Introduction
The «lumbar hernia (LH) is a posterolateral body wall hernia where the bowel, omentum, or pre-peritoneal fat herniates through the lumbar triangles».1
It was initially described by P. Barbette in the year 1672 and later on R.J.C. Garangeot published the first case in 1731.2 The incidence is greater among males aged 50-70 years.1 Most of the LH are acquired primary hernias, however the defect may be congenital or acquired.3
Moreno-Egea et al.4 created a therapeutic classification system to identify the four types of LH. It has six classification criteria which include: size, location, contents, muscular atrophy, origin, and the existence of the previous recurrence.
LHs can occur in two well-defined areas in the lumbar region: the inferior lumbar triangle (Petit's triangle), and the superior lumbar triangle (Grynfelt-Lesshaft's triangle).5 The «Grynfeltt-Lesshaft triangle limits laterally by the inferior oblique muscle, the floor of the transversalis fascia, the medial border of the quadratus lumborum, and superiorly by the 12th rib».1,2,5,6
There is an increased incidence of traumatic etiology. The advances in the available diagnostic methods are very helpful for the diagnosis of LHs in the current medical practice.2 However, they have been misdiagnosed as lipomas, muscle strains, fibromas, abscesses, and kidney tumors. Each misdiagnosed LH is a cause of increased morbidity.1
A LH may present in patients as an asymptomatic lumbar mass. A lumbar mass with back pain and a lumbar mass with non-significant abdominal symptoms are other forms of presentation.3
A case of primary superior lumbar hernia in a teenager patient with no previous history of diseases is presented. This is the first time that this entity is reported as a medical issue in a patient under 20 years old.
So the objective of this work is to specify the keys for the diagnosis of acquired Grynfeltt-Lesshaft hernia.
Case presentation
A 14-year-old African-American male patient coming from an urban area presented to the pediatric hospital with no previous history of diseases. He complained of a swelling, occasionally painful, located on the left side of the lumbar region. This swelling increased with active movements and disappeared on prone position (Figure 1). The patient’s mother reported that she had noticed this swelling 7 years ago and that two years before the consultation it was diagnosed as a lipoma by his family doctor.
On physical examination, a 7 cm x 7 cm mass was found over the lumbar area. The soft mass reduced when manually compressed and protruded painfully when the patient coughed. The mass was located horizontally between the 10th and 11th ribs, and vertically between the paraspinal muscles and the external oblique muscle.
An X-ray was performed to search for fractures or any abnormality at this level, but they were not found. The CT scan revealed the existence of a superior LH over the left side (Figure 2). The laboratory tests performed did not show any relevant results.
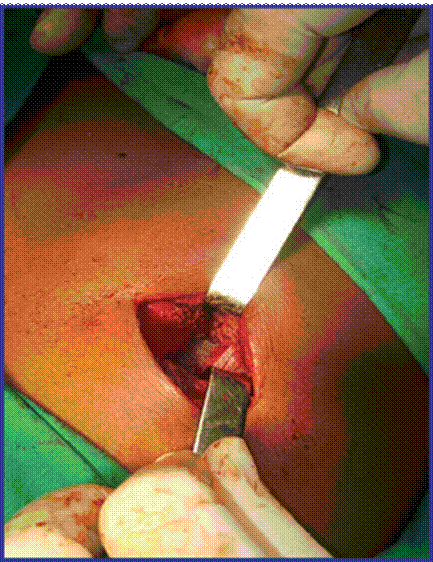
The patient was surgically treated two months after the first evaluation carried out at the initial consultation. The surgical approach used was a transverse incision over the tumour for lumpectomy where a small ring of 1cm x 1cm containing the herniated tumor composed of preperitoneal fat was found; no sac was described. (Figure 3).
The contents were reduced and the ring was closed by approximating its edges with independent sutures of Assufil 2.0; prolonged absorption was reinforced with a polyester fibre prosthetic mesh fixed with U sutures of Prolene 2.0 (Figure 4).
Penrose drainage and independent sutures were placed to ensure the closure of the plans up to the skin. No immediate postoperative complications were observed. The patient was discharged from hospital five days after the procedure. A year after the surgery, the patient was consulted again but he did not report any suggestive symptoms of LH and there were no tenderness or recurrence on physical examination.
Discussion
Patients may complain of backache or a painful area over a herniated tumor. The finding at palpation and the swelling that disappears in prone position are current findings on LHs,7 as in this case. The patient presented to the outpatient clinic with no emergency condition; this is due to the fact that most of the patients present to health care centers with non-emergency conditions and only 9% of them present with surgical emergencies.2
LHs are classified as congenital or acquired. An acquired LH is a primary or a secondary hernia, according to the case. Secondary LH may be of traumatic or post-surgical etiology, including flank incisions, renal surgery and other conditions. The estimation of secondary lumbar hernia reaches the 25 % of all acquired hernias.7
This diagnosis corresponds to an acquired primary superior LH that was initially described as a lipoma. This fact may be related to a misdiagnosis of a LH as a lipoma or other medical conditions.7 It is necessary to refer those cases of a superior lumbar mass to a secondary level of care so that a deeper evaluation can be made. As reported in the literature, X-rays are not the imaging test of choice for the diagnosis of a LH. The CT scan is the principal method for the diagnosis of LH.2
The surgical repair of the hernia is the ideal choice. The classical technique is as good as the laparoscopic technique, although the second procedure will have better outcomes. There is no real consensus about the best method of repairing a LH due to its low incidence.8 Synthetic meshplasty is the most used among open repairs combined with muscle flaps,7 this case only required the use of synthetic meshplasty for repairing the defect as there were no others issues such as a herniated sac with abdominal organs in its interior or a bigger ring that needed muscle flaps.
The open surgical technique proved to be effective a year after the surgery. Younger patients have increased levels of tissue formation;9 but as younger patients are more active which may affect the recurrence of LH or postoperative complications. The operated patient followed a strict schedule in the postoperative phase that did not involve the practice of intensity exercises during the recovery; this fact helped to reduce the probability of recurrence.
Conclusions
The Grynfelt-Lesshaft hernia is a rare surgical condition caused by a congenital or acquired etiology. A low backache or a located point of pain over the hernia in addition to a lumbar mass that reduces in prone position suggests the diagnosis of LH. The available advances in diagnostic methods allow us to easily identify a Grynfelt-Lesshaft hernia in younger patients. Hernia might be identified early from the analysis of the patient’s complaints, considering an increase in size at the lumbar area that disappears in prone position and increases during the Valsalva maneuver.