Available from: http://doi.wiley.com/10.1111/j.1524-4725.2008.34314.x
14.
[ Links ]
15.
Song H, Tan J, Fu Q, Huang L, Ao M. Comparative efficacy of intralesional triamcinolone acetonide injection during early and static stage of pathological scarring. J Cosmet Dermatol. 2019 [access: 27/03/2020]; 18(3):874-8. Available from: Available from: https://onlinelibrary.wiley.com/doi/abs/10.1111/jocd.12690
15.
[ Links ]
16.
Khalid FA, Mehrose MY, Saleem M, Yousaf MA, Mujahid AM, Rehman SU, et al16.
. Comparison of efficacy and safety of intralesional triamcinolone and combination of triamcinolone with 5-fluorouracil in the treatment of keloids and hypertrophic scars: Randomised control trial. Burns. 2019 [access: 08/07/2019]; 45(1):69-75. Available from: Available from: https://linkinghub.elsevier.com/retrieve/pii/S0305417918306983
16.
[ Links ]
17.
Laisuan W, Wongsa C, Dchapaphapeaktak N, Tongdee M, Chatmapanrangsee J, Rerkpattanapipat T. Anaphylaxis following intralesional triamcinolone acetonide (Kenacort) injection. Asia Pac Allergy. 2017 [access: 27/03/2020]; 7(2):115-8. Available from: Available from: https://synapse.koreamed.org/DOIx.php?id=10.5415/apallergy.2017.7.2.115
17.
[ Links ]
18.
Carvalhaes Mandello S, Petroianu A, TCBC- MG, Tostes Ferreira MA, Magalhães Barros V , Lopes RV. Avaliação do tratamento de queloide do lóbulo da orelha com infiltração de triancinolona, retirada cirúrgica e compressão da cicatriz. Rev Col Bras Cir . 2015 [access: 28/02/2019]; 42(1):9-13. Available from: Available from: http://www.scielo.br/pdf/rcbc/v42n1/pt_0100-6991-rcbc-42-01-00009.pdf
18.
[ Links ]
19.
Santos JMP dos, Souza C de, Vasconcelos AC de, Nunes TA, Santos JMP dos, Souza C de, et al19.
. Effect of triamcinolone in keloids morphological changes and cell apoptosis. Rev Col Bras Cir . 2015 [access: 28/02/2019]; 42(3):171-4. Available from: Available from: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S010069912015000400171&lng=en&tlng=en
19.
[ Links ]